CHAPTER 9: DELIVERY
Primary Care Groups
9.21 Prior to the introduction of PCGs in April 1999,
GP fund-holding practices could support the provision of CAM services
through savings they had achieved on their budgets, and an estimated
12% of fund-holding practices were choosing to do this in 1995[55].
Once PCGs were introduced, all practice-based services, including
CAM services, came under review. Many of our witnesses expressed
concern that fund-holding practices which had decided to 'go it
alone' in providing CAM services would not be able to convince
their new partners in a PCG that CAM provision should continue.
9.22 The Department of Health commissioned a study
in April 2000 on the way CAM services are "reconfigured in
the NHS under PCGs"[56].
This study identified the need for a consensus across the PCG
as one important factor likely to determine CAM provision (previous
evidence shows that consensus on CAM was hard to reach even when
it was only sought within the individual practices). The study
also explained that any decision about CAM will have to take into
account the two guiding principles for PCGs: these are the need
to take into account the issue of adequate clinical governance,
and to concentrate on the local population's primary care needs.
9.23 There does seem to be some justification for
CAM practitioners' concern that the organisation of PCGs will
impair the prospects of CAM services being commissioned within
the NHS. We took evidence from the NHS Alliance, which was formed
as a result of the introduction of PCGs in order to represent
them and help them to become established (Q 1459). They told us
that the extent of commissioning of CAM did seem to be falling,
and with particular reference to osteopathy (one of the CAM services
most commonly commissioned under fund-holding) they told us that
"…surveys suggest that PCGs are not renewing the existing
contracts held over from former fundholding arrangements. Our
own research indicates that over 32.8 per cent have been discontinued.
We believe this is due to the fact that PCGs have been given the
role of balancing inequality of access from the old fund-holding
system. This means they have to make a decision as to whether
to extend a minority service or discontinue it completely. The
problem we face, and it is a very important one, is that by discontinuing
osteopathy PCGs are reversing the trend for innovation within
primary care" (Q 427).
9.24 The NHS Alliance went on to elaborate on the
problems CAM will face if PCGs continue with this trend: "If
new approaches to treatment cannot be piloted in one or two GP
practices before they are extended to all in a PCG then important
opportunities for research in evidence-based practice will be
lost. This reversal of the trend to using osteopathy in primary
care will continue unless there is some incentive against it.
Once this relationship is lost it is difficult to see how comparative
studies will ever occur" (Q 427). They also suggested that
one way of attempting to encourage PCGs to reverse this trend
would be "…some exemption given to PCGs to allow the
piloting of CAM projects within a single or a couple of GP units
within each PCG. This would enable the evidence to be built up
as to whether or not it is applicable to extend that service over
the rest of the PCG. What we fear is that if that flexibility
is not built into the system then complementary medicine will
suffer" (Q 429).
9.25 The NHS Alliance did indicate that some of the
problems discussed above may not be permanent: "… primary
care groups and trusts are getting on to their feet. The primary
care group is meant to be instilling new ideas, it is meant to
be thinking the unthinkable, it is meant to be taking risks in
many ways. There have not been great risks taken in that first
year, largely, as I say, because of lack of funds. They will start,
I think, taking greater risks in the conventional sense, I do
not mean real risks of course. They will start doing that as they
gain their confidence and their feet…as the public become
more involved in what they are doing…It will take time for
the professionals to become involved, it is going to take time
for the patients to become involved, even more time for them to
get properly briefed and be able to arm themselves with the same
sorts of arguments and evidence that the professionals may be
using against them. It is very doctor dominated at the moment,
the scene, but I think that will change" (Q 1468).
9.26 However, some of the GPs interviewed in the
Department of Health's commissioned report on the provision of
complementary medicine under PCGs, referred to in paragraph 9.21,
were less sure that the situation would change in the near future.
That survey found that "most of the service providers who
rated complementary medicine as a low priority within their PCG
at the moment, felt that this situation was likely to continue
in the medium to long term"[57].
9.27 The NHS Alliance told us that they did have
a positive vision of how CAM may be provided by PCGs and PCTs
in the future. Dr Michael Dixon told us: "I would see the
future provision of complementary care being something that is
decided at PCT level so that there is some standardisation and
equity and that the actual service could be provided either from
one of these centres or, where you have got large practices, there
is no reason why the individual therapist should not be working
in those practices. I think what that would offer would be a co-ordinated
programme of complementary care within the Primary Care Trust
and one which was flexible as to where the care was going to be
provided…The new Primary Care Groups and Trusts are going
to have to commission care, the long pathways of care, using these
long-term service agreements. What I foresee is that the pathways
of care, the long-term service agreements, will give relatively
precise indications of at what point a patient might be offered
a complementary option and, therefore, clear guidelines to all
the primary care practitioners in that group as to when the work
might be feasible or could be offered within the budget of that
Primary Care Group. Therefore, again you would have that level
of standardisation, whether the treatment was being offered from
the resource centre centrally or whether it was being offered
in an individual practice" (Q 1463).
9.28 The NHS Executive was commissioned by the Department
of Health to produce a report on the key issues relating to CAM
in Primary Care. The report was prepared by drawing together an
information base on CAM in primary care through examining entries
to the Guild of Health Writers' Integrated Healthcare Awards Competition,
and through a questionnaire which was sent to all PCGs (and received
a 60% response rate). The report identified some patterns of PCGs'
commissioning of CAM therapies and important issues for PCGs to
keep in mind. These were:
- CAM occupied a greater or lesser profile within
the PCG depending on local circumstances, e.g. the financial state
of the PCG, need to review continuation of existing services and
having to balance PCG priorities
- Provision of CAM is usually based on the interest
and enthusiasm of particular individuals rather than being part
of an overall strategy of provision of services.
- Where no such therapies were being provided,
about one-fifth of PCGs had plans for provision within the next
2-3 years.
- Factors to be taken into account in the provision
of CAM were:
a) information on effectiveness and cost
effectiveness;
b) knowledge of accreditation procedures and standards for practitioners;
c) the wider resource implications of any decisions made.
- Patients do not necessarily see the NHS as their
provider of access to CAM, but do see NHS healthcare professionals
as an information resource.
- Given the significant number of people requesting
and using CAM treatment it seems that doctors and healthcare professionals
will not only need to be aware of what is available but also be
able to give advice on existing evidence.
9.29 Within this research work[58]
several areas for further work to aid PCGs in making informed
decisions about CAM were identified. In response to these needs
the Department of Health, the NHS Executive and the National Association
of Primary Care collaborated to put together and publish a Complementary
Medicine Information Pack for Primary Care Groups in June
2000. The aim of this pack is to "give primary care groups
a basic reference on complementary and alternative therapies most
commonly provided by PCGs." It includes information on current
levels of provision, on individual therapies and the groups representing
them on how to make referrals to CAM practitioners, and it outlines
existing models of provision as well as identifying further sources
of information. As these were all areas identified by PCGs as
issues upon which they needed guidance it will, we hope, be a
useful resource for PCGs in their practice reviews.
9.30 Another factor that is likely to impact on PCGs'
commissioning patterns is the local Health Improvement Programme.
The Department of Health told us that "Health Improvement
Programmes (HImP) will be the local strategy for improving health
and healthcare. They will cover the most important health needs
of the local population, and how these are to be met by the NHS
and its partner organisations...HImPs that engage all local interests
and which will result in comprehensive LTSAs [Long-Term Service
Arrangements - the replacement of annual contracts as the means
of commissioning services] will take time to develop fully. As
LTSAs develop, patients and their representative groups will be
able to take an active role in influencing commissioning decisions.
Those responsible for commissioning healthcare services will be
required to involve users and carers in identifying local priorities…If
local people and the relevant Primary Care Group, Health Authority
and NHS Trust feel strongly that there is a priority need for
CAM services, those responsible for commissioning services will
need to consider whether these would represent a cost-effective
means of meeting local health needs, consistent with the objectives
of the local HImP" (P 117).
9.31 The newly published Complementary Medicine
Information Pack for Primary Care Groups[59],
previously mentioned, also discusses the role of HImPs in determining
the use of CAM by PCGs. It advises that "Whilst CAM may not
be specifically mentioned in the PCG Health Improvement Plan or
Primary Care Investment Plan (PCIP), the PCG could still have
an interest in how CAM may be integrated into services to improve
the health of the local population. Across the PCG, there will
probably be some variation in the extent to which the local population
may be able to access CAM, usually related more to differences
in local provision rather than patient need. In these circumstances
the PCG will want to consider how the issue of equity of access
for the local population should be addressed…A commissioning
model for PCGs could involve care pathways for a given condition
rather than individual services, providing an opportunity for
CAM to be used and incorporated as an option, especially where
there is evidence of efficacy to support its use."
Gatekeeper Role of GPs
9.32 The gatekeeper role of GPs is traditionally
the route to most specialist care on the NHS; as Box 12 showed,
all NHS CAM provision is currently accessed either through GP
referral or the referral of another member of the primary or secondary
healthcare team. As discussed earlier in this report, one of the
main dangers of CAM is that patients could miss out on conventional
medical diagnosis and treatment because they approached a CAM
practitioner first who did not have the comprehensive medical
training of a medical practitioner. One way of ensuring that this
risk is minimised is to have GPs acting as gatekeepers so that
CAM therapies can only be accessed (on the NHS) if the patient
is referred by their GP or another member of the primary healthcare
team.
9.33 The Royal College of General Practitioners (RCGP)
supported the GP gatekeeper as the route for CAM access on the
NHS. They told us: "The GP is the gatekeeper for many other
services and, of course, if the patient has a particular condition,
then in theory there is no reason why one should not consider
CAM therapy as one of the points of referral...People also see
the GP as somebody who can look at the effectiveness of what is
likely to work for a particular condition. It may be a little
bit difficult to work out the full benefits of a particular treatment
without having a full assessment. It may just be the initial assessment
but in some way co-ordinated" (QQ 1484 & 1490).
9.34 The BMA also envisaged the gatekeeper role as
the best route for CAM access on the NHS: "We would anticipate
that gatekeeper role within the NHS function. So if we are going
to refer or delegate at the expense of the NHS we would expect
it to be the route into that" (Q 378).
9.35 The gatekeeper role of the GP or other member
of the primary healthcare team not only minimises the risk of
failing to diagnose serious problems but also ensures that the
GP is aware of the treatment their patient is getting, and that
all treatment is recorded in patient records. It also encourages
communication between healthcare professionals. Dr Simon Fradd
of the BMA also saw advantages in the gatekeeper role for financial
reasons: "The reason, I would say, for that gatekeeper role
within the NHS is because we have finite resources and we have
to balance that. This comes back to the whole evidence base again.
In my own commissioning group in Nottingham we had to make a decision:
would we buy CAM procedures or would we buy more hip replacements?
In the lack of really clear evidence we bought the hip replacements.
I have a function, not just in clinical gatekeeping but in financial
gatekeeping, and that is why I see a need for a gatekeeper role
within the NHS" (Q 379).
9.36 The gatekeeper role can only be effective in
relation to NHS CAM provision. In the private sector it would
be virtually impossible to have such a requirement to control
CAM access. Even if it were possible, it is unlikely that it would
be desirable. If people wish to access CAM practitioners without
a GP referral, this is their right, as long as they are doing
so privately. In fact, such visits probably aid the NHS, reducing
the burden on an already over-burdened service. If all such patients
were required to go through their GP it would add more pressure
upon busy doctors. However, this does mean that if patients access
CAM privately they may either: (i) not approach a GP first when
they could be seriously ill and may benefit from conventional
treatment; or (ii) they may see their GP but not tell him/her
they are also having CAM treatment, which may interfere with the
treatment which the doctors provide. Therefore it is very important
that CAM practitioners encourage their patients to see their GP
about health problems for which they have not sought a medical
opinion beforehand. It is also important that GPs do not make
patients feel embarrassed about accessing CAM treatments, but
instead encourage openness so as to work with the CAM practitioner
communicating about the patient's progress, etc. The BMA agreed
with this approach, saying they would encourage "…best
practice so that there is communication from the CAM practitioner
to the patient's family doctor, and that would be the very least.
However, I do not think we need to be proscriptive about it, but
we do need the quality controls that we have spent quite a lot
of time talking about today, to protect the public. Also, we need
to make it clear to the public that the medical profession are
behind this; that the public need not feel embarrassed about using
an alternative practitioner" (Q 378).
9.37 We recommend that all NHS provision of CAM
should continue to be through GP referral (or by referral from
doctors or other healthcare professionals working in primary,
secondary or tertiary care).
Criteria for NHS Provision
9.38 One of the questions in our Call for Evidence
asked what level of evidence was needed to justify NHS provision
of CAM.
9.39 We heard much evidence about this matter. Many
submissions suggested that 'only CAM therapies with an adequate
evidence base in their favour should be considered for NHS integration.'
As we discussed in Chapter 3, this is a difficult principle to
apply as an adequate evidence base is hard to define. The Royal
London Homoeopathic Hospital recognised this was a problem and
told us: "As a general rule only therapies which have some
evidence in their support should be introduced, but this should
be interpreted flexibly: it may be necessary to introduce a therapy
with a weak evidence base in NHS settings before it can be adequately
evaluated. Conversely, existing evidence may not be generalisable
to NHS contexts. It would be difficult to define minimum required
standards of evidence in a hard and fast manner" (P 195).
9.40 In the NHS Executive's study on key issues for
CAM in Primary Care[60]
discussed in the previous section, one of the questions put to
the PCGs in the survey was: "What factors are important in
decision-making on the provision of complementary therapies throughout
the PCG?" Respondents were asked to identify the five most
important factors, and the results show that in considering CAM's
role in NHS primary care the most important factors are evidence
of effectiveness and cost-effectiveness, followed by accreditation
procedures and standards (See Figure 1).
Figure 1:
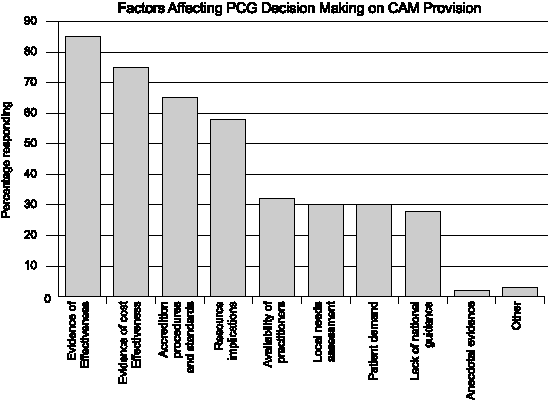
9.41 These findings again stress the importance of
doing more research and gathering more evidence about CAM's effectiveness,
as has been discussed in previous chapters. But the Royal London
Homoeopathic Hospital's point that it may be necessary to introduce
into the NHS new therapies with weak evidence bases in order to
facilitate such research was reiterated by other witnesses.
9.42 The NHS Confederation told us "Integration
in itself will also assist in the process of developing an evidence
base. It is also the most promising way to take forward the matter
of public provision. The NHS Confederation believes there are
several service reasons why CAM should be publicly funded. However
it should be made clear that in the current financial climate,
provision of CAM in the NHS would have to compete with other priorities.
It is likely that these services not backed by good evidence will
be given a low priority" (P 145).
9.43 The NHS Confederation believes that there are
several steps to be taken in deciding the extent of future provision
of CAM. These are:
- "Systematically appraising the evidence
and emerging evidence…alongside any other health technology
assessments. NICE should take the lead in such appraisals.
- "Where an appraisal is promising yet sufficient
evidence is not available…supporting further research and
development work" (P 145).
9.44 One of the prime reasons for integrating CAM
into the NHS will be if it is found to be cost-effective and can
save scarce medical resources. We have heard some evidence that
preliminary studies show that integrated healthcare can be cheaper
than conventional medicine alone but more work needs to be done
in this area. FIM told us: "The amount of work which is done
on cost-effectiveness within the NHS is very limited, similarly,
there is very little which has been done in terms of the cost-effectiveness
of CAM provision. There are some findings to show that it did
result in savings to the NHS. Our view would be that cost-effectiveness
is an area of additional research which should be given attention,
for example, across some of the chronic conditions which could
be alleviated by CAM approaches. We would suggest that certainly
more research needs to be done in this area. It is a very important
one" (Q 112).
9.45 There are also questions of what level of regulation
a therapy, or a practitioner, should be subject to if they are
to work on the NHS. This was discussed in Chapter 5 on Regulation
9.46 We recommend that only those CAM therapies
which are statutorily regulated, or have a powerful mechanism
of voluntary self-regulation, should be made available, by reference
from doctors and other healthcare professionals working in primary,
secondary or tertiary care, on the NHS.
55 Thomas, K. & Luff, D. (April 2000) The Provision
of Complementary Medicine Under Primary Care Groups: Interim Report
to the Department of Health. Medical Care Research Unit, University
of Sheffield. Back
56
Thomas, K. & Luff, D. (2000) (Op.cit.). Back
57
Thomas, K. & Luff, D (2000) (Op.cit.). Back
58
Thomas, K. & Luff, D. (2000) (Op.cit.). Back
59
Thomas, K. & Luff, D. (2000) (Op.cit.). Back
60
Thomas, K. and Luff, D. (2000) (Op.cit.). Back
|