

Positive Patient Outcome After Spinal Manipulation
in a Case of Cervical AnginaThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: Man Ther. 2009 (Dec); 14 (6): 702–705 ~ FULL TEXT
Steven R. Passmore, Andrew S. Dunn
Veterans Affairs of Western New York Health Care System,
Buffalo, New York, USA.
passmosr@mcmaster.ca
Introduction
When angina pectoris is suspected but adequately ruled out, upper anterior chest pain and related symptoms may be attributed to cervical angina, particularly in the presence of radiculopathy and myelopathy (Nakajima et al., 2006). Cervical angina is theorized to involve the C6, C7, or T1 nerve roots, and possibly the medial and lateral pectoral nerves (Jacobs, 1990; Freccero and Donovan, 2005). While the prevalence of cervical angina is not completely clear, it is described as a virtually unknown and neglected clinical syndrome that may not be uncommon but is under diagnosed (Nakajima et al., 2006; Christensen et al., 2005). Aside from cardiac enzyme and exercise tolerance testing, Christensen et al. (2005) suggest cervical angina is potentially recognized from true angina through manual palpation of the spine and thorax.
There are more articles like this @ our:
What is the Chiropractic Subluxation PageManual palpation for locating vertebral joint dysfunction is most reliably indicated through eliciting tenderness (Jull et al., 1988; Hubka and Phelan, 1994; Haavik- Taylor and Murphy, 2007). Further diagnostic tactics that may discern cervical from true angina may include improvement after corticotrophin therapy but not glyceryl trinitrate, normal temperature, and lack of vasomotor changes (Grieve,1988). However, upon recognition of the presentation, what is an appropriate course of care for cervical angina? Nakajima et al. (2006) suggest that anterior cervical surgical procedures that alleviate compression on nerve roots or the spinal cord and may be palliative. The same authors also mention surgery should be avoided until conservative measures have been exhausted, but caution the use of ææaimless conservative therapyÆÆ (Nakajima et al., 2006). So the question remains what is an appropriate, focused approach to the conservative treatment of cervical angina? Furthermore, what type of intervention and treatment frequency should be recommended and what is the sustainability of such an intervention?
This paper follows the case of a patient with cervical angina in whom radiographic findings can be correlated to patient presentation. The symptoms of cervical angina responded to a brief course of spinal manipulative therapy (SMT) targeted at the cervicothoracic junction, a novel finding previously absent in the literature.
Case description
History
A 42–year-old woman was referred for evaluation and management of neck pain with cervical radiculopathy and comorbid cervical spondylosis. Upon subjective evaluation, symptoms reportedly developed over the previous five years, for which the patient had not actively pursued management options. During her history, the patient described her neck pain as æænumb, dull, and sometimes accompanied by sharpness across the chestÆÆ. The patient was naive to SMT, and was referred to the clinic by her primary care physician.
Examination
A cervical spine radiographic study performed the week prior to consultation was compared to a study performed 3 years earlier that revealed minor anterior wedging of the C3 vertebral body without instability. The remaining cervical vertebral heights and alignment were otherwise maintained. The prevertebral soft tissues were intact. Subtle narrowing of the C4–5 disc space was observed and minimal uncovertebral spurringwas noted on the left at the C3–4 and C5–6 levels (Fig. 1). The right intervertebral foramina were patent.
During the objective examination a Neck Disability Index (Cleland et al., 2006) (NDI) score of 58 was recorded as a baseline outcome measure. ValsalvaÆs manoeuvre/test (Rubinstein et al., 2007), the Cervical compression test (Rubinstein et al., 2007), and Cervical traction/neck distraction test (Rubinstein et al., 2007) were positive. Muscular reflexes were 1–2+ and bilaterally symmetric at levels C5–7. Upper extremity clonus was absent. Motor strength was 4–5+ throughout. Sensory examination was hypoesthetic over the C7 dermatome. Passive cervical range of motion as observed was pain producing into extension, lateral flexion and rotation toward end range. Hypokyphosis was noted in the thoracic spine. Segmental palpation (Jull et al., 1988) was painful at C3–4 bilaterally, and T4–5 on the left. Manual palpation revealed hypertonicity with tenderness in the suboccipital and levator scapulae musculature bilaterally. Due to the pre-existing diagnoses of cervical radiculopathy and spondylosis, with no additional upper extremity complaint peripheral joint examination was deferred at this time.
Interventions and outcomes
Treatment was initiated and the patient received high-velocity, low-amplitude (HVLA) SMT to the regions indicated by segmental palpation (C3–4 bilaterally, and T4–5 on the left) in conjunction with passive stretches for the suboccipital and levator scapulae bilaterally. Stretches were held once muscle tension was attained for 10 s. In the cervical spine a supine digit pillar pull (Peterson and Bergmann, 2002)was employed for SMT while in the thoracic spine a bilateral hypothenar transverse push (Peterson and Bergmann, 2002) was utilized. Immediately following treatment the patient verbally self-reported localized æædecreased stiffness and painÆÆ in the cervical region. These procedures and outcome occurred on two instances (treatment visits 1 and 2).
The present body of literature on spinal manipulation has not specifically identified an optimal dosage of care in regard to the number and frequency of visits (Jull and Moore, 2002; Haas et al., 2004). While laboratory studies have examined changes immediately following a single instance of spinal manipulation (Martinez- Segure et al., 2006; Tseng et al., 2006; Haavik-Taylor and Murphy, 2007), this immediate re-evaluation with completed outcome measures and full physical assessment has not yet translated into standard clinical practice. Clinical papers cite delay of thorough reevaluation for periods up to 9 or 12 visits, to follow a course of care as opposed to a single instance of intervention (Haas et al., 2004). In the present case the plan included a treatment frequency of two visits per week with re-evaluation after the forth visit in an attempt to minimize the number of patient visits needed to bring about clinical change or lack thereof, and indentify an appropriate end point early on in care to minimize potential over treatment (Dunn and Passmore, 2008).
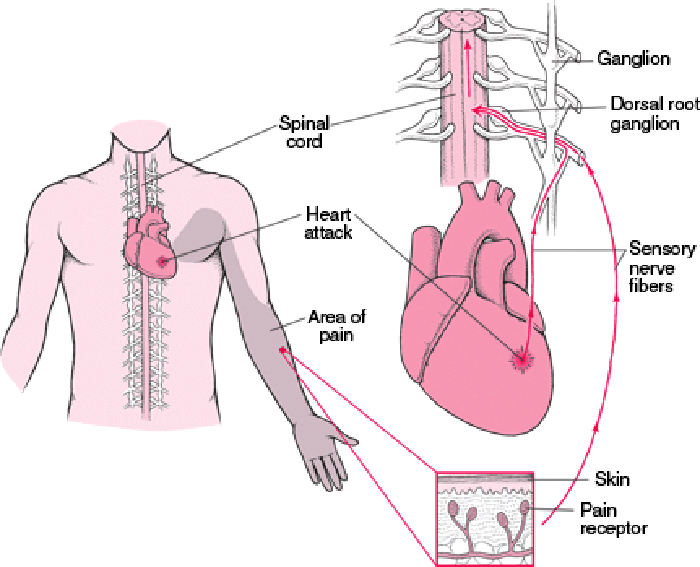
Upon presentation for her third scheduled appointment, she reported that the prior treatment had minimally sustained palliative effects, and that sleep the night before was interrupted by sensations of a self perceivedmyocardial infarction, including chest pain with dizziness, and pain in the lateral aspect of the left upper extremity with paresthesia distribution into the first through third digits (Fig. 2), in addition to her previous neck pain. Manual therapy was deferred and the patient, who had a previous borderline exercise tolerance test (ETT) to investigate a prior apparent cardiac episode, was sent to the emergency department (ED) for evaluation. Immediately prior to referral for manual therapy the referring physician performed cardiac auscultation and described the presence of regular rate and rhythm of all heart sounds with the absence of murmur.
The attending ED physician requested an electrocardiogram, and chest radiographs, but found no significant findings. Serial cardiac enzyme laboratory analysis was also negative. Upper extremity pain radiation was provoked positionally by cervical spine left lateral flexion (Lindgren et al., 1992) and the diagnosis of cervical angina was communicated. Having ruled out cardiac etiology, a return to manual therapy was determined. The patientÆs course of care for neck pain with cervical spine radiculopathy was resumed at levels indicated by palpation in the cervical and thoracic spine (C3–4 bilaterally, and T4–5 on the left) with the addition of HVLA techniques directed specifically to hypomobile and tender segments (C5–6 on the left, C6–7 on the right and the T2 costotransverse joint on the left) at the cervicothoracic junction as cervical angina is theorized to involve the C6, C7, or T1 nerve roots (Jacobs, 1990; Freccero and Donovan, 2005).
Manipulation directed at the cervicothoracic junction was delivered utilizing the thumb spinous push technique (Peterson and Bergmann, 2002). The patient lay prone and the clinician made a first distal phalange to spinous process contact while inducing lateral flexion targeted at facet joint manipulation. Also, the prone hypothenar costal push, (Peterson and Bergmann, 2002) was utilized in which the clinicianÆs hypothenar region contacted the patientÆs upper costal angles, and HVLA SMT was delivered to manipulate the costovertebral articulations. These techniques were integrated into the existing treatment plan with delivery at an intended frequency of twice per week at dysfunctional motion segments (Dunn and Passmore, 2008). This was performed on two occasions before re-evaluation (treatment visits 3 and 4).
After her fifth scheduled appointment (treatment visit 4), a reevaluation was performed. Segmental palpation was no longer painful in the cervical or thoracic spine regions. ValsalvaÆs manoeuvre/test, Cervical Compression Test, and Cervical traction/neck distraction test were painless and a re-evaluation NDI score of 48 was recorded. Immediately following treatment she noted a sustained decrease in cervical spine pain and chest pain, and following the second treatment directed to the cervicothoracic region her pain had resolved. While spontaneous recovery can never be completely dismissed, based on the temporal correlation of the decrease in symptom presentation, clinical findings, and outcome measure scores while undergoing a course of SMT it is theoretically feasible to attribute this patientÆs improvement to the intervention. She followed up with her primary care physician for her biannual physical examination 11 weeks later without report of chest pain at that time.
Discussion
Atypical chest pain presentations related to cervical radiculopathy entered the literature over 70 years ago when Nachlas (1934) identified what he described as ææpseudo angina pectorisÆÆ. Later, Hanflig (1936) suggested pain in the shoulder girdle, arm and precordium can be attributed to cervical arthritis. The term ææcervical anginaÆÆ came into favour following a publication by Jacobs (1990).
Recent cases in the literature reported chest pain with associated nerve root impingement ranging from C6–T2 (Freccero and Donovan, 2005; Ozgur and Marshall, 2003; Yeung and Hagen,1993). A retrospective chart review of 241 cases of C6–7 anterior cervical discectomy with unilateral nerve root impingement revealed that 15% presented with breast/chest pain (Ozgur and Marshall, 2003). Ozgur and Marshall (2003) proceed to state that of those 15% of individuals, 90% experienced long-term relief following anterior cervical discectomy and fusion, which they feel, is a clear indication of nerve root involvement.
However, Grant and Keegan (1968) and more recently Erwin et al. (2000) suggest that costovertebral joints might be an under recognized site of pain generation in atypical chest, upper back and arm pain. Grant and Keegan (1968) found that pressure applied over the ribs that reproduced chest pain could be used to identify ææcostal syndromeÆÆ, and additional pressure over the dorsal spine could identify æævertebro-costal syndromeÆÆ which occurred most often at a single vertebral level. Although no treatment options, descriptions, or protocol were detailed in the primarily diagnostic clinical paper the authors mentioned pain was often relieved by spinal traction. They also state that in their 41 clinical patients there were five consistent symptoms reported that were congruent with presentation which included accurate localization, accentuation by thoracic spine movement, exacerbation by breathing/coughing/ straining, association with posture/position, and a history of mechanical stress (Grant and Keegan, 1968). Erwin et al. (2000) demonstrate the anatomic possibility of pain production via evidence for the existence of enervated synovial folds in the costovertebral joints. It remains unclear if chest pain generation is occurring at the site of the nerve root, the costotransverse joints, or potentially the zygapophyseal joints (Erwin et al., 2000).
In this patient when cervicothoracic SMT was delivered, it was directed at both the upper thoracic costotransverse joints, and lower cervical zygapophyseal joints. With a theoretical etiology of cervical radiculopathy, a positive response to manual therapy in this case of cervical angina was congruent with predictions theorized in a recent radiculopathy study (Cleland et al., 2007). In agreement with a cervical radiculopathy and manual therapy outcome prediction paper this patientÆs anticipated response was favourable as her age is less than 54 years, and radicular symptoms were in her non-dominant arm (Cleland et al., 2007). Supporting a recent cervical radiculopathy outcome measure study, this patient demonstrated an NDI improvement that exceeds a minimally detected change of 7, and meets a minimally clinically important difference of 10 points improvement (Cleland et al., 2006).
In a study on the diagnostic accuracy of cervical spine palpation, while there were no false-positives (medically asymptomatic zygapophysial joints diagnosed as symptomaticmanually), therewas an instance of a false-negative (medically symptomatic zygapophysial joints diagnosed as asymptomatic manually) (Jull et al., 1988). This false-negative occurred at the level of the C6–7 zygapophysial joint. It was also the only instance inwhich a joint belowC5–6was indicated by either medical or manual diagnosis. This finding could be interpreted as indicative that manual diagnoses of symptomatic lower cervical, or cervicothoracic joints may be more difficult to discern. Symptomatic joints in the cervicothoracic region could have falsely been declared clear until patient symptomatic presentation clearly warrantedmore thorough assessment of the joints in this region. This was the case in the present course of management.
This patient presented with unilateral osteophytes of the uncovertebral joints projecting into the intervertebral foramen potentially serving as the etiology of her cervical radiculopathy and cervical angina, but they may also be a benign comorbid condition. Had she not experienceda sustainedresponse toSMT,other treatmentoptions include but are not limited to active exercise, cervical spine traction, grade I–IV mobilisation, pharmacological intervention, or surgery. Authors of a recent study suggest that there is controversy over the possibility of relieving radicular symptoms without removal of offending osteophytes via direct surgical decompression of the uncovertebral joints.Shenet al. (2004)postulate thatanterior cervical discectomy and fusion (ACDF) can add the 2–3mm of distraction prerequisite for a favourable clinical outcome without osteophyte removal. Finding that it is unnecessary to remove potentially offending osteophytes to see clinical improvement supports why radicular symptoms could be alleviated by SMT, which has been demonstrated to increase zygapophysial joint space on MRI post manipulation (Cramer et al., 2002). However, should future patients fail to respondto cervicothoracicSMTorotherconservativemeasures, and where patients fail to respond to ACDF, uncoforaminotomy to remove osteophytes is the suggested approach to care (Pechlivanis et al., 2006).
When assessing a patient presenting with chest pain, a distinction between cervical angina, and true angina must be made to diagnose and manage cardiac issues distinct from mechanical neck, costovertebral and shoulder pain. Patients should be screened to rule out cardiac etiology first. A study examining co-morbidity for people in their seventies with mild, moderate and severe neck and shoulder pain revealed a significant percentage of individuals reported a history of angina (Vogt et al., 2003). With regard to neck pain rated mild, moderate, or severe, the associated percentages of people who reported angina were, respectively, 13.1%, 19.1%, and 16.4%. With regard to shoulder pain rated mild, moderate, or severe, the associated percentages of people who reported angina were, respectively 13.3%, 14.5%, and 18.6%.
Conclusion
This case identified an individual with the under diagnosed phenomena of cervical angina. This patient demonstrated a sustained improvement up to 11 weeks following a brief trial of SMT directed to the cervicothoracic region, suggesting a mechanically based, musculoskeletal etiology to her presentation. Future prospective studies are needed to assess the viability of a course of SMT management, and the consideration of related treatments such as grade I–IV joint mobilisation for patients who have tested negative for true angina, but continue to present with unrelenting atypical chest and upper extremity pain prior to directing them for surgical management. These additional studies also need to confirm the appropriate dosage of SMT for these patients following clearance and referral from cardiology through carefully controlled clinical studies with re-evaluation following each intervention. This case also raises the issue of the need for careful palpation to ascertain dysfunction in tissues, and the possibility that such dysfunction in the cervicothoracic junction may be more difficult to identify through manual palpation then other regions. Future work is needed to determine whether it is HVLA manipulation of the costotransverse, zygapophyseal or the combination of these joints in conjunction with passive stretches that may have contributed to the therapeutic benefit of this course of management.
Acknowledgments
The research endeavours of Steven Passmore are funded in part by Fellowships from the Foundation for Chiroparactic Education and Research, New York Chiropratic College and an Ontario Graduate Scholarship.
References:
Christensen HW, Vach W, Gichangi A, Manniche C, Haghfelt T, Hoilund-Carlsen PF.
Cervicothoracic angina indentified by case history and palpation findings in patients
with stable angina pectoris.
J Manipulative Physiol Ther 2005;28: 303–11.Cleland J, Fritz J, Whitman J, Heath R.
Predictors of short-term outcome in people with a clinical diagnosis of cervical radiculopathy.
Phys Ther 2007;87:1619–32.Cleland J, Fritz J, Whitman J, Palmer J.
The reliability and construct validity of the Neck Disability Index and patient specific
functional scale in patients with cervical radiculopathy.
Spine 2006;31:598–602.Cramer GD, Gregerson DM, Knudsen JT, Hubbard BB, Ustas LM, Cantu JA.
The effects of side-posture positioning and spinal adjusting on the lumbar Z joints:
a randomized controlled trial with sixty-four subjects.
Spine 2002;27:2459–66.Dunn, AS and Passmore, SR.
Consultation Request Patterns, Patient Characteristics, and Utilization of Services
within a Veterans Affairs Medical Center Chiropractic Clinic
Mil Med. 2008 (Jun); 173 (6): 599–603Erwin WM, Jackson P, Homonko D.
Innervation of the human costovertebral joint: implications for clinical back pain syndromes.
J Manipulative Physiol Ther 2000;23:395–403.Freccero D, Donovan D.
Adjacent segment degeneration at T1–T2 presenting as chest pain.
Spine 2005;30:E655–7.Grant AP, Keegan DA.
Rib pain – a neglected diagnosis.
Ulster Med J 1968;37:162–9.Grieve GP.
In: Common vertebral joint problems. 2nd ed.
Edinburgh: Churchill Livingstone; 1988. p. 393–4.Haas M, Groupp E, Aickin M, Fairweather A, Ganger B, Attwood M, et al.
Dose Response for Chiropractic Care of Chronic Cervicogenic Headache
and Associated Neck Pain: A Randomized Pilot Study
J Manipulative Physiol Ther 2004 (Nov); 27 (9): 547ù553Haavik-Taylor H, Murphy B.
Cervical Spine Manipulation Alters Sensorimotor Integration:
A Somatosensory Evoked Potential Study
Clin Neurophysiol. 2007 (Feb); 118 (2): 391û402Hanflig S.
Pain in the shoulder girdle, arm, and precordium due to cervical arthritis.
JAMA 1936;106:523–6.Hubka M, Phelan S.
Interexaminer reliability of palpation for cervical spine tenderness.
J Manipulative Physiol Ther 1994;17:591–5.Jacobs B.
Cervical angina.
NY State J Med 1990;90:8–11.Jull, G, Bogduk, N, and Marsland, A.
The Accuracy of Manual Diagnosis for Cervical
Zygapophysial Joint Pain Syndromes
Med J Aust 1988 (Mar 7); 148 (5): 233û236Jull G, Moore A.
What is a suitable dosage of physical therapy treatment?
Man Ther 2002;7:181–2.Lindgren KA, Leino E, Manninen H.
Cervical rotation lateral flexion test in brachialgia.
Arch Phys Med Rehabil 1992;73:735–7.Martinez-Segura R, Fernandez-de-las-Penas C, Ruiz-Saez M.
Immediate Effects on Neck Pain and Active Range of Motion After a Single
Cervical High-velocity Low-amplitude Manipulation in Subjects Presenting
with Mechanical Neck Pain: A Randomized Controlled Trial
J Manipulative Physiol Ther 2006 (Sep); 29 (7): 511û517Nachlas I.
Pseudo-angina pectoris originating in the cervical spine.
JAMA 1934;103:323–5.Nakajima H, Uchida K, Kobayashi S, Kokubo Y, Yayama T, Sato R, et al.
Cervical angina: a seemingly still neglected symptom of cervical spine disorder?
Spinal Cord 2006;44:509–13.Ozgur B, Marshall L.
Atypical presentation of C-7 radiculopathy.
J Neurosurg Spine 2003;99:169–71.Pechlivanis I, Brenke C, Scholz M, Engelhardt M, Harders A, Schmieder K.
Anterior uncoforaminotomy in the treatment of recurrent radiculopathy after anterior
cervical diskectomy with fusion.
Minim Invasive Neuorsurg 2006;49:323–7.Peterson DH, Bergmann TF, editors.
Chiropractic technique. 2nd ed.
St. Louis: Mosby; 2002. p. 222–76.Rubinstein SM, Pool JJ, van Tulder MW, Riphagen H, de Vet HC.
A systematic review of the diagnostic accuracy of provocative tests of the neck
for diagnosing cervical radiculopathy.
Eur Spine J 2007;16:307–19.Shen F, Samartzis D, Khanna N, Goldberg E, An H.
Comparisson of clinical and radiographic outcome in instrumented anterior cervical
diskectomy and fusion with or without direct uncovertebral joint decompression.
Spine J 2004;4: 629–35.Tseng Y, Wang W, Chen W, Hou T, Chen T, Lieu F.
Predictors for the immediate responders to cervical manipulation in patients with neck pain.
Man Ther 2006;11:306–15.Vogt M, Simonsick E, Harris T, Nevitt M, Kang J, Rubin S, et al.
Neck and shoulder pain in 70- to 79-year-old men and women: findings from the
health, aging and body composition study.
Spine J 2003;3:435–41.Yeung M, Hagen N.
Cervical disk herniation presenting with chest wall pain.
Can J Neurol Sci 1993;20:59–61.
Return to SUBLUXATION
Since 1-11-2018


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |