

Radiographic Sagittal Alignment and Kinetic Chain
Alterations in Geriatric Patients With Scoliosis:
A Case SeriesThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: Cureus 2026 (Mar 25); 18 (3): e105827 ~ FULL TEXT
OPEN ACCESS John P Whelan, Justin M Dick
Physical Medicine and Rehabilitation,
Clear Life Scoliosis and Chiropractic Center,
Charlotte, USA.
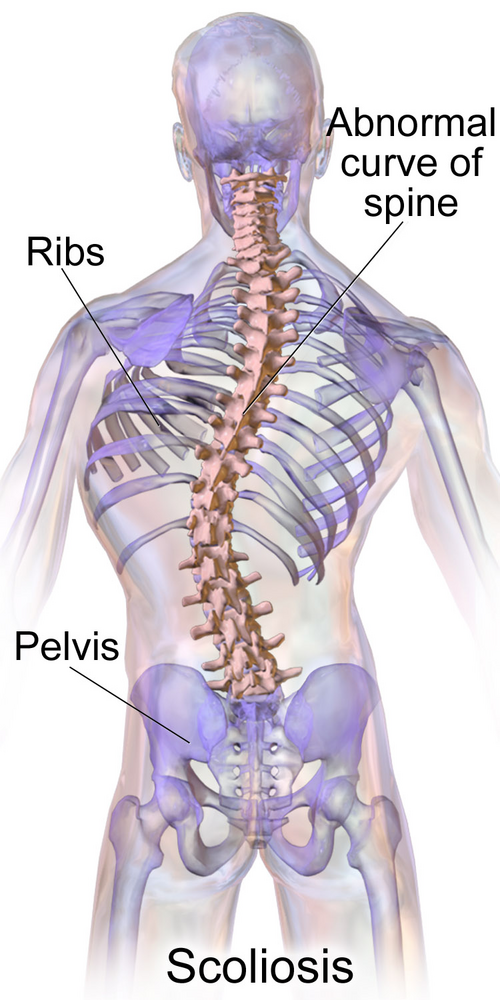
Adolescent idiopathic scoliosis (AIS) is a three-dimensional spinal deformity that originates in adolescence but carries lifelong biomechanical consequences. In geriatric patients, chronic pain associated with a history of AIS is frequently attributed to the scoliotic curve itself. This case series proposes an alternative framework. Pain in this population may originate from long-term kinetic chain dysfunction and accelerated degeneration driven by decades of compensatory biomechanical loading.
Two geriatric subjects with a history of AIS and chronic pain presented to a private chiropractic clinic. Both underwent a multimodal non-surgical spinal rehabilitation program based on the CLEAR Institute protocol. Pre- and post-treatment radiographic measurements and self-reported outcomes were assessed. Both patients demonstrated clinically meaningful reductions in pain and measurable improvements in sagittal spinal alignment following treatment.
These cases suggest that in geriatric patients with AIS, chronic deficits may be more closely related to kinetic chain dysfunction and compensatory degeneration than to the primary scoliotic curve. A non-surgical, multimodal rehabilitation approach targeting global spinal alignment can yield significant clinical improvement. Larger prospective studies are needed to evaluate this hypothesis further.
Keywords: adolescent idiopathic scoliosis (ais), adult idiopathic scoliosis, complete kinetic chain, geriatric physical therapy, non-surgical rehabilitation, spinal degeneration
From the FULL TEXT Article:
Introduction
Adolescent idiopathic scoliosis (AIS) is a structural, three-dimensional spinal deformity defined by a lateral curvature of 10 degrees or greater accompanied by vertebral rotation and trunk asymmetry. [1] It typically presents between the ages of 10 and 17 and affects approximately 2 to 3 percent of adolescents, with a marked predominance in females. [2, 3] Curve progression most commonly coincides with periods of rapid pubertal growth. Left untreated, AIS can lead to pain, progressive deformity, and psychological distress related to body image and disability. [3]
The long-term natural history of AIS extends well beyond skeletal maturity. Spinal curves, particularly those exceeding 50 degrees, have been shown to continue progressing into adulthood. [4] The prevalence of scoliosis in the general population increases sharply with age. Population studies report rates as high as 68 percent in individuals between 60 and 90 years old, a figure that includes both de novo degenerative scoliosis and the progression of pre-existing AIS. [5] This convergence of adolescent deformity and age-related degeneration creates a clinically complex presentation in older adults. The primary source of pain in these patients is often difficult to determine.
Scoliosis should also be understood within the context of the kinetic chain. The cervical spine, thoracic spine, lumbar spine, pelvis, and lower extremities function as an integrated biomechanical unit. A structural deformity in one spinal region does not remain regionally confined. It obligates compensatory adaptations throughout the entire chain to preserve sagittal balance, horizontal gaze, and ambulatory function. These compensations may involve altered cervical curvature, thoracolumbar junctional remodeling, pelvic obliquity, asymmetric lower-extremity loading, and gait deviations. Such strategies will become maladaptive over time. This results in chronic asymmetric loading across discs, facet joints, ligaments, and myofascial tissues. This persistent mechanical inefficiency may accelerate degenerative change, promote segmental instability, and contribute to progressive pain and dysfunction in areas both adjacent to and distant from the primary scoliotic deformity.
Published literature demonstrates that patients with adolescent idiopathic scoliosis frequently exhibit abnormal cervical mechanics, including hypolordosis, instability, and cervical buckling patterns, suggesting that the biomechanical impact of scoliosis extends well beyond the primary coronal curve. [6] As these compensatory patterns accumulate over decades, they may progressively reduce functional reserve and impair the body’s ability to tolerate normal mechanical demands. This decline can contribute to diminished tolerance for standing, walking, lifting, and other activities of daily living. Additional evidence has documented that restoration of sagittal spinal alignment in patients with complex spinal histories, including prior surgery and pre-existing scoliosis, is associated with meaningful reductions in pain and disability. [7, 8]
This case series aims to describe the clinical presentation, radiographic findings, and treatment outcomes of two geriatric female patients with a history of AIS who presented with chronic functional deficits. We propose that deficits were not only a direct consequence of the scoliotic curve but rather the result of long-term kinetic chain dysfunction. Both patients presented consecutively for scoliosis-specific care using the CLEAR Institute treatment protocols and monitored with a subjective functional rating index and objective radiographs. [1, 9–13]
Case presentation
Case 1
A 74–year-old female presented with a known history of AIS and chronic lower back pain with intermittent radiation into her right lower extremity. She rated her pain as a 6 out of 10 on a numeric pain scale. The pain was a constant dull ache that worsened with prolonged standing or walking. The patient's gait was severely disrupted. She used a walking cane to assist in ambulation and reported a history of falls and a subjective feeling of instability with ambulation. No prior care was tried for her scoliosis or gait abnormalities. Surgical intervention was recommended. Her primary goals were to manage her pain and improve her balance.

Table 1 Physical examination revealed a left lumbar prominence and mild trunk shift to the left. Paraspinal musculature was hypertonic in the left lumbar region. Bilateral piriformis syndrome was noted upon palpation, which increased pain. Bilateral posterior superior iliac spine (PSIS) palpation induced pain. Postural assessment demonstrated a forward head posture. Anterior hip rotation was noted on the posture evaluation. Orthopedic testing was negative for significant radiculopathy on examination. She reported intermittent lower extremity radicular symptoms with walking (Table 1).
Intervention
Following an initial evaluation, Case 1 completed a spinal corrective program consisting of 20 in-office sessions (3 sessions per week spanning 7 consecutive weeks). The CLEAR™ Institute’s “Mix-Fix-Set” model of care was utilized. Each session lasted approximately 120 minutes and was supervised by a licensed chiropractor trained in scoliosis biomechanics through the CLEAR™ Institute.
Results

Figure 1

Table 2

Figure 2

Table 3 Paraspinal musculature continued to be hypertonic in the left lumbar region. Pain associated with previously documented bilateral piriformis syndrome was reduced. Bilateral PSIS palpation did not induce pain. She reported the ability to ambulate without the use of a cane. She reported that she felt more "stable" on her feet. She reported she could resume activities of daily living but was unable to farm.
Radiographic evaluation was performed on July 10, 2023, of weight-bearing radiographs. The anteroposterior view demonstrated moderate left lumbar scoliosis. The Cobb angle measured 23.3 degrees at initial presentation and reduced to 20.9 degrees (Figure 1, Table 2). Quantitative cervical and lumbopelvic spine changes were measured to assess structural outcomes utilizing PostureRay (PostureCo, Inc., Trinity, FL). This is a machine learning-assisted parameter measurement. Radiographic line-drawing methods have demonstrated high inter- and intra-examiner reliability and are comparable to manual measurements across spinal regions. Measurements were compared with normative values and baseline imaging to determine the degree of anatomical correction. All images and analysis were completed by the same physician.
Sagittal analysis of the lateral cervical projection revealed a cervical kyphosis. The absolute rotation angle (ARA) of C2–C7 measured –9.2 degrees, a significant deviation from the normative value of –42.0 degrees. Forward head posture measured 25.9 mm of anterior translation (Figure 2, Table 3). These findings demonstrate a complex, multi-regional spinal deformity with significant sagittal and coronal imbalances, consistent with loss of cervical lordosis and age-related degenerative progression.
Case 2
A 60–year-old female presented with a long-standing history of idiopathic scoliosis. The patient reported chronic debilitating lower back pain with ambulation only. She rated her pain as 0 out of 10 on a numeric pain scale statistically. Her abnormal gait was constant and significantly limited her ability to perform daily activities, as this induced pain. Surgical intervention was recommended. No prior care was tried for her scoliosis or gait abnormalities.
Physical examination revealed significant trunk asymmetry with a right thoracic prominence and an elevated right shoulder. Paraspinal musculature was hypertonic bilaterally, with greater tension on the right (Table 1). Bilateral piriformis syndrome was noted with increased pain upon palpation. Bilateral PSIS palpation induced pain. Postural assessment demonstrated a forward head posture. Anterior hip rotation was noted on the posture evaluation. Orthopedic and neurological testing was otherwise unremarkable. The patient's gait was severely disrupted.
Intervention

Figure 3

Table 4

Figure 4

Table 5 The patient completed a two-month course (three sessions per week spanning seven consecutive weeks) of scoliosis-specific chiropractic care following the CLEAR Institute protocol. This multimodal program incorporated spinal adjustments, scoliosis-specific rehabilitative exercises, and spinal traction. The CLEAR protocol is a structured, evidence-informed approach to non-surgical scoliosis management that integrates mechanical traction, proprioceptive neuromuscular re-education, and corrective exercise to address the three-dimensional nature of scoliotic deformity.
Results
Paraspinal musculature continued to be hypertonic in the left lumbar region. Previously noted bilateral piriformis syndrome demonstrated reduced pain. Bilateral PSIS palpation did not induce pain. Clinically, she reported the ability to walk without pain for longer distances. She also reported a marked improvement in her ability to perform daily activities while standing.
Follow-up radiographs were obtained on April 4, 2024. The thoracolumbar Cobb angle reduced from 74.0 degrees to 71.1 degrees (Figure 3, Table 4).
The cervical ARA improved from 2.1 degrees to –20.4 degrees, representing a normalization toward the expected lordotic curvature. Forward head posture decreased from 19.7 mm to 15.5 mm (Figure 4, Table 5).
Discussion

Figure 5 This case series presents two geriatric female patients with long-standing adolescent idiopathic scoliosis who experienced significant clinical improvement following a non-surgical rehabilitation program through the CLEAR Institutes' protocols (Figure 5). [12]
The central finding is not simply that treatment was effective. It is that the most clinically meaningful improvements occurred in the sagittal plane and kinetic chain. This is seen specifically in cervical alignment and forward head posture, rather than in the primary coronal scoliotic curve. The kinetic chain combination of the lumbar extensors, hip extensors, and piriformis activation created much of the imbalance and associated symptoms. This pattern of response supports the hypothesis that the pain in these patients was driven primarily by kinetic chain dysfunction and compensatory degeneration, not by the scoliotic curve itself. This observation is critical, as the relationship between back pain and the magnitude of the scoliotic curve in adults is inconsistent, suggesting other factors are at play. [14–17]
Both patients, despite having different Cobb magnitudes, presented with strikingly similar and severe sagittal plane deformities. Case 1 presented with a cervical ARA of 2.1 degrees, a near-complete inversion of the normal cervical lordosis. Case 2 presented with a cervical ARA of –9.2 degrees and a forward head posture of 25.9 mm. These findings are consistent with a whole-body compensatory strategy in which the cervical spine undergoes progressive kyphotic deformation to maintain horizontal gaze in the presence of a primary thoracolumbar or lumbar deformity. [18, 19] Prior retrospective cross-sectional analysis of 37 patients with AIS from this clinic demonstrated that all participants exhibited a loss of cervical lordosis. [6] The two cases presented here are consistent with this pattern and extend it to a geriatric population where sagittal malalignment is a known contributor to pain, functional decline, and increased fall risk. [19–21]
The kinetic chain concept provides the theoretical framework for understanding why this compensatory cervical deformity is clinically significant. Decades of abnormal cervical kyphosis and forward head posture generate chronic, elevated tensile and compressive loads on the cervical and upper thoracic musculature, facet joints, intervertebral discs, and ligamentous structures. [22–26] These loads accelerate degenerative changes, including facet joint osteoarthritis and fatty infiltration of paraspinal muscles, and create a persistent nociceptive environment. [27–31] The body then adapts the lower trunk and into the lower extremities. Over time, pain may develop as a downstream consequence of chronic biomechanical dysfunction throughout the kinetic chain, not a direct symptom of the scoliotic curve. This distinction has important implications for treatment. A strategy focused solely on reducing the Cobb angle may fail to address the actual source of symptoms. [14]
The outcomes observed in these two cases align with findings from the literature on conservative scoliosis care. [7, 8, 11, 32] The CLEAR Institute protocol used in both cases is a structured, multimodal approach to non-surgical scoliosis management that has been shown to produce positive outcomes. [1, 9–11] The present cases suggest that in geriatric patients, the protocol's effects on sagittal alignment and the kinetic chain may be particularly relevant to pain outcomes and an increase in the ability to perform activities of daily living. The reduction in forward head posture observed in Case 2, from 25.9 mm to 11.9 mm, is a clinically substantial change that likely reduced the chronic mechanical burden on the cervical spine and is a contributor to the resolution of symptoms. [26]
This case series has several important limitations. The sample size of two patients precludes generalization. No control group was included. Functional outcome measures beyond self-reported pain intensity were not systematically collected. The minimal clinically important difference (MCID) of approximately 9 points of the functional rating index was not achieved. [33] The follow-up period was limited to two months. Longer-term follow-up data would be necessary to determine whether the radiographic and clinical improvements observed are sustained. Despite these limitations, the cases provide a coherent and clinically meaningful illustration of the kinetic chain dysfunction hypothesis in geriatric AIS patients. They also demonstrate that non-surgical rehabilitation targeting global spinal alignment may be feasible and potentially effective in this population. [32, 34–35]
Conclusions
This case series suggests that in geriatric patients with AIS, chronic pain may be more closely related to kinetic chain dysfunction and compensatory sagittal deformity than to the primary scoliotic curve. These findings underscore the importance of assessing global spinal biomechanics in this population. A non-surgical, multimodal rehabilitation program based on the CLEAR Institute's protocol produced clinically meaningful reductions in pain and measurable improvements in sagittal spinal alignment in both patients. These findings support the hypothesis that treatment in this population should prioritize restoration of global biomechanical function. Larger prospective studies are needed to confirm these observations and to characterize the long-term durability of non-surgical rehabilitation in geriatric patients with AIS.
Human subjects:
Informed consent for treatment and open access publication was obtained or waived by all participants in this study.
Conflicts of interest:
In compliance with the ICMJE uniform disclosure form, all authors declare the following:
Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work.
Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work.
Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Author Contributions
Concept and design: Acquisition, analysis, or interpretation of data:, Drafting of the manuscript:, Critical review of the manuscript for important intellectual content:, Supervision:
Justin M. Dick, John P. Whelan
References
A non-surgical multimodal approach to adolescent idiopathic scoliosis (Lenke 5C) using an intensive two-week CLEAR Institute protocol: a report of two cases.
Whelan J, Paige P, Dick JM.
Cureus. 2026;18:0.
doi: 10.7759/cureus.102006.Epidemiology of adolescent idiopathic scoliosis.
Konieczny MR, Senyurt H, Krauspe R.
Child Orthop. 2013;7:3–9.
doi: 10.1007/s11832-012-0457-4.Adolescent idiopathic scoliosis: common questions and answers.
Kuznia AL, Hernandez AK, Lee LU.
https://www.aafp.org/pubs/afp/issues/2020/0101/p19.html
Am Fam Physician. 2020;101:19–23.Health and function of patients with untreated idiopathic scoliosis: a 50-year natural history study.
Weinstein SL, Dolan LA, Spratt KF, Peterson KK, Spoonamore MJ, Ponseti IV.
AMA. 2003;289:559–567.
doi: 10.1001/jama.289.5.559Adult scoliosis: prevalence, SF-36, and nutritional parameters in an elderly volunteer population.
Schwab F, Dubey A, Gamez L, El Fegoun AB, Hwang K, Pagala M, Farcy JP.
Spine (Phila Pa 1976) 2005;30:1082–1085
doi: 10.1097/01.brs.0000160842.43482.cd.A retrospective cross-sectional analysis of abnormal cervical mechanics in patients with scoliosis. 5
Dick JM. Cureus. 2025;17:0.
doi: 10.7759/cureus.91098.Radiographic sagittal alignment and neurological changes following conservative cervical structural rehabilitation after motor vehicle collision in a patient with pre-existing scoliosis: a case report.
Dick JM, Paige P. Cureus. 2026;18:0.
doi: 10.7759/cureus.104584.Refractory lumbar pain following motor vehicle collision in a geriatric patient with prior lumbar surgery: clinical resolution after multimodal conservative spinal structural rehabilitation.
Dick JM.
Cureus. 2026;18:0.
doi: 10.7759/cureus.103540.Reduction of adolescent idiopathic scoliosis: a 13-month follow-up.
Dick JM, Spurgeon S. Cureus. 2025;17:0.
doi: 10.7759/cureus.78669.Reduction of adolescent idiopathic scoliosis utilizing the labyrinthine righting reflex: a case report.
Dick JM, Whelan J.
Cureus. 2026;18:0.
doi: 10.7759/cureus.101343Morningstar MW.
Outcomes For Adult Scoliosis Patients Receiving Chiropractic Rehabilitation:
A 24-month Retrospective Analysis
J Chiropractic Medicine 2011 (Sep); 10 (3): 179–184Chiropractic treatment of idiopathic scoliosis with the CLEAR Institute method: a description of the protocol.
Woggon A, Martinez D.
Scoliosis. 2013;8:0.Measurement properties of the Functional Rating Index: a systematic review and meta-analysis.
Bai Z, Shu T, Lu J, Niu W.
Spine (Phila Pa 1976) 2018;43:0–9.
doi: 10.1097/BRS.0000000000002690.Differential diagnosis of back pain in adult scoliosis (non operated patients)
Rigo M.
Scoliosis. 2010;5:0.The impact of lumbar scoliosis on pain, function and health-related quality of life in postmenopausal women.
Urrutia J, Espinosa J, Diaz-Ledezma C, Cabello C.
Eur Spine J. 2011;20:2223–2227.
doi: 10.1007/s00586-011-1829-z.Current knowledge on the different characteristics of back pain in adults with and without scoliosis: a systematic review.
Zaina F, Marchese R, Donzelli S, Cordani C, Pulici C, McAviney J, Negrini S.
J Clin Med. 2023;12:5182.
doi: 10.3390/jcm12165182.Compensatory mechanisms contributing to keep the sagittal balance of the spine.
Barrey C, Roussouly P, Le Huec JC, D'Acunzi G, Perrin G.
Eur Spine J. 2013;22 Suppl 6:0–41.
doi: 10.1007/s00586-013-3030-zAnalysis of compensatory mechanisms in the pelvis and lower extremities in patients with pelvic incidence and lumbar lordosis mismatch.
Cheng X, Zhang K, Sun X, Zhao C, Li H, Zhao J.
Gait Posture. 2017;56:14–18.
doi: 10.1016/j.gaitpost.2017.04.041The association between whole body sagittal balance and risk of falls among elderly patients seeking treatment for back pain.
Kim J, Hwang JY, Oh JK, Park MS, Kim SW, Chang H, Kim TH.
Bone Joint Res. 2017;6:337–344.
doi: 10.1302/2046-3758.65.BJR-2016-0271.R2Influence of spinal sagittal alignment, body balance, muscle strength, and physical ability on falling of middle-aged and elderly males.
Imagama S, Ito Z, Wakao N, et al.
Eur Spine J. 2013;22:1346–1353.
doi: 10.1007/s00586-013-2721-9.Postural sway in older patients with sagittal imbalance and young adults during local vibratory proprioceptive stimulation.
Ito T, Sakai Y, Yamazaki K, et al.
Healthcare (Basel) 2021;9:210.
doi: 10.3390/healthcare9020210Accelerated intervertebral disc degeneration in scoliosis versus physiological ageing develops against a background of enhanced anabolic gene expression.
Bertram H, Steck E, Zimmerman G, Chen B, Carstens C, Nerlich A, Richter W.
Biochem Biophys Res Commun. 2006;342:963–972.
doi: 10.1016/j.bbrc.2006.02.048Mechanical conditions that accelerate intervertebral disc degeneration: overload versus immobilization.
Stokes IA, Iatridis JC.
Spine (Phila Pa 1976) 2004;29:2724–2732.
doi: 10.1097/01.brs.0000146049.52152.daCorrelation between kinematic sagittal parameters of the cervical lordosis or head posture and disc degeneration in patients with posterior neck pain.
Lee HJ, Jeon DG, Park JH.
Open Med (Wars) 2021;16:161–168.
doi: 10.1515/med-2021-0219Chu EC, Lo FS, Bhaumik A.
Plausible Impact of Forward Head Posture
on Upper Cervical Spine Stability
J Family Med Prim Care 2020 (May 31); 9 (5): 2517–2520The relationship between forward head posture and neck pain: a systematic review and meta-analysis.
Mahmoud NF, Hassan KA, Abdelmajeed SF, Moustafa IM, Silva AG.
Curr Rev Musculoskelet Med. 2019;12:562–577.
doi: 10.1007/s12178-019-09594-y.Aberrant spinal mechanical loading stress triggers intervertebral disc degeneration by inducing pyroptosis and nerve ingrowth.
Fu F, Bao R, Yao S, et al.
Sci Rep. 2021;11:772.
doi: 10.1038/s41598-020-80756-6.Axial rotation and pain are associated with facet joint osteoarthritis in adolescent idiopathic scoliosis.
Bisson DG, Sheng K, Kocabas S, et al.
Osteoarthritis Cartilage. 2023;31:1101–1110.
doi: 10.1016/j.joca.2023.03.007Paraspinal muscle pathophysiology associated with low back pain and spine degenerative disorders.
Noonan AM, Brown SH.
JOR Spine. 2021;4:0.
doi: 10.1002/jsp2.1171.Correlation between the fatty infiltration of paraspinal muscles and disc degeneration and the underlying mechanism.
Shi L, Yan B, Jiao Y, Chen Z, Zheng Y, Lin Y, Cao P.
BMC Musculoskelet Disord. 2022;23:509.
doi: 10.1186/s12891-022-05466-8.Biological principles of adult degenerative scoliosis.
Petrosyan E, Fares J, Lesniak MS, Koski TR, El Tecle NE.
Trends Mol Med. 2023;29:740–752.
doi: 10.1016/j.molmed.2023.05.012.Conservative treatment in adult degenerative scoliosis: a prospective cohort study.
Bayram F, Karatekin BD, Erhan B, Pasin O, Yumusakhuylu Y.
Maedica (Bucur) 2024;19:23–29.
doi: 10.26574/maedica.2024.19.1.23.Psychometric properties of the functional rating index in patients with low back pain.
Childs JD, Piva SR.
Eur Spine J. 2005;14:1008–1012.
doi: 10.1007/s00586-005-0900-z.Scoliosis bracing and exercise for pain management in adults-a case report.
Weiss HR, Moramarco K, Moramarco M.
J Phys Ther Sci. 2016;28:2404–2407.
doi: 10.1589/jpts.28.2404.Adult scoliosis: therapeutic approach and spinal pain management.
Kontopanou M, Benetos IS, Pneumaticos SG, et al.
https://eexot-journal.com/aoet/article/view/293
Acta Orthopaedica et Traumatologica Hellenica. 2022;73:306–312.
Return to SCOLIOSIS
Return to SPINAL PAIN MANAGEMENT
Since 4-30-2026


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |