

A Case Report on the Management of a Patient
Presenting With Post-concussion Syndrome and
Post-traumatic Stress Disorder, Using the
Upper Cervical Chiropractic TechniqueThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: Topics in Integrative Health Care 2015 (Mar 31); 6 (1) ~ FULL TEXT
OPEN ACCESS Scott Bales, DC
180 Parsons Rd #11
Alliston, Ontario, Canada L9R1E8Introduction: This case report describes the chiropractic management of a patient with a history of multiple mild traumatic brain injuries, using Upper Cervical manipulative technique.
Clinical Features: A 42 year old man presenting with symptoms of post-concussion syndrome, and diagnosed with post-traumatic stress disorder and depression.
Intervention and Outcome: The Kale Upper Cervical Procedure was utilized to assess, monitor, and correct the effects of an upper cervical subluxation in a patient over an 8 week period. The patient reported significant improvement in symptoms of post- concussion syndrome, and small positive improvements in PTSD symptoms. Follow up at 11 months showed continued improvement in most symptoms.
Conclusion: Upper cervical chiropractic management of a patient with multiple mild traumatic brain injuries was presented. Significant improvements in post-concussion symptoms were observed.
From the FULL TEXT Article:
Introduction
Concussion is defined as a complex pathophysiological process affecting the brain, induced by biomechanical forces. Concussion is often used interchangeably with the term mild traumatic brain injury (mTBI) but is more correctly categorized as a subset of TBI. [1] The majority of concussion injuries are temporary in nature, resolving in 7-10 days, with the acute symptoms reflecting a functional disturbance in neurology rather than structural damage. [1, 2] The established management of acute symptoms is physical and cognitive rest and then graded physical exertion before return to play. [1]
Common characteristics of a concussion injury include physical (headache, dizziness, nausea, visual disturbances, tinnitus, balance disturbance), and cognitive and emotional symptoms (difficulty focusing, fatigue, emotional changes, and irritability). In 10-15% of concussions, symptoms persist beyond 10 days and may not be specific to concussion but to other concomitant injury. [1] Management of post-concussive symptoms include physical and psychological therapies, vestibular and cognitive therapies, as well as assessment of other causes, including upper cervical subluxation. [1, 3]
Military personnel are at increased risk for concussive injury due to their exposure to explosions, falls, and motor vehicle accidents. [4] A review of military personnel deployed to Iraq and Afghanistan estimated 8-20% may have sustained a TBI. [5]
Post-Traumatic Stress Disorder (PTSD) is a mental illness brought on by traumatic exposure to overwhelming stress. The condition is more common in certain occupations such as military personnel, and first responders. Symptoms include nightmares, flashbacks, avoidance behaviors, edginess, irritability, trouble concentrating, poor sleep, and numb, disconnected and detached feelings. [6] The 2004-2005 National Epidemiologic Survey on Alcohol and Related Conditions found a lifetime prevalence of PTSD of 7.3% in the general U.S. population. [7] In contrast, approximately 15% of veterans suffer with PTSD and among those with a history of a traumatic brain injury the rates are much higher. [8, 9]
There are a multitude of factors that influence treatment outcome and as such no single treatment has proven effective for everyone. Cognitive behavioral therapy and selective serotonin reuptake inhibitors are common treatments but have shown non-response rates as high as 50% and 20-40% respectively. [7]
Reports of military personnel suffering with post-concussion and PTSD symptoms have garnered much attention recently. The clinical improvement in these conditions following re-alignment of the cranio-cervical junction that is presented in this case report may shed new light on the management of these conditions.
Case Presentation
The patient was a 42 year old Caucasian male retired from the military after 18 years of service, medically discharged suffering with Post Traumatic Stress Disorder (PTSD) and depression. There was a history of multiple head injuries including 12 concussions as a result of motor vehicle accidents, shell shock from bomb explosions, a collapsed roof, and a severe parachute accident. The parachute accident was a 1200 foot jump with parachute failing to open properly and the patient impacting the ground with such force that both femur heads blew through the pelvis. The patient was in and out of consciousness at the scene of the accident and suffered some retrograde amnesia.
Presenting symptoms included mood swings that quickly changed from normal temperament to that of anger followed by depression. These episodes occurred every 1-2 weeks lasting 1-2 days. Major mood swings occurred once every 4 weeks, lasting 2-3 days in which the patient coped by disassociating from everyone until it passed. He was unaware of any triggers. He did not sleep well, waking every 2 hours. The patient had been prescribed Effexor and Seroquel as well as counseling for his PTSD symptoms. Both were discontinued due to worsening of his symptoms. The only medication he was currently taking was Pantoloc for stomach pain.
The patient competes in strongman competitions which require heavy lifting during training and competition. Lifting requirements include squatting 600+ lbs, deadlifting 600-750 lbs, bench pressing 350-400 lbs, and shoulder pressing 300+ lbs. While performing these extreme lifting exercises the patient reported feeling dizzy during the lift. He also experienced blurred vision and saw white spots that lasted for a few minutes. About a half hour after a workout a headache and nausea develop and within an hour extreme fatigue ensues to the point where he found it hard to stay awake. He became lightheaded and had to lie down. Lying down alleviated the headache and nausea and by the next day he had generally recovered from the workout. The same symptoms occurred during a strongman competition, but he required 4-5 days before fully recovering. Over the past 3 years the patient had competed in 13 amateur strongman competitions, every 4-5 weeks during the summer months. The patient was considering retiring from such competitions due to the severity of his symptoms.
Assessment
The patient was examined for the presence of an upper cervical subluxation [10] using orthopedic, neurological, postural, thermographic instrumentation, and radiographic examinations. The Kale method of Upper Cervical analysis and management were utilized. [11]
Orthopedic tests were unremarkable other than mild weakness bilaterally in the anterior deltoid and hip flexors and this was only noticeable with the head fully rotated to the right. Surface EMG readings along the entire spine were normal. [12] Neurological tests revealed abnormal heart rate variability. [12] Manual visual testing revealed normal smooth pursuit of both eyes but slower than normal saccadic movement both vertically and laterally. There was a very mild convergence insufficiency. Horizontal and vertical gaze stability was impaired.
Postural evaluation revealed an imbalance showing up as right head tilt and a low right shoulder (standing) and a short right leg in the prone position.
Thermographic analysis involves the differential measurement of bilateral paraspinal skin temperature of the cervical spine starting at the level of T1 and gliding up to and under the occiput (Thermographic Scan). The recording pickup is thermocouple based and the software used was the Kale K4. The purpose of the scan was to analyze the neurophysiology of the patient indicating when the upper cervical spine has joint dysfunction (referred to by Doctors of Chiropractic (DC) as “subluxation”). [11]
Thermographic analysis of paraspinal skin temperature has a long history in the Chiropractic profession first introduced with the invention of the Neurocalometer by Dossa Evins in 1922 and developed and refined into a pattern analysis by Dr. B.J. Palmer in the 1930’s. [13] A number of studies have looked at the inter-examiner and intra-examiner reliability of paraspinal skin temperature measurements. [14-16] Plaugher’s study used thermocouple based instruments and found fair to excellent levels of agreement. [15]
The patient’s thermographic analysis revealed a consistent pattern of imbalance. Three thermographic scans were performed on two separate days over a six day period to determine the pattern.
Radiographic Examination
Three cervical x-rays were taken in a seated posture according to the Kale procedure to determine the misalignment vectors of the upper two cervical vertebrae in relation to the foramen magnum of the occiput. The X-ray views taken were a Neutral Lateral, A-P Open Mouth, and Base Posterior. [11, 17]
The neutral lateral cervical x-ray showed a normal lordosis, normal bone integrity and normal joint and soft tissue spacing. The Kale procedure measures the Atlas plane line. The Atlas measured 15 degrees superior to horizontal.
The A-P Open Mouth view is used to measure atlas and axis laterality relative to the foramen magnum (FM), and axis spinous rotation relative to its body. A horizontal line drawn through the anterior portion of the FM is bisected and represents the approximate center of the FM. The axis vertebra (C2) measured 1mm to the right of this line at its base and 1.5mm at the spinous process. The Atlas vertebra (C1) measured 1mm to the right of this line. The Base Posterior view showed less than 1mm of rotation of the atlas, anterior on the right side. Figure 1 is a diagrammatic representation of the misalignment measurements obtained from the radiographic examination.
Intervention
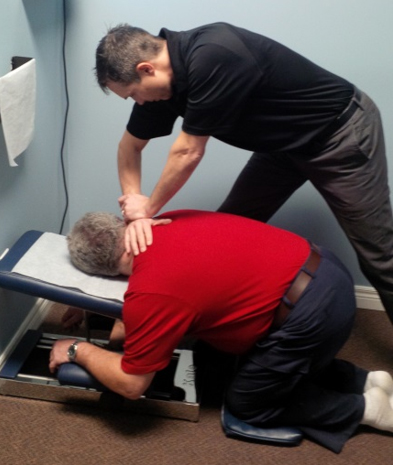
The patient was treated according to the Kale procedure protocol. [11] Treatment consisted of a thermographic scan followed by an adjustment when the established thermographic pattern of imbalance was present. The patient was adjusted in the knee-chest posture on a solid head-piece table. [11] The knee-chest posture consists of the patient kneeling on a small pad on the floor, knees perpendicular to the thighs and thighs parallel to the floor. The head and shoulders are placed on the front of the table. The head is rotated so the ear and mastoid process are flat on the table. In this case the patient’s head was rotated to the right placing the left ear and mastoid process on the table (Figure 2). The adjustment is a low force, body drop-toggle recoil.
Figure 1. Diagram of the upper cervical misalignment in this case.

Figure 2. Depiction of the set up for a knee-chest adjustment.
The patient was initially assessed twice weekly for 8 weeks. All adjustments were delivered to the second cervical vertebra (C2).
It should be noted that the patient was also under prior and concurrent therapy for musculoskeletal injuries by a DC and an acupuncturist. The chiropractic care had been ongoing for approximately 6 years treating low back and hip tightness and discomfort. The acupuncture care had been ongoing for approximately 2 years treating inflammation in the low back and right shoulder. The patient reported that neither the chiropractic or acupuncture treatment had any effect on his post-concussion or PTSD symptoms.
Outcomes
During the eight weeks of treatment the patient was able to continue to train intensively and competed in a professional strongman competition. During the competition he experienced no nausea, headache, blurred vision, or fatigue. His only symptom was slight light-headedness.
At 11 months follow-up he continues to no longer suffer from his workout-symptoms. Concurrently he had found improvement in his sleep, waking only every 3-4 hours. Mood swings still occur but less frequently, 1-2 per month and a major mood swing occurring only once every 4-6 weeks. Some of the time the mood swings no longer involve anger but swing straight to depression.
All abnormal orthopedic and neurological tests have shown improvement or complete resolution with the exception of the visual deficiencies. Home exercise rehabilitation for these deficiencies has been prescribed.
Discussion
The majority of concussion symptoms resolve in 7-10 days. When they persist beyond this time period it is often the result of other processes such as cervical spine injuries. [1] It’s well known that upper cervical spine injuries can mimic symptoms of concussion and post-concussion syndrome. [18] The complex and intimately connected anatomy of the cranio-cervical junction may allow injury to this area to affect cranial hemodynamics and the central nervous system. The medullaspinalis is directly attached to the dura matter via the dentate ligaments, and the dura matter then attaches to the suboccipital muscles via myodural bridges and the internal boney margins of the atlas, axis and foramen magnum. [19, 20] Misalignment of the cranio-cervical junction might create a torqueing of the dural structures causing occlusion of the vertebral canal. Occlusion of the vertebral canal could cause abnormalities in the pressure and flow of fluids into and out of the skull. Much like the effect of a Chiari malformation, this situation could cause neural damage due to mechanical forces and ischemia. [21]
Increased sympathetic activity and decreased parasympathetic activity compared to controls have been observed in concussed athletes, and the autonomic dysregulation was proportional to the severity of the injury and improved with recovery. [18] Cerebral blood flow and its autoregulation are also disturbed following concussion. [18] Although the autonomic nervous system (ANS) may be diffusely distributed throughout the brain its primary control center is located within the brainstem. It is hypothesized that head injury or trauma to the upper cervical spine may damage this center. [18] Abnormalities in cerebrospinal fluid (CSF) flow have also been observed as a result of misalignment and pathology in the cervical spine. [22] Extravascular compression of the internal jugular vein by the transverse processes of the upper cervical vertebrae has been observed as well. [23]
Since misalignment of the upper cervical spine may be associated with neurological and vascular abnormalities, the reduction of misalignment may result in the resolution of those abnormalities. A 23 year old female with post-concussion syndrome found relief from headache and vertigo symptoms following upper cervical realignment. [3]
Exercise and physical exertion typically exacerbate concussion symptoms. [18] When performing activities that involve lifting extreme amounts of weight, a Valsalva-like maneuver is often used. The Valsalva maneuver is known to cause an increase in intracranial pressure and is sometimes used to evaluate Chiari malformations. [24, 25] Flow velocity in the superior sagittal sinus is also known to decrease during the Valsalva maneuver. [26] The increase in intracranial pressure is thought to result from impedance to normal venous drainage of the head as a Valsalva maneuver causes a significant increase in pressure inside the thoracic cavity. [25]
Altered venous drainage and lowered intracranial compliance was observed in a cohort of patients with mTBI. [27] The mTBI cohort showed significantly higher venous outflow through these secondary venous pathways. [27] In the upright posture, non-jugular valve-less venous pathways predominate the drainage of the skull. [27] It is reasonable to think that such a cohort may have an increased sensitivity to further increases in intracranial pressure from a Valsalva maneuver.
The clinical improvement that coincided with the correction in the alignment of the subluxated vertebra may be a result of the reduction in this canal occluding lesion, and subsequent improvement in both neurological function and fluid dynamics within the CNS.
Limitations
As this is a case report in cannot determine cause and effect as it lacks a comparison group. Also, standardized outcome measurements were not used to quantify pre and post symptom profiles and quality of life changes.
Further investigation into the effect of upper cervical subluxation on cranio-cervical fluid dynamics in the CNS is warranted.
References
McCrory P, Meeuwisse WH, Aubry M et al.
Consensus statement on concussion in sport: the 4th international conference on concussion in sport held in Zurich, November 2012.
Br J Sports Med 2013;47:250-258.Signoretti S, Lazzarino G, Tavazzi B, Vagnozzi R.
The pathophysiology of concussion.
Phys Med Rehabil 2011;3:359-368.Mayheu A, Sweat M.
Upper Cervical Chiropractic Care of a Patient with Post Concussion Syndrome,
Positional Vertigo, and Headaches
J Upper Cervical Chiropr Res 2011 (Jan 6): 3-9Bryan CJ.
Repetitive traumatic brain injury (concussion) increases severity of sleep disturbance among deployed military personnel.
National Center for Veterans Studies, Salt Lake City, UT.
http://dx.doi.org?10.5665/sleep.2730Tanielian T, Jaycox LH.
Invisible Wounds of War: Psychological and Cognitive Injuries, Their Consequences, and Services to Assist Recovery.
Santa Monica, CA: Rand Corporation; 2008Canadian Mental Health Association.
Internet. http://www.cmha.ca/mental health/post-traumatic-stress-disorderBoard of Health of Select Populations; Institute of Medicine.
Treatment for Posttraumatic Stress Disorder in Military and Veteran Populations: Final Assessment Committee on the Assessment of Ongoing Efforts in the Treatment of Posttraumatic Stress Disorder.
Washington (DC): National Academics Press (US); 2014.O’Neil ME, Carlson K, Storzbach D, et al.
Complications of Mild Traumatic Brain Injury in Veterans and Military Personnel:
A Systematic Review
Washington (DC): Department of Veterans Affairs (US), Jan 2013.Theeler BJ, Erickson JC.
Mild head trauma and chronic headaches in returning US soldiers.
Headache 2009;49:529-534.Palmer BJ.
The Subluxation Specific The Adjustment Specific.
Davenport IA: Palmer School of Chiropractic; 1934.Kale MU.
Kale Certification Residency Course.
Copyright 1988. Spartanburg SC.INSiGHT Subluxation StationTM, Discovery Model.
Chiropractic Leadership Alliance.Palmer BJ.
Fight To Climb.
Davenport IA: Palmer School of Chiropractic; 1950.Owens EF, Hart JF, Donofrio JJ, Haralambous J, Mierzejewski E.
Paraspinal Skin Temperature Patterns: An Interexaminer and Intraexaminer Reliability Study
J Manipulative Physiol Ther 2004 (Mar); 27 (3): 155-159Plaugher G, Lopes MA, Melch PE, Cremata EE.
The inter and intraexaminer reliability of a paraspinal skin temperature differential instrument.
J Manipulative Physiol Ther 1991;14(6):361-7.McCoy M, Campbell I, Stone P, Fedorchuk C, Wijayawardana S, Easley K.
Intra-Examiner and Inter-Examiner Reproducibility of Paraspinal Thermography
PLos One 2011 (Feb 11); 6 (2): 1-10Remier, PA.
Modern X-ray Practice and Chiropractic Spinography. 3rd ed.
Davenport IA: Palmer School of Chiropractic; 1957.Leddy JJ, Sandhu H, Sodhi V, Baker JG, Willer B.
Rehabilitation of concussion and post-concussion syndrome.
Sports Health 2012;4(2):147-154.Enix DE, Scali F, Pontell ME.
The cervical myodural bridge, a review of literature and clinical implications
J Can Chiropr Assoc 2014 (Jun); 58 (2): 184-192Ericksen K, Rochester RP.
Orthospinology Procedures: An Evidence Based Approach to Spinal Care.
Philadelphia. Lippincott Williams & Wilkins, 2007.Williams H.
A unifying hypothesis for hydrocephalus, Chiari malformation, syringomyelia, anencephaly and spina bifida.
Cerebrospinal Fluid Res. 2008;5(7):1-11.Damadian RV, Chu D.
The possible role of cranio-cervical trauma and abnormal CSF hydrodynamics in the genesis of multiple sclerosis.
Physiol Chem Med NMR 2011;41:1-17.Djorde R, Nenad I, Jovo K, et al.
Incidence and distribution of extravascular compression of extracranial venous pathway in patients with chronic cerebrospinal venous insufficiency and multiple sclerosis.
Phlebology 2013;0(0):1-4.Wostyn P, Audenaert K, De Deyn PP.
The Valsalva maneuver and Alzheimer’s disease: is there a link?
Curr Alzheimer Res. 2009;6(1):59-68.Valsalva Maneuver, Internet.
Cited August 2014 http://en.wikipedia.org/wiki/valsalva_maneuver.Pomschar A, Koerte I, Lee S et al.
MRI Evidence for Altered Venous Drainage and Intracranial Compliance in Mild Traumatic Brain Injury
PLoS One. 2013 (Feb 6); 8 (2): e55447Kuriyama N, Tokuda T, Yamada K, et al.
Flow velocity of the superior sagittal sinus is reduced in patients with idiopathic normal pressure hydrocephalus.
J Neuroimaging 2011;21(4):365-9
Return to CASE STUDIES
Return to MILD TRAUMATIC BRAIN INJURY
Since 5-22-2015


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |