

Designing a Framework for the Delivery of Collaborative
Musculoskeletal Care Involving Chiropractors and
Physicians in Community-based Primary CareThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: J Interprof Care. 2010 (Nov); 24 (6): 678–689 ~ FULL TEXT
Silvano Mior, Jan Barnsley, Heather Boon, Fredrick D. Ashbury, & Robert Haig
Department of Research,
Canadian Memorial Chiropractic College,
Toronto, Canada.
Strategies have been proposed to facilitate collaboration between conventional health care providers in primary care. However, little is known if these are transferable to CAM health care providers. We designed a qualitative study to articulate a conceptual model to advance the interprofessional collaboration between physicians and chiropractors within community-based primary care in Ontario, Canada. Data obtained from 16 key informants and eight focus groups, with a range of professionals including chiropractors, physicians and academia as well as patients, informed the development our framework.
The framework included processed-based factors that clustered under three categories: communication, practice parameters, and service delivery; presumed necessary to address challenges and optimize benefits of collaboration. The development of this framework may help understand and promote interprofessional collaborative practice and contribute to the understanding of how CAM may participate in mainstream healthcare.
KEYWORDS: Interprofessional collaboration, trust, patient-centeredness, chiropractic, primary care
From the FULL TEXT Article:
Introduction
Today's focus on collaborative patient-centered care reinforces the importance of interprofessional work as a way to optimize intellectual resources and enhance patient and health outcomes (Barrett, Curran, Glynn, & Godwin, 2007). However collaborative care is not easily achieved because of its inherent complexities and dynamic nature (D'Amour, Ferrada-Videla, Rodrigues & Beaulieu, 2005). Theoretical frameworks have been proposed to facilitate understanding of successful collaboration (e.g., Oandasan, Baker, Barker, Bosco, D'Amour et al., 2006; Orchard, Curran, & Kabene, 2005; San Martin-Rodriguez, Beaulieu, D'Amour, & Ferrada-Videla, 2005) but the first step is to identify the objective of, and strategies to achieve, such collaboration (Kailin, 2001). We present findings from a qualitative study designed to articulate a conceptual framework to facilitate an opportunity to advance collaboration between physicians and chiropractors in the delivery of musculoskeletal care within community-based primary care.
Chiropractors are one of the most frequently accessed regulated, non-physician provider groups, who are commonly seen for musculoskeletal conditions (MSC) (Balon & Mior, 2004). Despite their presumed recognition and reported acceptance (Theberge, 2007), their inclusion into mainstream has met with limited success (Kelner, Wellman, Boon & Welsh, 2004; Myburgh, Hartvigsen & Grunnet-Nilsson, 2008; Weeks, 1997). Social scientists have suggested that this limited success may be created by tensions between chiropractors seeking to enhance their role in mainstream (secondary legitimacy) (Myburgh et al., 2008) and mainstream wishing to protect its dominant position and maintain jurisdictional boundaries (Kelner et al., 2004). Others noted that barriers limiting chiropractors' inclusion have included provider competition, philosophical differences, physicians' lack of knowledge about chiropractic interventions, perceived limited evidence in support of clinical efficacy, professional bias and prejudice, and lack of funding for services (Astin, Marie, Pelletier, Hansen, & Haskell, 1998; Kelner et al., 2004).
Collaboration in primary care has been successfully achieved between physicians and allied health professionals (e.g., psychiatry, social work, and nursing) (Nolte, 2005; Oandasan et al., 2006). Such collaboration reportedly can enhance the continuity and quality of care (Nolte, 2005). However, little is known which strategy can be used to facilitate collaboration between physicians and CAM providers (Frenkel & Borkan, 2003; Greene, Smith, Allareddy, & Haas, 2006). We conducted a study to develop a framework that could be implemented to facilitate the collaboration between chiropractors and physicians in community-based primary care. We asked two main questions: What are the challenges, benefits and opportunities of chiropractic-physician collaboration? And what are the specific factors or activities that would help promote collaboration?
Method
The grounded theory research method (Charmaz, 2000; Glaser & Strauss, 1967) was used to design this study. The intent of grounded theory is to aid researchers to generate an abstract schema of a specific phenomenon, such as a theoretical framework, from naturalistic data (Creswell, 1998). The study had two distinct phases: (i) key informant interviews and focus groups in which we explored participants' meaning of the nature of the interprofessional relationship and the factors that would enable a successful collaboration between the providers; and (2) confirmatory focus groups where we presented the evolving conceptual framework to participants for critique and refinement. The Research Ethics Committees of the University of Toronto and of the Canadian Memorial Chiropractic College approved the study.
Sampling and data collection
The phase 1 key informant interviews were conducted first to identify key issues that might influence the building and maintenance of a collaborative relationship. A total of 16 key informants were purposefully sampled from across North America because of their expertise and influential status in primary health care practice, research or health policy. These opinion leaders came from academia (n = 3), administration (n = 1), chiropractic (n = 5), medicine (n = 4), midwifery (n = 1), nursing (n = 3) and physiotherapy (n = 1). The key informants were selected to maximize variation (Cameron et al., 1997) and were also encouraged to suggest others who could provide additional information (snowball sampling). An open-ended interview guide was created from a literature review and research team discussions; however, key informants were free to add their own personal thoughts and comments. Each key informant interview lasted about 1 hour.

Table I Phase 1 focus groups were used to explore the unique factors identified by the key informants but within the context of the particular community where the collaboration between physicians and chiropractors might occur. Focus group participants in phase 1 were selected from two primary care networks (PCNs) that had expressed interest in interprofessional collaboration with local chiropractors. A PCN was made up of a number of family physicians linked by a common administrative structure, but not necessarily located in the same physical setting. Eight focus groups were held, four at each PCN site. The first group was composed of the physicians in the PCN; the second of a group of chiropractors practicing in close proximity to the PCN; the third group was of patients recruited from PCN physicians' offices, but who had not previously seen a chiropractor; and the fourth group was of patients recruited from both the physicians' and chiropractors' offices who were receiving chiropractic care. Approximately 10–12 individuals were invited to each focus group to accommodate for potential drop-outs (Krueger, 1998), with 62 participating (see Table I).
Focus groups were led by a research team member with experience in group facilitation. A second team member, a chiropractor, attended and prepared field notes, as well as provided answers to professional or technical questions. The focus group guides were developed from insights gained from the key informant data and literature reviews. The focus groups lasted about 2.5 hours.
In phase 2, two additional focus groups were held to refine the emerging conceptual framework developed from the data collected in phase 1. One of these confirmatory focus groups was held at each of the two PCN sites. Each group was composed of two chiropractors and two physicians, who were selected from the previous focus groups and who were seen as "championing" the idea of a collaborative model. The groups met for 2 hours.
All interviews and focus group sessions were audio taped and transcribed verbatim, with the participants' consent. Each transcript was checked for accuracy by two research team members; errors in content and sentence structure were corrected and extraneous comments or sounds (e.g., laughter) noted. Transcripts were not returned to participants for review.
Data analysis
In both phases, each transcript was independently analyzed by two members of the research team using the constant comparison method (Strauss & Corbin, 1998). The data were examined for meaningful phrases, sentences or paragraphs and compared for similarities and differences. Open coding was used to identify categories and sub-categories. Team research meetings were convened to discuss and harmonize the individual interpretations until consensus was reached on the themes, categories and sub-categories. The coding structure and the related transcript reference data were entered into qualitative data analysis software, which facilitated the handling and retrieval of data and quotes (NVivo Version1.1, QSR International Pty. Ltd., Melbourne).
The analysis proceeded in an iterative and inductive manner in which analysis of early interviews and focus groups informed later data collection. The analysis of phase 1 was focused on the development of a conceptual framework that was "grounded" in the participants' perceptions and experiences that could be used to guide and support collaboration between chiropractors and physicians. The framework was generated over many team meetings using axial coding methods to identify how the open codes were related to our central phenomenon (collaboration) and each other (Creswell, 1998). The analysis in phase 2 was focused on refining the conceptual framework that evolved from phase 1.
Results
Participants use of, and meanings attributed to, specific terminology provided a context for the development of the conceptual framework discussed below. Participants viewed integration as a more formal relationship where different health care professionals were subsumed under a common policy, administration, formal structure, and sharing a common vision of care delivery. Alternatively, collaboration was described as health care providers working together but maintaining their autonomy in the absence of formal structure and processes for the delivery of patient care.
Two different types of individuals were recognized as responsible for the success and sustainability of collaborative relationships. A "leader" was perceived as an enabler of the collaborative relationships (e.g., ensured the necessary resources and incentives were provided). A "champion" was someone who facilitated and was responsible for the day-today interactions and planning. This distinction was considered to be important when developing strategies for program implementation.
Development of our collaborative framework
Two emergent themes, "trusting relationships" and "patient centeredness", provided the context for the conceptual framework. According to study participants, successful collaboration must be built on trust. This trusting relationship must be developed between, and sustained by, the patient (Pt), the chiropractor (DC), and the physician (MD). This was particularly evident amongst patients with no prior chiropractic experience, for example:I need that physician/chiropractor trust in the collaboration...
( Patient, focus group 6:454).The fundamental issues that positively or negatively affected the development of a trusting relationship included the lack of knowledge about or negative experiences, real or perceived, with both provider groups. In particular, among patients and physicians, negative chiropractic experiences included perceived provision of inappropriate care; the negative image of the chiropractic profession because of the actions of one its members or as promulgated by the public, media or other health care professionals; and differences in philosophy and scope of practice:
It is an issue of credibility and education. Most medical students never have a chance
to see a chiropractor in their entire education.
( Physician, interview 1: 80)
And you never hear the positive side. I don't recall seeing 60 Minutes doing chiropractors are great...
So it is extreme stories but never good extremes, always bad.
( Patient, focus group 5: 352).A second emergent theme advocated for a patient-centered focus. This focus reinforced the ideas that collaboration would enable patient participation in clinical decision making and management, and be respectful of patient choice. It would focus the collaboration on the patient rather than the personal or professional preferences of providers:
the patient is really the most potent integrator of health care.
( Chiropractor, interview 14: 45)
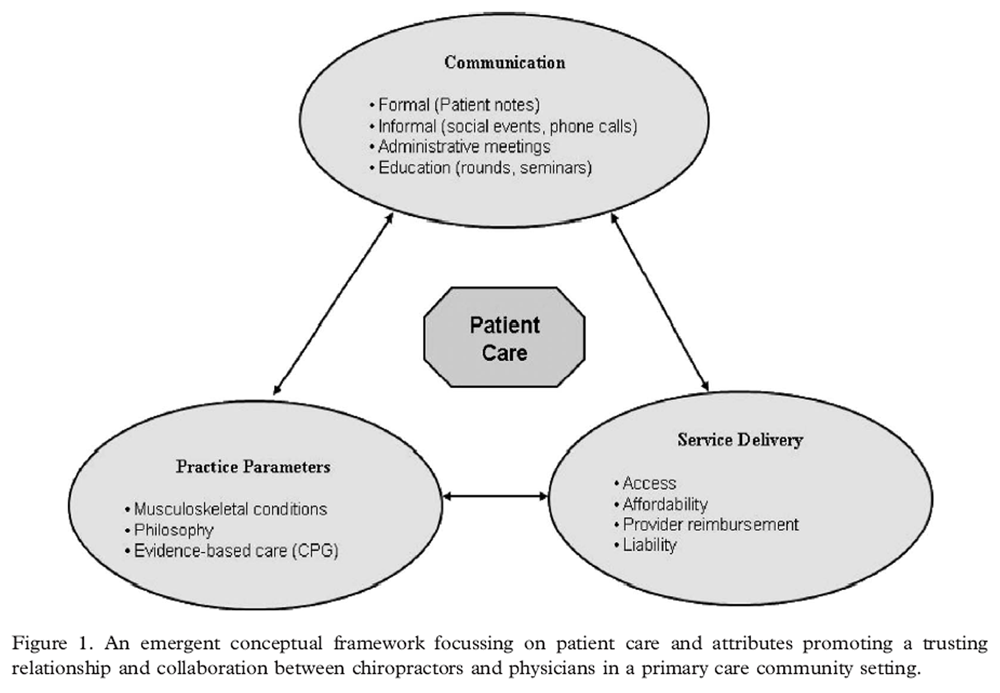
Figure 1 Trust and patient centeredness formed the desired end points of the framework which identified the enabling factors for successful collaboration. These factors clustered under the three categories: communication, practice parameters, and service delivery (See Figure 1). As Figure 1 indicates, within each of these categories, subcategories were identified that defined the activities presumed necessary to optimize successful collaboration. Below is an in-depth description of this framework.
Category 1 – Communication: Communication was identified as critical for the collaborative relationship, as the following data extract illustrates:
I think that communication is really important. Ongoing communication about the situation,
the treatment strategy, and how the patient is responding, is an example of the type
of communication that I think is necessary for true collaboration.
( Midwife, interview 16: 77)The suggested activities to enhance communication included formal and informal meetings. Formal meetings included regular educational workshops or seminars to help inform evidence-based patient care and share knowledge about relevant aspects of medical and chiropractic practices. Because providers' busy schedules could jeopardize communication opportunities, participants suggested meetings be held quarterly at a time convenient for all providers or coincident with hospital or in-service rounds. To promote attendance, these sessions could become a part of a continuing education program that fulfils annual credentialing requirements:
If they did Accredited Group Learning Activities (i.e., continuing education) with us, we would get
to know them pretty well. You create a relationship where you share issues, for example developing
a model of managing acute low back pain.
( Physician, focus group 1: 150)
Education, absolutely, education. Seeing each other's point of view, whereas physicians feel very
strongly about what they have been taught and how they deal with this problem, the chiropractor
feels the same way. So somehow finding some middle ground by spending time together and
understanding what each has to offer the patient is important.
( Patient, focus group 8: 363)Case-based discussions were suggested as a suitable pedagogical format to facilitate the discussion of commonly treated conditions, as well as dealing with controversial issues. Also arranging informal social meetings could help foster personal relationships and contribute to the development of mutual respect and trust. The meetings would be particularly important in the early stages of model implementation to help break down barriers to communication:
So social things, having dinner together, having evening meetings or meetings around an
education event, that will enable you to put a face to a name and chat to them in some
other capacity, allows for a little bit of trust to develop.
( Physician, interview 7: 74)Communicating pertinent patient information was also addressed as a challenge. Ideally such information could be facilitated by access to an electronic medical record (EMR). This would preclude the need to send formal letters, and thus reduce costs and time requirements for practitioners and improve the continuity of care. However, EMRs are not easily available in most primary care settings and patient privacy and security concerns would have to be addressed. Consensus was reached around sharing patient information in a written 1-page form, summarizing pertinent clinical and treatment information. This form could be sent to a secured providers' office facsimile or accompany the patient to their appointment:
It would be helpful to send them (chiropractors) a referral note. We are trying to move ahead
with computerization but we're not quite there but we are also not anxious of increasing
our paperwork . . . Chiropractors don't have compatible computer systems with us,
so we will have to fax them the information.
( Physician, focus group 3: 97)Interprofessional communication could be challenged by "profession-specific language". Participants identified differences in profession-specific terms to describe patient complaints, examination findings, diagnoses, and treatments. A suggestion was made that a glossary of terms be developed as a reference for all interprofessional correspondence:
One of the problems that crop up in communicating with a chiropractor is common language.
Chiropractors speak a different language, use different terminology and I think that is
something that you have to overcome or understand.
( Physician, focus group 8: 53)Participants recommended materials be made available to patients to inform them of the clinical services. These materials, approved by the providers, included in-office posters, pamphlets or brochures, brief announcements in PCN newsletters, and the delivery of patient-directed workshops.
Category 2 – Practice Parameters: This category represented aspects of clinical practice related in general to the scope and delivery of care. All participants recommended that the parameters of practice needed to be clearly defined and based upon best evidence. Concerns were raised by some study participants regarding the controversial areas of chiropractic practice, such as the treatment of infants, on-going treatment plans, the management of systemic conditions (e.g., diabetes and asthma), the reading of x-rays, manipulation of the neck, and perceptions that some chiropractors provided "unscientific treatments":
So if you send someone to a chiropractor for back pain and then the chiropractor
has the whole family going for urinary incontinence and asthma, my patients won't go!
( Physician, interview 1: 51)
Whereas the people in my family, who do go to a chiropractor, go every week
and have for years as far as I know . . . How come there is no end to this?
( Patient, focus group 5: 92)To address these concerns, clinical practice guidelines (CPG) could be introduced to address the variability, quality and costs of care. Furthermore, introducing CPGs dealing primarily with MSC would facilitate collaboration and focus on conditions most commonly managed by chiropractors. Study participants agreed that the benefits of chiropractic care were particularly supported by scientific evidence related to back pain and MSC in general. Most advocated a focus on MSC delivered within specific timelines:
I would start with low back pain. It is the easiest, the safest, the least controversial
and it is actually quite well researched.
( Physician, focus group 1: 221)However, there was also awareness, especially among the chiropractors, that limiting the current scope of chiropractic practice would be inconsistent with current legislation:
We have a scope of practice, so leave it at the scope of practice.
( Chiropractor, focus group 2: 614)Category 3 – Service Delivery: In regard to service delivery (i.e., the process of delivering care), four subcategories emerged: access, affordability, provider reimbursement, and liability. Participants recognized that in Ontario, patients have direct access to chiropractic services and enforcing a different process could create a barrier to collaboration. However, if physicians decided to refer patients, all agreed that the patient's right to choose to attend or see a particular provider should not be violated:
I think that patient choice is so important because if you have a gut feeling
and you don't like it, you need to have that choice to go somewhere else.
( Patient, focus group 8: 433)Some patients who had not previously seen a chiropractor suggested they would prefer to choose from a list or have one recommended by their physician. Similarly some patients with no prior chiropractic experience expressed concern with the image and legitimacy of the chiropractic profession:
I would prefer to have one recommended to me by my doctor. I think that one
of the reasons why people don't go to chiropractors is because they are afraid
and don't know who to go to.
( Patient, focus group 7: 184)Because chiropractors commonly practice independently and are typically not located in the hospital or community clinics, many patients considered chiropractors outside of mainstream health care, further contributing to their uncertainty and concern:
Ultimately we don't associate chiropractors as being a part of the health care system
but that may be my perception. . . . We see chiropractors as stand alone, an alternative
and basically on the other side of the fence, outside of the system, outside of the medical realm.
( Patient, focus group 5: 399)Physicians too suggested that referral for chiropractic care was not always welcomed by some patients; however, they felt that this barrier could be overcome by physician reassurances:
You develop a relationship with your patients and they trust you. If you suggest they see
a chiropractor, even if they have reservations, they will often try it. And once they get better,
they will be fine, and they will come back and tell you that it was good.
( Physician, focus group 8: 389)Cost of chiropractic care was identified by all participants as an important barrier to patient access, and ultimately to collaboration. However, patients had disparate opinions about the ideal payment structure, ranging from coverage of chiropractic care similar to physicians visits to variable out-of-pocket amounts. Most of the chiropractors were open to different reimbursement options providing the patient fee was not significantly different than their office fees and the billing process was simple. Many of the physicians were unfamiliar with how chiropractors were reimbursed. Physicians varied in their recommendation of a patient fee structure, ranging from a sliding fee structure to no fee:
In my opinion there should be equity on both sides. If the patient is not paying out of pocket
to see the MD, then they should not pay to see the chiropractor. If not, then you will be
creating a barrier.
( Chiropractor, focus group 2: 443)Four reimbursement methods were identified: salary, capitation, fee for service, and course of care. Each method had its strengths and weaknesses; for example, in the salary model it was suggested that providers may not be as productive as those working on fee-for-service. However, fee-for-service could promote quantity of care perhaps leading to overuse or inappropriate care. Regardless of the method used, participants emphasized that it must be seen equitable for all parties if the collaboration is to be successful:
I think the lack of equity leads to bad attitudes and bad attitudes lead to lack of wanting
to work together collaboratively.
( Physician, interview 1: 25)Physicians raised concerns about liability when referring patients for chiropractic care. In part, this concern was based upon lack of knowledge regarding chiropractors' liability insurance, as well as the physicians' experiences with other health care givers, in particular nurse practitioners and midwives. However, non-physician participants had the opposite view, suggesting that it was nothing more than a "red herring" as all regulated health professions in Ontario have liability coverage:
The concern that working with (other professionals) will increase physician liability is nothing
but a red herring. . . (They) are accountable to (their Colleges); they are registered, have a
legislatively defined scope of practice and carry their own insurance.
So physicians don't carry increased liability.
( Nurse, interview 3: 127)
Discussion
Despite the increasing integration of complementary and alternative therapies into the mainstream health care system (Coulter et al., 2005; Mizrachi et al., 2005), there is still confusion surrounding the terms and extent of such acceptance (Boon & Kachan, 2008). Our study suggests that health care providers are able to conceptually differentiate between integration and collaboration based upon the structure and process of the relationship. Unlike integration, collaboration was perceived as working together, but maintaining autonomy in the absence of a formal structure (Boon et al., 2009; Oandasan et al., 2006). Participants preferred the term collaboration. This preference may symbolically demarcate professional boundaries and define the limits of the relationship in an effort to avoid potential confrontations (Mizrachi et al., 2005), while simultaneously protecting their interests (Kelner et al., 2004).
The study identified previously described attributes of a successful collaborative practice (Nolte, 2005; Orchard et al., 2005; San Martin-Rodriguez et al., 2005; Way et al., 2000) and barriers to the integration of chiropractic services into physician-based environments (Astin et al., 1998; Coulter et al., 2005; Greene et al., 2006). Acknowledging the unique site-specific barriers and enablers is the first step in implementing a collaborative practice (Kailin, 2001). A fundamental enabler to successful collaboration is developing and maintaining a trusting relationship (Boon & Kachan, 2008; D'Amour et al., 2005; Orchard et al., 2005). This was identified by the majority of the participants who emphasized the importance of a harmonious relationship between providers and patients if the collaboration is to survive. Trust is built upon understanding, communication, and delivering care based upon best practice (Boon & Kachan, 2008; Frenkel & Borkan, 2003). Despite growing interest among physicians for CAM therapies, they lack understanding of CAM and have little awareness that their patients seek CAM providers (Kaczorowski et al., 2002). We incorporated strategies into our framework that would promote social and professional communication between providers, understanding of professions and their roles, and focus on best practice care of MSC.
The centrality of the patient in our model is consistent with overarching focus of interprofessional collaborative practice (D'Amour & Oandasan, 2005; Frenkel & Borkan, 2003; Nolte, 2005; Oandasan et al., 2006). The resulting framework is centered on meeting the needs of the patient, promoting choice and their participation in clinical decisionmaking, and providing a common ground among the providers and patients that transcends the potential tensions from philosophical differences. It also highlights the importance of patient access, including affordability.
A number of frameworks have been proposed to address the structure, composition, settings, and barriers to collaborative practice, but few relate to matters of process, or involve CAM providers who are not organizationally situated (Coulter et al., 2005; D'Amour et al., 2005; Institute of Medicine, 2005). We present a framework whose characteristics are similar to the structuration model presented by D'Amour and colleagues (D'Amour et al., 2005; San Martin-Rodriguez et al., 2005); in both frameworks the patient is the focus and both include influential processes broadly related to organizational and relational enablers of collaboration. While in D'Amour's framework the processes to improve relationships are conceptualized, in ours they are operationalized. Although we acknowledge the importance of champions and leaders in supporting collaboration (two dominant organizational enablers of collaboration, governance and formalization in D'Amour's framework); we did not include them in our framework. We mostly focused on practice and care delivery processes that may be considered to fall within "formalization", and more relevant within primary care.
The differences between the two frameworks may be a product of the setting wherein they were derived, one in structured organizational team-based settings (D'Amour et al., 2005) and ours in loosely structured community-based settings. We wanted to create a practical framework appropriate for the planning and implementation of interprofessional collaborative practice. While some may view this as an opportunity to enhance chiropractic's legitimacy (Myburgh et al., 2008), we see it as a way of supporting greater communication between chiropractors, patients, and physicians; decreasing the fragmentation of patient care; and improving the continuity and quality of care (Greene et al., 2006; Mainous et al., 2000).
The limitations of this study were that it involved key informants from a few sites from across North America and the focus groups were comprised of participants in only two preselected PCN pilot sites in rural Ontario, Canada. Although the results from the focus groups at both sites were similar, it is possible that additional groups in different locations may have yielded different or additional information. Also the nature of the data interpretation may have yielded different conclusions if analyzed from a particular perspective of one of the participant groups. However, the diversity of backgrounds and the experience of the study team limited a biased interpretation of results.
Conclusion
Physicians, chiropractors, and patients participating in focus groups generally supported a framework of collaboration to optimize the efficient and effective use of limited resources. The framework developed in this study may help to understand and promote interprofessional collaborative practice not only between physicians and chiropractors, but other health care providers in primary care. The implementation and subsequent evaluation of this proposed model should determine if it enhances interprofessional collaborative practice.
Acknowledgement
Funding was provided from a grant from the Ontario Ministry of Health and Long TermCare, Canada.
Declaration of interest:
The authors report no conflict of interest. The authors alone are responsible for the content and writing of the paper.
References:
Astin, J. A., Marie, A., Pelletier, K. R., Hansen, E., & Haskell, W. L. (1998).
A review of the incorporation of complementary and alternative medicine by mainstream physicians.
The Archives of Internal Medicine, 158, 2303–2310.Balon, J. W., & Mior, S. A. (2004).
Chiropractic care in asthma and allergy.
Annals of Allergy Asthma and Immunology, 93, S55–S60.Barrett, J., Curran, V., Glynn, L., & Godwin, M. (2007).
CHSRF Synthesis: Interprofessional Collaboration and Quality Primary Healthcare.
Ottawa: Canadian Health Services Research Foundation.Boon, H., & Kachan, N. (2008).
Integrative medicine: A tale of two clinics.
BMC Complementary and Alternative Medicine, 8, 1–8.Boon, H.S., Mior, S.A., Barnsley, J., Ashbury, F.D., and Haig, R.
The Difference Between Integration and Collaboration in Patient Care:
Results From Key Informant Interviews Working in
Multiprofessional Health Care Teams
J Manipulative Physiol Ther. 2009 (Nov); 32 (9): 715–722Cameron, C., Ashbury, F. D., & Iverson, D. C. (1997).
Perspectives on Reach to Recover and Can Surmount: Informing the evaluation model.
Cancer Prevention & Control, 1, 102–107.Charmaz, K. (2000).
Grounded theory: Objectivist and constructivist methods.
In N. K.Denzin & Y. S. Lincoln (Eds.),
Handbook of qualitative research (pp. 509–535).
Thousand Oaks, CA: SAGE Publications.Coulter, I., Singh, B. B., Riley, D., & Der-Martirosian, C. (2005).
Interprofessional referral patterns in an integrated medical system.
Journal of Manipulative and Physiological Therapeutics, 28, 170–174.Creswell, J. W. (1998).
Qualitative inquiry and research design: Choosing among five traditions.
Thousand Oaks, CA: Sage Publications.D'Amour, D., Ferrada-Videla, M., Rodrigues, L., & Beaulieu, M. (2005).
The conceptual basis for interprofessional collaboration: Core concepts and theoretical frameworks.
Journal of Interprofessional Care, 19, 116–131.D'Amour, D., & Oandasan, I. (2005).
Interprofessionality as the field of interprofessional practice and interprofessional education: An emerging concept.
Journal of Interprofessional Care, 19, 8–20.Frenkel, M. A., & Borkan, J. M. (2003).
An approach for integrating complementary-alternative medicine into primary care.
Family Practice, 20, 324–332.Glaser, B., & Strauss, A. (1967).
The discovery of Grounded Theory: Strategies for qualitative research.
Chicago: Aldine.Greene, B. R., Smith, M., Allareddy, V., & Haas, M. (2006).
Referral patterns and attitudes of primary care physicians towards chiropractors.
BMC Complementary and Alternative Medicine [On-line]. Available from:
http://www.biomedcentral.com/1472-6882/6/5Institute of Medicine (2005).
Integration of CAM and Conventional Medicine (Chapter 7)
In I.o.M.Committee on the Use of Complementary and Alternative Medicine (Ed.),
Complementary and Alternative Medicine in the United States (pp.196–225).
Washington, DC: The National Academies Press.Kaczorowski, J., Patterson, C., Arthur, H., Smith, K., & Mills, D. A. (2002).
Complementary therapy involvement of physicians: Implications for practice and learning.
Complementary Therapies in Medicine, 10, 134–140.Kailin, D. C. (2001). Initial strategies.
In N.Fass (Ed.), Integrating complementary medicine into health systems (pp. 44–48).
Gaithersberg: Aspen Publication.Kelner, M., Wellman, B., Boon, H., & Welsh, S. (2004).
Responses of established healthcare to the professionalization of complementary and alternative medicine in Ontario.
Social Science and Medicine, 59, 915–930.Krueger, R. A. (1998).
Moderating focus groups (vol. 4).
Thousand Oaks, CA: Sage Publications.Mainous, A. G., Gill, J. M., Zoller, J. S., & Wolman, M. G. (2000).
Fragmentation of patient care between chirpractors and family physicians.
Archives of Family Medicine, 9, 446–450.Mizrachi, N., Shuval, J. T., & Gross, S. (2005).
Boundary at work: Alternative medicine in biomedical settings.
Sociology of Health & Illness, 27, 20–43.Myburgh, C., Hartvigsen, J., & Grunnet-Nilsson, N. (2008).
Secondary legitimacy: A key mainstream health care inclusion strategy for the Danish chiropractic profession?
Journal of Manipulative and Physiological Therapeutics, 31, 392–395.Nolte, J. (2005).
Enhancing interdisciplinary collaboration in primary health care in Canada.
Ottawa: Conference Board of Canada.Oandasan, I., Baker, R., Barker, K., Bosco, C., D'Amour, D., Jones, L. et al. (2006).
Teamwork in health care: Promoting effective teamwork in health care in Canada –
policy synthesis and recommendations.
Ottawa: Canadian Health Services Research Foundation.Orchard, C. A., Curran, V., & Kabene, S. (2005).
Creating a culture for interdisciplinary collaborative professional practice.
Medical Education [On-line]. Available from:
www.med-ed-online.orgSan Martin-Rodriguez, L., Beaulieu, M., D'Amour, D., & Ferrada-Videla, M. (2005).
The determinants of successful collaboration: A review of theoretical and empirical studies.
Journal of Interprofessional Care, 19, 132–147.Strauss, A., & Corbin, J. (1998).
Basics of qualitative research: Techniques and procedures for developing grounded theory, 2nd edn.
Thousand Oaks, CA: Sage Publications.Theberge, N. (2007).
The integration of chiropractors into healthcare teams: A case study from sport medicine.
Sociology of Health and Illness, 30, 19–34.Way, D., Jones, L., & Busing, N. (2000).
Implementation strategies: Collaboration in primary care – family doctors & nurse practitioners delivering shared care.
Toronto: The Ontario College of Family Physicians.Weeks, J. (1997).
The emerging role of alternative medicine in managed care.
Drug Benefit Trends, 9, 14–16, 25–28.
Return to INTEGRATED HEALTH CARE
Since 8-15-2018


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |