
Guideline Title:
New Zealand Acute Low Back Pain Guide
This guide provides an evidence based approach to the assessment and treatment of acute low back pain, for the prevention of chronic pain and disability. It follows an extensive review of the international literature, and wide consultation with professional groups in New Zealand. The guide is to be used in conjunction with the Guide to Assessing Psychosocial Yellow Flags in Acute Low Back Pain: Risk Factors for Long-Term Disability and Work Loss.
This guide has been developed from the
comprehensive publication Clinical Practice Guideline - Acute Low Back
Problems in Adults: Assessment and Treatment, which was distributed by
ACC and the National Health Committee in January 1996. The
participation of various professional groups, through submissions and
a health professionals’ hearing, enabled an expert panel to
develop this guide. The guide reflects current best practice in New
Zealand and will be reviewed as new evidence becomes available. The
expert panel recommends that this guide should have its first review
within 2 years of publication.
Any further comments and
submission of new evidence for the National Health Committee and ACC
should be made through the appropriate professional association.
No
references are provided in this document. Comprehensive lists of
references are available in the documents detailed in the
acknowledgment at the end of this guide.
| Acute low back pain is |
|
| Recurrent low back pain is |
|
| Chronic low back pain is |
|
| This guide: |
|
This guide is based on a review of the best available scientific evidence for improved clinical outcomes, in accordance with the approach to systematic reviews recommended by the international Cochrane Collaboration.
The advice in the guide is based on 'at least moderate research evidence', where moderate research evidence is defined as one relevant high quality scientific study or multiple adequate scientific studies of an acceptable design. Randomised controlled trial studies of therapy or prospective cohort studies of assessment and natural history, meeting specific criteria, are internationally recognised as acceptable evidence.
Evidence for some treatment options such as biofeedback is unlikely to become available in view of their cost and limited application to the management of acute low back pain. Acceptable evidence may become available for some other treatment options and will be described in future editions of the guide.
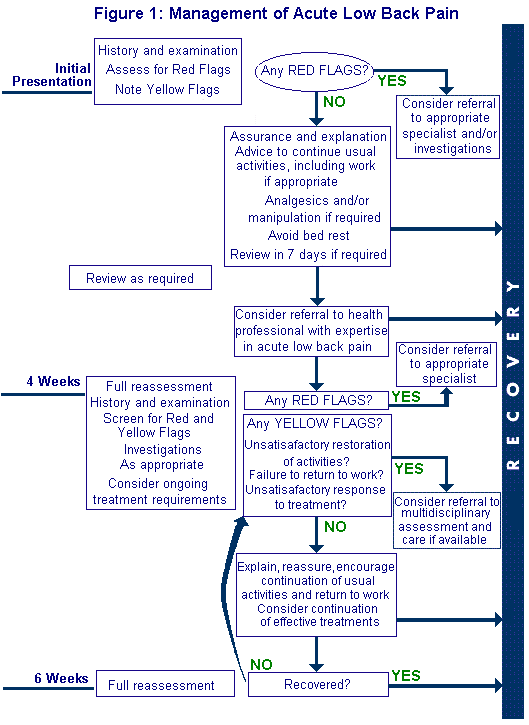
Best practice advice
The ‘best practice’ advice given in the Management of Acute Low Back Pain Flowchart (Figure above) and in the Summary of Management Options is not intended to be read as a rigid prescription. The advice is intended to offer flexibility and choice, so that clinical judgement can be made according to patients’ circumstances, supported by the best available evidence for improved clinical outcome.
Definitions
- Acute low back problems: activity intolerance due to lower back or back and leg symptoms lasting less than 3 months
- Chronic low back problems: activity intolerance due to lower back or back and leg symptoms lasting more than 3 months
- Recurrent low back problems: episodes of acute low back problems lasting less than 3 months but which recur after an interval free of low back symptoms sufficient to restrict activity or function
Most severe back pain and severe activity limitation improves considerably in a few days or at most a few weeks, but milder symptoms may persist longer, often for a few months.
A good history history must be taken to identify:
- the risk factors for serious disease (Red Flags, see next page)
- how limiting the symptoms are
- similar previous episodes
- any factors that might limit an early return to usual activities, including work (this includes screening for Yellow Flags - see page 7 and accompanying booklet)
The clinical examination aims to identify any neurological deficit (note that over 90% of all clinically significant lower limb radiculopathy due to disc herniation involves the L5 or S1 nerve root at the L4/5 or L5/S1 disc level). Pointers in the history may indicate the need for a more general examination, particularly if Red Flags for serious or systemic disease (such as cancer) are suspected.
The following approach to investigations and referral is recommended:
- Patients with persistent neurological deficit and pain should be referred to the appropriate specialist.
- Patients with Red Flags should be investigated appropriately and referred if investigations are abnormal. Referral may still be appropriate at 4 weeks, even if investigations are normal.
- Patients with no Red Flags and normal neurological examination should only have full blood count, ESR and plain X-rays of the lumbar spine if they have not recovered at 4 - 6 weeks or if there are other indications.
- Abnormal investigations may justify referral to an appropriate specialist.
- At 6 weeks, patients with no Red Flags, normal investigations and persistent symptoms should be referred to a specialist or specialist team if available. Multidisciplinary Teams may be more effective in preventing pain and disability.
Intervention between 4 and 8 weeks after acute low back problems start is most likely to help prevent chronic low back problems. Patients with low back symptoms persisting beyond 12 weeks have a rapidly reducing rate of return to normal activity.
| Table 1: Red Flags for potentially serious conditions |
|
| Note: Yellow Flags It may be useful to conduct a preliminary screening for important psychosocial factors (Yellow Flags) at the time of initial presentation. Potential Yellow Flags should be more comprehensively and formally assessed at the 4 and 6 week full reassessments, if the patient is not making expected progress. Refer to page 7 and the booklet, ‘Guide to Assessing Psychosocial Yellow Flags in Acute Low Back Pain’. |
A full blood count and ESR should be performed only if there are any Red Flags. Other tests may be indicated depending on the clinical situation.
Plain X-rays of the lumbar spine are indicated if any of the Red Flags are present but not otherwise in the first 4 weeks. The value of plain X-rays to some treatment providers in developing a management plan must be balanced against the radiation exposures involved.
As 30% of people without low back symptoms will have significant abnormalities on MRI and CT scans of the lumbar spine, these investigations should be reserved for people being worked up for surgery or where a specific pathology (such as cancer or infection) is strongly suspected.
It is important to let the patient know that, if a full history and examination have uncovered no suggestion of serious problems, no further investigations are needed. They should be advised to stay as active as possible and continue usual daily activities.
Activity Alteration and Work Activities
Bed rest for more than 2 days should be discouraged, as it has been shown to impair recovery. It is recommended that patients should increase physical activity progressively according to a timetable rather than be guided by pain level. Activities and postures may need to be modified in the short term, and suitable advice provided.
It is important to discuss work activities, especially those involving heavy lifting, bending or twisting, that may have contributed to the original problems. Alternative duties and/or workplace design may need to be discussed with the worker and/or employer.
Effective interventions to control symptoms of acute low back pain include:
- Analgesics
If patients need their pain symptoms controlled, paracetamol and non-steroidal anti-inflammatory drugs have been shown to be effective. - Manipulation
Manual loading of the spine using short or long leverage methods is safe and effective in the first 4-6 weeks of acute low back symptoms. Treatments to relieve low back pain that do not include an appropriate emphasis on return to usual activity may inadvertently encourage the patient to fear moving or using their back. It is important to combine symptom control with encouragement to promote activity, including returning to work.
Advice to continue ordinary activity usually results in more rapid symptomatic recovery from an acute episode, and leads to less chronic disability and less time off work when compared to ‘traditional’ medical treatment. Traditional medical treatment has inappropriately focused on analgesics only as required, advice to rest and ‘let pain be your guide’ for return to usual activity. All of these have been shown to delay recovery.
Progressive reactivation over a short period of days or a few weeks, combined with behavioural management of pain, makes little difference to the rate of initial recovery of pain and disability, but leads to less chronic disability and work loss.
Advice on a planned return to normal work within a short time may lead to shorter periods of work loss and less time off work.
Educating patients about low back symptoms provides assurance. This can lead to improved feelings of well-being, reduced health service use and improved use of self-management strategies. Education as part of a ‘back school’ at the workplace may be effective. The efficacy of back schools in non-occupational settings has yet to be demonstrated by randomised controlled trials.
The clinician is responsible for making sure that the episode resolves as expected. Follow-up will depend on the clinical situation, including the severity of symptoms, the presence of any neurological deficit, history of previous episodes and other medical and/or psychosocial factors. A reasonable approach for most patients is a review by the end of the first week, unless symptoms have completely resolved. It may be appropriate to arrange an earlier review, to reinforce the message to keep active and avoid prolonged bed rest.
Yellow Flags and Red Flags can be thought of as:
- Yellow Flags = psychosocial risk factors
- Red Flags = physical risk factors
Yellow Flags are factors that may increase the risk of developing, or perpetuating, long-term disability and work loss associated with low back pain. Identification of risk factors can inform appropriate cognitive and behavioural management strategies to achieve functional outcome goals.
The accompanying Guide to Assessing Psychosocial Yellow Flags in Acute Low Back Pain provides:
- a method of screening for psychosocial factors that are likely to increase the risk of an individual with acute back pain developing prolonged pain and disability causing work loss and associated loss of quality of life
- a systematic approach to assessing psychosocial factors, including a screening questionnaire
- suggested strategies for better management by primary care treatment providers for those with acute back pain who are At Risk
The presence of psychosocial risk factors does not mean that the back pain is any less real nor does it reduce the need for symptom control.
Most At Risk individuals can be effectively managed by their usual treatment provider, without the need for referral to a psychologist. These patients will require strategies that are effectively integrated with requirements for analgesia and physical modalities to enable them to remain active and return to ordinary activities.
| Tabl2 2: Psychosocial Yellow Flags - main categories |
| Clinical assessment of Yellow Flags may identify the risk of long-term disability, distress and work loss due to: |
|
All patients with symptoms and/or signs of cauda equina syndrome should be referred urgently to an appropriate specialist. The presence of Red Flags and/or abnormal tests indicates the need to consider referral or at least fuller investigation. Certain Red Flags (such as severe pain at night or weight loss) should lead to full investigation and/or referral being considered, even if the tests are normal.
Patients with pain radiating from the back down one leg as far as the ankle, with or without neurological signs, have a higher chance of a disc herniation as the cause of their low back problems. Nevertheless, the natural history of back-related leg pain is benign in most patients and these patients should be managed as shown in Figure 1 unless there is unremitting, severe pain or increasing neurological deficit. Caution should be exercised in advising manipulation if there is any neurological deficit.
Surgery is not indicated for non-specific low back pain. Where there is no improvement, some patients with back-related leg pain and a defined disc lesion may recover more rapidly with surgery. Note that the long-term results of surgery for back-related leg pain are no better than conservative management. Patient preferences will be important in any decision about surgical intervention.
Most patients with episodes of acute low back pain should have largely recovered within 4 weeks. Some studies suggest that as many as 90% of affected people will have resumed their normal activities in this time. All patients who have not regained usual activity after 4 weeks should be formally reassessed and again at 6 weeks. The assessment should include retaking the history and examination, looking for Red or Yellow Flags, neurological deficit and any evidence of systemic disease. Treatment providers must consider whether continuing treatment will accelerate recovery or simply prolong the ‘traditional’ medical model.
Comment on Multidisciplinary Teams
There is clear evidence that Multidisciplinary Teams or networks are effective in managing chronic back pain. The evidence for their effectiveness in unresolved episodes of acute low back pain is yet to be determined. The expert panel has recommended the use of Multidisciplinary Team management for episodes of acute low back pain unresolved at 6 weeks in line with international opinion.
Who Might be in the Multidisciplinary Teams?
They might include health professionals with appropriate training in musculoskeletal disorders, psychosocial assessment, vocational management and other relevant specialities. These teams may not be embodied in a discrete organisation, but may reflect a close collaborative team approach for the assessment and comprehensive management of At Risk patients by professionals from various disciplines with specific skills working together. This is particularly true of rural areas where access to specialist teams would otherwise be a treatment barrier to those needing prompt specialist intervention.
What is the Role of Multidisciplinary Teams?
The lead treatment provider may require support from a multidisciplinary team to integrate all components of the comprehensive evaluation and management plan. This support could provide input into key clinical decisions and promote service coordination. Multidisciplinary Teams are able to:
- make an objective review of progress to date and a comprehensive evaluation of the presenting problem, emphasising the early identification of barriers to progress that have so far gone unnoticed.
- develop a comprehensive management
plan including:
- integration of all components of the evaluation into the decision-making process
- an outline of expected milestones with time frames
- incorporation of strategies for dealing with any barriers that are identified
- options for continued lack of progress.
- provide treatment, only for the most complex or resistant cases.
Table 3a and 3b provide a summary of management options based on the available evidence for improved clinical outcomes. The evidence was reviewed by an expert panel who felt that it was more helpful to focus on the availability of evidence rather than to make recommendations about the treatments that must or must not be used.
Caution should be exercised in recommending treatment options for which the evidence of improved clinical outcomes is lacking or inconclusive. Treatment providers who wish to provide best practice care can now choose treatments for which there is good evidence for improved clinical outcomes.
| Table 3a. Summary of management options for an episode of acute low back pain based on the evidence available at present |
| At least moderate research evidence for improvement in clinical outcomes |
|
| At least moderate research evidence for improvement in clinical outcomes |
|
| At least moderate research evidence of potential harm from the treatments below which should not be used for an episode of acute low back pain |
|
| Table 3b. Insufficient research evidence for any improvement in clinical outcomes |
|