

What Are Patient Beliefs and Perceptions About Exercise
for Nonspecific Chronic Low Back Pain?
A Systematic Review of Qualitative StudiesThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: Clin J Pain. 2014 (Nov); 30 (11): 995–1005 ~ FULL TEXT
Susan C. Slade, PhD, PT, Shilpa Patel, PhD, C. Psychol, Martin Underwood, MD, FRCGP, and Jennifer L. Keating, PhD, PT
Faculty of Medicine,
Nursing and Health Sciences,
Monash University,
Melbourne, Australia
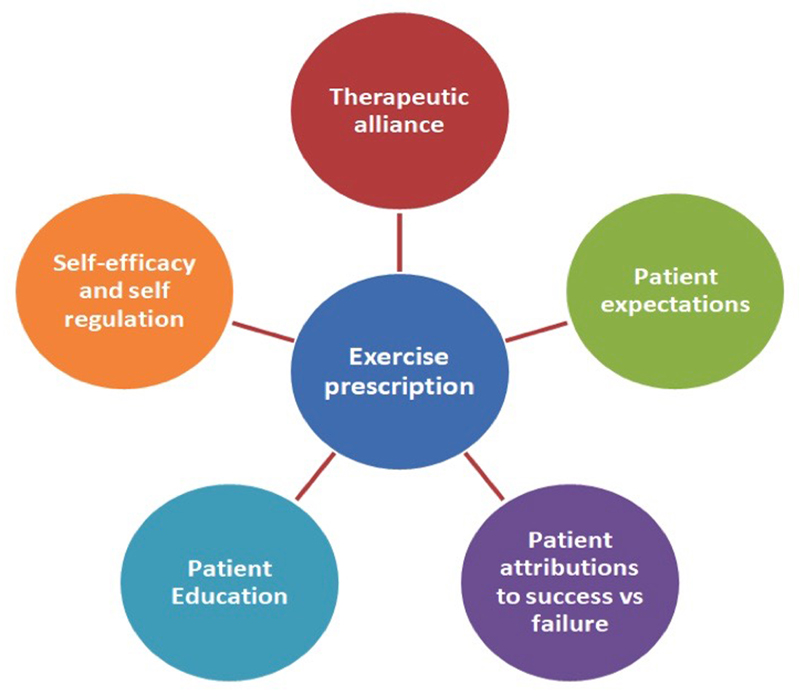
OBJECTIVES: The global burden of low back pain is the highest ranked condition contributing to years of living with disability. Exercise is moderately effective, and adherence to exercise may improve if participants are engaged. Identification of elements that enhance engagement would enable clinicians to prescribe appropriate interventions. The review objective was to identify and synthesize qualitative empirical studies that have explored beliefs about exercise therapy of people with nonspecific chronic low back pain.
METHODS: Two independent reviewers conducted a structured review and metasynthesis informed by Cochrane and Campbell Collaboration guidelines and the PRISMA statement. Fifteen papers were included for data extraction, method quality assessment, and thematic analysis.
RESULTS: Four key themes emerged: (1) perceptions and classification of exercise; (2) role and impact of the health professional; (3) exercise and activity enablers/facilitators; (4) exercise and activity barriers. Participants believed that there were distinctions between general activity, real/fitness exercise, and medical exercise. Levels of acquired skills and capability and participant experience with exercise culture require consideration in program design. People participating in exercise classes and group work may be more comfortable when matched for abilities and experience. When an intervention interferes with everyday life and appears to be ineffective or too difficult to implement, people make a reasoned decision to discontinue.
DISCUSSION: People are likely to prefer and participate in exercise or training programs and activities that are designed with consideration of their preferences, circumstances, fitness levels, and exercise experiences.
Key Words: exercise prescription, chronic low back pain, patient beliefs, qualitative research, review
From the FULL TEXT Article:
Introduction
The global burden of low back pain (LBP) is now the highest ranked condition contributing to years of living with disability. [1] It is an important source of long-term disability and absence from work and causes substantial economic and societal burden. Nonspecific chronic LBP (NSCLBP) is not a diagnosis but rather a description of back pain for which a cause cannot be definitively identified or a precise pathoanatomic diagnosis cannot be given. [2] Nearly all people with chronic LBP are diagnosed with NSCLBP; this does presume that specific pathologies have been ruled out after a clinical assessment that includes appropriate tests and imaging. [3–5] The condition manifests as a continuation of an initial episode or periodic recurrences and remissions. [6–11]
In addition to its specific effect on LBP, exercise is recommended for the prevention of many other diseases and for its general health benefitshttp://www.who.int/dietphysicalactivity/factsheet_recommendations/en/
World Health Organization and government recommendations focus on regular amounts of exercise to improve health, and more recent recommendations are for 1 hour of activity daily and moderately strenuous exercise for 30 minutes 6 d/wk
http://www.who.int/dietphysicalactivity/factsheet_recommendations/
http://www.health.gov.au/internet/.../health-pubhlth-strateg-phys-act-guidelines
http://www.gov.uk/government/publications/uk-physicalactivity-guidelines
http://www.cdc.gov/physicalactivity/everyone/guidelines/index.html
http://ec.europa.eu/sport/library/documents/c1/eu-physical-activity-guidelines-2008_en.pdfUnless contraindicated, people with back pain should be advised to exercise because of benefits to their general health.
Despite being recommended as the treatment of choice, exercise is at best only modestly effective for NSCLBP. In randomized controlled trials the effects of different types of exercise appear comparable. [12–30] Clinical practice guidelines for the management of NSCLBP recommend that patient preferences should be considered and that exercises should be individualized. [31] It is likely that adherence, as measured by attendance or engagement with exercise, and the extent to which a person’s behavior corresponds with agreed recommendations from a health care provider, will improve if programs align with participant preferences and beliefs.
Kolt et al [32] reported that participant adherence to low back rehabilitation increased with supplementary printed material, supervision, motivation strategies, clinic attendance, positive reenforcement, goal setting, and therapist/participant contracts. Supervised and individualized exercise with health professional input and self-management techniques including home audio and video-tapes have been demonstrated to have a positive effect on exercise adherence in chronic musculoskeletal conditions. [32–36] Self-efficacy, depression, pain catastrophizing, and levels of physical activity and ability have been demonstrated to have an impact on outcome in self-management programs for chronic pain. [37]
Jack et al [38] recommended that health providers who prescribe exercise also consider program organization and leadership skills, participant exercise history and level of ability, and education requirements that could dictate the format of explicit verbal instruction and written information. Identification of program design features that enhance engagement would enable clinicians to prescribe appropriate exercise and activity interventions for the NSCLBP care-seeking population. [39] By examining and analyzing the gap between what is offered and what participants expect, experience, and prefer, the exercise program content may be more attractive.
Participant reports are central to the evaluation of health care in terms of both outcomes and experience of the quality of care and can be used to identify areas that require action to improve the process and outcomes. [40] Varying approaches have been developed to elicit participants’ experiences of discrete aspects of health care and include interviews, focus groups, and surveys or questionnaires. [41] People with chronic disease and conditions, such as those with LBP, are often dependent on regular care and can often have well-defined knowledge of their own physical condition and ability. Consequently, many people may have specific expectations of the purpose and goals of management and may be able to provide insights into how and why they engage and participate. [42]
We conducted a systematic review of qualitative studies that have explored the perceptions and beliefs of people with NSCLBP with regard to exercise therapy, physical activity, or training for the management of their condition. Specifically, we sought to identify and synthesize qualitative empirical studies that explored what people with NSCLBP believe or perceive about exercise therapy, physical activity, or training for the management of their condition. We hoped that review outcomes might enable us to make recommendations for clinical practice and further research.
METHODS
A structured review process was adapted from the Cochrane Collaboration, Cochrane Back Review Group, PRISMA Statement, and Cochrane guidelines. [43–46] We used a comprehensive set of search strategies recommended for identifying qualitative reports. [47–52] The a priori inclusion and exclusion criteria were established before conducting searches of the electronic database and were applied to the final search yield. Two reviewers (S.P. and S.C.S.) used the criteria to screen titles and abstract. They independently extracted data, appraised method quality, conducted thematic analysis, and synthesized data in a narrative format. Two other independent researchers acted as arbiters throughout the process, gave expert opinion and assisted with consensus regarding methods, forms, and tables (J.L.K. and M.U.).
Inclusion and Exclusion Criteria
Papers were included if: they were published in peerreviewed journals; included >80% of participants over 18 years; participants consulted a practitioner who prescribed exercise; >80% of participants had back pain of >6 weeks duration; and papers reported data that enabled evaluation of what patients believe, prefer, or have experienced regarding exercise as a treatment for NSCLBP. Papers were excluded if they were not published in English or were editorials, expert opinion, letters, or commentary and when participants had NSCLBP with specific underlying spinal pathology. These criteria were applied to the search yield using a standardized form (online Appendix 1, Supplemental Digital Content 1, http://links.lww.com/CJP/A73) that was initially tested on 3 papers by 3 researchers (J.L.K., M.U., and S.C.S.) for consistency and agreement was unanimous.
Literature Search: Identification and Selection of Included Papers
Eight electronic databases were searched without date limits up until July 2012, using explosions and combinations of key search terms for qualitative research, exercise, physical fitness, physical training, conditioning, activity, LBP, patient experience, patient preference, attitudes, perceptions, expectations. Databases searched were AMED, Campbell Collaboration, CINAHL, Embase, Medline, PsychInfo, Sportdiscus, and ISI Web of Science. In addition, we did forward and backward citation tracking of included papers and selected review articles. Search language was adapted to individual database formats. Search strategies are available in online Appendix 2 (Supplemental Digital Content 2, http://links.lww.com/CJP/A74). All of the searches were downloaded to bibliographic management software for deletion of duplicates and initial screening of titles by the primary author who deleted those that were clearly irrelevant. Two independent researchers (S.C.S. and S.P.) screened the remaining abstracts and read papers in full before making final inclusion/exclusion decisions. Disagreements were resolved through discussion and a third reviewer was approached if consensus was not reached or when there was a conflict related to reviewer independence.
Data Extraction
Data extraction guidelines and a data extraction form (online Appendix 3, Supplemental Digital Content 3, http://links.lww.com/CJP/A75) were developed by consensus (S.C.S., S.P., J.L.K., and M.U.) so that the same information was extracted from each included paper. The following data were systematically extracted under the following headings: methods, population, data collection, data synthesis, results, themes, discussion, conclusions, and recommendations. The completed data extraction forms were examined for consistency and merged for the data synthesis phase. Themes and subthemes were extracted from each included paper, independently confirmed by the 2 researchers, and transferred to a spreadsheet. The items were assembled into common groups, and duplicates were deleted to remove ambiguity. Reviewers did not extract data from studies for which they were coauthors.
Method Quality Assessment
Two reviewers independently appraised included studies using the Critical Appraisal Skills Programme checklist for qualitative studies because it provided decision rules and detailed instructions on how to interpret criteria. [53] Reviewers were not involved in quality appraisal for studies on which they were coauthors. This checklist consists of a series of questions that helps the reviewer to assess the rigor, credibility, and relevance of the study. Rigor refers to whether the approach to the study is thorough and appropriate; credibility refers to whether the findings are well presented and meaningful; relevance refers to the usefulness of the study’s findings. [54–59] Disagreements were resolved by consensus and by a third researcher if necessary. Papers were not excluded on the basis of method quality but partitioned into high and low scores for outcome comparison in the discussion.
Data Analysis
The primary studies were combined, compared, and contrasted to generate meaning that extended beyond any individual study using interpretive synthesis, which is a combination of metaethnography and grounded theory. During data extraction, the themes and subthemes from each paper were extracted, and a thematic framework was developed for the entire data set. This involved reading all of the included papers in-depth, noting the major themes reported in all of the papers, and then developing a thematic framework that encompassed all identified themes. In this way the concepts from individual studies were “translated” into one another to become overarching themes. This framework was then applied to the extracted data and used to develop analytical charts to manage the data. [60] The data synthesis built interpretation from the original studies by firstly identifying interpretations offered by the original researchers (secondorder constructs) and, secondly, enabling the development of new interpretations (third-order constructs) that go beyond those offered in individual primary studies and offer a reinterpretation based on primary research.
Data management began with familiarization with the data and the noting of recurrent themes, constructing an index, and labeling the data with the index. The data were then sorted by theme and summarized in a series of matrix-based charts, retaining the context and language of the respondents. Descriptive analysis involved identifying dimensions within the data, categorizing these dimensions, and finally grouping sets of categories together as classes. Explanatory analysis involved identifying links between sections of and subgroups within the data to try to explore why such associations and subgroups existed. The reviewers independently developed overarching models that linked together the translations and authors’ interpretations. These models were then discussed, merged, and used to generate hypotheses to produce a “line-of-argument.”
Charting the data enabled us to compare how the same theme was explained and interpreted within different studies and whether there were recurring themes. Two independent researchers (S.C.S. and S.P.) conducted thematic analysis, consulted at stages during the process using the constant comparison method, and identified major overarching or higher-order themes. An approach was taken that primarily applied thematic analysis, which was considered within a grounded theory framework. We summarized the themes and subthemes from each paper and collapsed them into the overarching themes and summarized how the authors of each paper explained and interpreted common understandings. The richness of the data and thoroughness of explanatory analysis was deemed more important than the frequency of reported themes. It became apparent that the included studies shared a number of major themes; we were able to assess the frequency of these themes in comparison with the entire data set. [61-63]
RESULTS
Review Identification and Selection

Figure 1 The total search yield of 3,431 was sorted by title, and 3,311 clearly unsuitable titles were excluded. The remaining 121 titles were examined by title and abstract. Two independent reviewers (S.C.S. and S.P.) excluded 75 papers after applying the inclusion and exclusion criteria to the information contained in the abstract. Of the remaining 48 papers, 33 were excluded after reading in detail and applying the inclusion and exclusion criteria. The 2 authors (S.P. and S.C.S.) were able to reach a consensus without an independent arbiter. Figure 1 shows a flowchart of progress into the review with a total of 15 included papers (12 studies). [64–78]
Method Quality
The method quality was assessed, using the Critical Appraisal Skills Programme tool, by 2 independent researchers, and consensus was reached regarding a rating of low, medium, and high for each included paper (Table 1, Supplemental Digital Content 4, http://links.lww.com/CJP/ A79, Table 2, Supplemental Digital Content 5, http://links. lww.com/CJP/A80).Three studies (4 papers) were of high quality, [71, 73–76]
8 were of medium quality, [65–67, 69, 70, 72, 77, 78]
and 1 was of low quality. [68]Interobserver agreement of quality assessment was determined by calculating percentage agreement and a k-coefficient. There were a total of 120 items (10 items for each of the 12 papers), and the reviewers agreed on 103 items (85%) and disagreed on 17 items (15%). The overall interobserver agreement of the individual items (k=0.077) represents substantial agreement between the reviewers. For the initial total method quality score the 2 reviewers agreed on 8/12 scores. Following a consensus and discussion round agreement was reached on 12/12 scores without the need for an independent arbiter.
Data Extraction
Pilot data extraction for 2 papers conducted by S.C.S. and S.P. in November 2012 indicated there was consistency and unanimous agreement. [68, 78] Extracted data were merged and synthesized from individual documents into a summary table (Table 3, Supplemental Digital Content 6, http://links. lww.com/CJP/A81). The included studies provide data from studies conducted mostly in the United Kingdom and 1 each from Australia and New Zealand; there were no data published for other cultural contexts.
Data Synthesis
After reading all the papers in-depth and noting the major themes, it was agreed that the thematic framework should be participant beliefs about exercise and activity for NSCLBP.
Four key themes emerged:(1) perceptions and classification of exercise;
(2) role and impact of the health professional;
(3) exercise and activity enablers/facilitators;
(4) exercise and activity barriers.A table of all supporting extracted quotes is available from the first author on request.
Theme 1: Perceptions and Classification of Exercise
Perceived Difference Between Medically and Nonmedically Prescribed Exercise:
Most participants acknowledged the importance of being active but made a distinction between general activity, real/fitness exercise, and medical exercise. Many participants were not challenged by traditional back exercise programs and perceived these as unlikely to be helpful. Those who had extensive exercise experience appeared less fearful, and more confident, about exercise effects and various exercise environments. Some people had pursued their own exercise programs or developed relationships with trainers, often by “trial and error,” because they felt that physiotherapy and rehabilitation classes did not push them hard enough. [65–68, 71, 72, 75–77]
David (FG3): “the best thing that I can do is just walk, even if it’s sore, I still think I’m better to keep walking.” [71] (p1906)
“I’ve been doing the Pilates and the walking has vastly improved my condition. I’m cycling 10–15 minutes and then I swim for half an hour, but I try to do that 5 days a week.” [68] (p1481)
Participant 21, 39–year-old woman: “I think you should be made to do more. It wasn’t working me hard enough. I think you need much more as you go on.” [66] (p24)
A26-13-2038: “I am already a physically active person and the study did not take this into account.” [77] (p754)
Carolyn: “when you’re working with a physiotherapist you feel like you’re in a clinical situation. With a personal trainer you feel like you’re in a motivational situation, it’s more encouraging.” [75] (p117)
Participant 1, 39–year-old man: “I think physiotherapists give you a type of exercise, which is very specific to the back problem. These are the types of exercises that you would do on your living room floor; people haven’t got the motivation to do this on a daily basisy” [66] (p247)
“To me at a sports centre you’re exerting yourself.” [65] (p66)
Individual Preferences for Types and Formats of Exercise:
There are individual preferences such as consideration of experience, abilities, adequate physical challenge, exercise mastery, individualization, and supervision and a belief that spinal stabilization is beneficial. Matching people with similar fitness, strength, and technical expertise was thought important for enhancing group dynamics. Individual performance could be enhanced when exercises were aligned with fitness levels and previously acquired skills. [64–67, 70–72, 75, 77, 78]
Participation and engagement were facilitated by familiarity with the exercise environment, culture and training process, and knowledge acquired from previous exercise programs. Individuals were more likely to engage within programs that were fun and had variety than ones that were boring, unchallenging, or onerous because they disrupted daily activities.
G2:F40: “If you stabilise the muscles around your spine then the spine will get more chance of staying healthy. [76] (p182)
Michael: “Going to the gym is about physically going to a safe place. I can do exercises there if I go to the gym. I can use the equipment. I’m here; I’ll do those things.” [75] (p117)
Participant 21, 39–year-old woman: “It wasn’t working me hard enough. I think it could have been more. It does work, but I think you need much more as you go on. Like each time you should get more and more.” [66] (p247)
Jean: “I’m not a gym person. If you’re taking people who have never done exercise into an environment that is so powerful, you’re intimidating them from the word go.” [75] (p117)
A55-18-2004: “I am surprised that no one has asked what forms of exercise I take, particularly as most of the exercises I do at the class, I have already been doing myself.” [44] (p754)
130-13-2001: “I find back pain improves with regular exercise at local gym. If attending three times a week, back pain eases.” [77] (p754)
Deborah: “I loathe exercise. I don’t like structured exercise”. Surely there must be a fun way of doing it. I was offered three free dancing lessonsyanother creative way of getting exercise. It’s exercise without exercising.” [75] (p118)
693-17-2000: “I feel that the exercise class is geared to people who do no exercise. As I exercise every day I find it a waste of time getting to and from the class.” [77] (p754)
“You can go at your own pace, and your own capabilities. Nobody made you feel embarrassed or anything.” [65] (p65)
Importance of Individualized Exercise:
Participants liked or wanted exercises, and the delivery of exercise programs, to be individualized. Participants who felt that their exercises made sense to them and were well explained also felt that their individual needs were addressed, in contrast to those who felt that their exercises did not make sense or did not push them hard enough. Compliance was difficult when they lacked confidence in correct exercise performance and there was consensus that a sense of mastery is essential for correct exercise technique and confidence building. People wanted exercise instructors to demonstrate exercises, observe exercise practice, give feedback, and make subsequent corrections in technique. This concurs with the NICE clinical practice guidelines that exercise for NSCLBP should be individualized or tailored to the person and supervised. [64–67, 70–72, 75, 77, 78]
Irene (FG2): “I went to a back classyphysio, and there was about eight or nine people in the class, but it didn’t work because what suited one person didn’t suit another.” [71] (p1903)
Rita: “If they demonstrate it on your body you tend to remember. It does help your image in your mind later on.” [75] (p118)
Jean: “The important thing about being monitored is they are giving you feedback. So, one-to-one is ideal, one-to-four is reasonable as long as the person is there.” [75] (p118)
Participant 9, 62–year-old woman: “I think I would have liked maybe a little more time doing exercises with them. Because it is very rushed in there it’s a very busy unit, and maybe a little more time, maybe 10 minutes, 15 minutes of actually doing the exercises with them.” [66] (p249)
Female patient, age 46, nurse: “I think the exercises are fine and when I asked how to do them they were further explained to me. And it seems the exercises make you clear how to do things automatically, as you would do things in daily life.” [64] (p70)
R14 (female, age 52): “It was great to be supervised. I was worried about doing the wrong thing, so to be told why you’re doing thisyyou had confidence that it was okayythe fact that someone was watching gave you confidence.” [70] (p43)
Theme 2: Role and Impact of the Health Professional
People perceive that the health professional has a definite role and preferred characteristics that include good communication and being an effective educator. [64, 66, 72–76, 78]
Effective and Good Health Care Provider Communication Skills Are Important:
Good communication was related to participants feeling involved in the process. Participants who were not able to discuss their needs or who received poor explanations did not feel involved. According to participants, good health professional communication involved taking time over explanations; using appropriate language and terminology; listening, understanding, and getting to know the patient; and encouraging the patient’s participation in the communication process. They particularly valued behaviors such as listening and responding to their questions, consulting with them about the effectiveness of the therapy and relating the intervention to their individual self-help needs. The key issue here is that the process was seen as consultative, rather than prescriptive and that the individual’s values, preferences, and life circumstances are considered.
Participant 4, 52–year-old woman: “Got boredythey didn’t ask me what I thought I wanted, they just did what they assumed was physiotherapy.”66(p248) G2:M46: “He has got very much the right attitude. He is encouraging you, explaining it to you clearly and encouraging you to go through with it.” G2:F40: “In addition to the video, his explanation of the rationale behind it must have some benefits and it clearly did.” [76] (p182)
Lynne, aged 47 years, who had a 10–year history of NSCLBP: “the people who were running the program would get angry with me (when I couldn’t do the exercise correctly) and so it didn’t actually help (I felt guilty for a long time).” [74] (p147)
Participant 0206, ATX24, EP: “You have to make the appointment to go and see the GP for him to do the prescription exercise. I thought he would go through the do’s and don’ts. What to start off with, what to work up to, how often, blah, blah, that sort of thingyI was in there and out within 3 minutes, he just sat and read the sheet of paper and that was it. He sent me away to work it out for myself. [75] (p202)
Participant 5, 48–year-old woman: “I know somebody else who went to a back class, and I don’t think they got quite so much in-depth explanation about it, and they just thought this exercises oh God, why do I have to do them? But when you got it really explained to you, and what the benefits, and to keep doing this.” [66] (p246)
Lynne: “With the personal trainer I learnt what I had to do in a non-hazardous, for me, way. It basically turned my life around. I don’t think I ever really knew what it was I had to do. He was an educator.” [73] (p276)
Provision of Education and Information Are Important:
Participants liked or wanted treatments and diagnoses that were well explained, and participants who received poor explanations did not feel involved. There was a strong emphasis on wanting an understanding and explanation of their situation, to be given education material and resources, and accurate, understandable explanations that are free from jargon.
Female patient, age 56, doctor’s receptionist: “They explained everything carefully and assured me I wouldn’t break anything.” [64] (p68)
Michael (FG1): “I think it’s (advice) crucialythe only thing I would say is that the advice is often given at a time when the patient is in pain and is least likely toyreflect on it maturely. So I think it could be helpful to be given both the advice when you are in pain and also the advice at a period afterwards, when you are probably better.” [71] (p1903)
Participant 2: “It also gave you a greater understanding of the actual physiology of the spine and how you can damage it so easily but how strong it is in another sense if you move properly and if your posture is right. I think that was very helpful.” [72] (p170)
Carolyn: “Heaps of explaining, telling you why you’re doing this particular exercise. I think just having things explained to you is very important. Tell me why, tell me why. Explain it to me.” [73] (p275)
G1:M56: “Mainly that (video) shows we should sort of know a little bit more about how the body works, so that we can be responsible to ourselves to a degree so that we do the right things like bending/not bending.” [76] (p182)
Theme 3: Exercise and Activity Enablers/Facilitators
Across the included studies participants identified additional enablers to exercise participation and engagement that included self-efficacy and self-confidence, perceived benefit, or good outcome, effective for pain reduction, motivators, and incentives. Confidence was gained by successful performance through supervision, pain control, knowledge acquisition through the provision of information, goal sharing, and follow-up contact.
Supervision of exercise programs was considered important to provide individual correction:
Participants expressed the need for follow-up support and reassurance from the practitioner that they were carrying out instructions correctly, and assistance with appropriate treatment progression in line with their stage of recovery. It was generally expressed that exercise instructors should demonstrate exercises, observe exercise practice, give feedback, and make subsequent corrections in technique rather than hand out a sheet or list of exercises. [64–67, 70, 71, 73–75, 77, 78]
Michael (FG1): “In my own case I think it (exercise) is very important. I would now exercise every day at least by walkingyI would also swim and occasionally I would do the exercises if I feel that my back’s beginning to tighten again, so I think it’s crucial.” [71] (p1903)
Participant 0401, ATX6 and EP: “I don’t think it will cure the pain but I think it will, hopefully, help to ease it. That’s what I’m hoping for. And at least make me, I’m hoping that, you know, if I’m doing things wrong it will correct it.” [78] (p200)
R16; female, age 52: “When I first started doing the exercises, I wasn’t confident enough to do it, because I was frightened that I was going to harm my back. After a while I got the confidence to know that I could do it and it wasn’t harming my back.” [70] (p43)
G1:M56: “I did find the exercise made it more comfortable and made me more flexible”; G2:F53: “I still get pain, but it is not tending to be of the same severity as it was before.” [76] (p182)
233-11-2019: “The exercise classes have got me in a very much improved mental state.” [77] (p754)
A71-18-2020: “I have found this (exercise routine) to be very beneficial, both physically and mentally.” [77] (p754)
Participant 14, 41–year-old man: “It would be helpful if there was somebody you could phone and say well, you know my background, this is how I’m feeling, is there some exercises I should be starting again, or is there something else I could try.” [67] (p45)
Theme 4: Exercise and Activity Barriers
Across the included studies participants identified barriers to exercise participation and engagement. These included lack of time, diagnostic uncertainty, fear of pain, and lack of fit into daily life.
Time:
Difficulties with exercise adherence and not seeing benefits of exercise were frequently attributed to lack of time and fit into daily life. Participants believed that being disciplined to prioritize exercise within routine daily life and family commitment was important for their ongoing participation. [67–69, 71, 72, 75, 76, 78]
Participant 0206: “Fit into your daily life? A nightmare! There is a cre`che at the gym but that is Ł3.75 an hour andyby the time my husband gets home in the evening; there isn’t any time to get to the gym.” [78] (p202)
Participant 12, 64–year-old man: “I only do them (exercises) one lot in the morning. Certainly they were saying three times a day, which I think is probably not easy for everybody to doyI used to find difficulties with doing them at work.” [67] (p45)
Alan, a patient: “Doing your exercises twice a day or whatever. Finding the time in the morning and find the time in the evening. That’s something I’m not yet managing to do regularly enough I think to really make the difference.” Harry, a patient: “There’re always a thousand things that need to be done and somehow doing exercisesytends to fall further and further down the list.” [69] (p629)
Participant 5: “If you keep the exercises up, which I don’t all the time because I haven’t got the time but I do when I can.” [72] (p170)
G2:F53: “To do them all (stabilisation exercises) you need to set the alarm and get up early in the morning, I mean it is something once you get into a habit of doing.” [76] (p183)
G2:F40: “And I try sort of bring into like my everyday life rather than do the whole exercises two or three times a week.”76(p183) Steven aged 60, with a 42–year history of NSCLBP: “They structured what they wanted me to do around my work and life.” [73] (p274)
Peter aged 43, with a 1–year history of NSCLBP: “Understanding you and your lifestyle, ask you questions about your life, what you do.” [73] (p274)
Alan: “Eventually I’ll get my act together and absorb it into my lifestyle but it’s not something I can do overnight.” [69] (p629)Diagnostic Uncertainty:
The need for an accurate diagnosis was typically considered to be an acceptable means of “validating” the individual’s distress, and contributing to improved treatment outcomes and a means of reducing the risk of doing the wrong exercises. Verbeek et al42 reported that patients expect an accurate diagnosis, so that they can prove to themselves and others that their pain is real. Patients are often dissatisfied either about not receiving a diagnosis, inadequate diagnoses, or different diagnoses over time. The inability of practitioners and exercise programs to relieve pain, for many people, was a source of much frustration and disappointment and could invoke perceptions of not being believed. The explanations patients had already been given for their LBP may have affected their beliefs regarding the level of exercise and activity they could manage. These experiences were felt to contribute to nonadherence to medical regimens and unsuccessful rehabilitation. The lack of a precise diagnosis is typically associated with poor recovery. Clinicians may need to reflect on the way they handle uncertainty of this nature and how this diagnostic uncertainty may influence treatment decisions and communication with care seekers. [65, 66, 71, 72, 75, 77]
Participant 22, 33–year-old woman: “I think by the middle or the end of my treatment I would have expected to know what was going on, what was wrong with my back. I think, if it’s curable or if it’s not. If it’s just going to be a long-term thing, I would like to have found out.” [66] (p248)
Jean: “I found out since that it’s not been diagnosed correctly. They’ve been giving me the wrong exercises for somebody with what I’ve got now. For 10 years I’ve been doing exercises according to this type of pain, when it’s been aggravating the other thing that was never diagnosed, it was always there but they never looked at it.” [74] (p150)
David (FG3): “There was a real element of the doctor, you know, stabbing at different treatments, you know? ‘Cause I was never properly diagnosed, you know, you try this, try exercises, physiotherapy, tablets, put you in traction then for a while). It was just, I mean, nobody’s ever, you know, if they can’t put their finger on what it isythen they can’t treat it.” [71] (p1903)
Participant 6: “But all they tell me is it’s probably wear and tear.” [72] (p169)
Participant 2: “I do suffer from a lot of what I’ve been told is soft tissue pain, which is the damage caused to all the tissues, I have got some spikes on the vertebrae on the X-ray, it shows up, I don’t know what they call them, but there is a problem there.” [72] (p169)
Participant 3, 50–year-old woman: “I think [I’d have liked] some more insight into the back pain, and really find out what’s going on, you know.” [66] (p248)
Roberta (FG2): “Yes it comes down to the point again, of diagnosis and specialist advice and treatment.” [71] (p1904)Fear of Movement and Pain Aggravation:
Fear Avoidance: Fear of pain aggravation and the avoidance of potentially painful activities were associated with decisions to exercise and could lead to avoidance or loss of confidence with exercise and activity. Fear of pain returning could also be an incentive to continue exercise when this strategy had been successful. Exercise confidence could be enhanced by health care providers who demonstrated how to do the exercises correctly and gave feedback on performance and how to pace. As exercise is unlikely to produce an immediate tangible benefit, such as pain relief, it is difficult for many patients, for whom pain relief is their primary concern, to recognize the value of exercise. [65, 68, 70, 72, 75–77]
R16 (female age 52): “When I first went, started doing the exercises, I wasn’t confident enough to do it, because I was frightened I was going to harm me back, and after a while I’d got the confidence to know that I could do it and I wasn’t harming me back.” [70] (p43)
“It was great because you felt you were being supervised, I was worried about doing the wrong thing, so to be told why you’re doing thisyyou had confidence that it was okayythe fact that a physiotherapist was actually there watching you, gave you confidence.” [70] (p43)
Participant 4: “It aggravates you to the point sometimes where you think, I’m not going to do that it really really hurts, and I know you’ve got to get beyond that stage but it’s easier to say thaty[than] actually do it.” [72] (p170)
G1:F29: “I wanted to play tennis and was afraid it was going to really hurt me”; G1:F38: “When we played tennis we felt we had a similar sort of fear avoidance thing going on.” [76] (p182)
A04-10-2007: “The exercise classes were pointless; they just caused me more pain and aggravated pelvic injury from two years ago, causing a lot of pain which doctors just don’t seem to want to know.” [77] (p754)
“I usually pace myself on what I do on a daily basis and I know what I can and can’t do. If I carry on working all the time, just continuously doing housework or bending down, doing the dusting and things, it comes and it won’t go. The back pain gets worse and worse until I actually stop. Then I have a rest and then I just have to leave it for next time.” [68] (p1482)
DISCUSSION
It is interesting that very few of the papers we located actually reported on participant beliefs about exercise as a treatment for NSCLBP and barriers and motivators to adherence. Within the included studies there was inconsistency in the provision of supporting quotes, and often the emphasis was on experience of pain and health care provider opinions rather than exercise beliefs or perceptions. In the area of exercise and LBP research, there is a paucity of qualitative data. This contrasts with 336 randomized controlled trials of exercise as a treatment for chronic LBP that are listed in the Cochrane Library.
Four of the studies we identified were secondary analyses nested within randomized controlled trials. [64, 76–78] Two papers reported a research question, [64, 75] and all papers reported research aims or objectives. The method quality was variable but the majority of studies (8/12) were in the fair/ medium range and had the following consistent deficits in method quality: justified and explicit description of recruitment, data collection, and analysis steps that would enable replication, consideration of the researcher/participant relationships, and researcher biases. Linking the discussion to the research aims, examination of strengths and limitations, and recommendations for research were variable. It would be difficult to replicate many of the studies and build on existing work, and consideration might now be given to mechanisms for improved reporting of qualitative studies.
Key themes within the identified studies included perceived effectiveness, exercise ability and preferences, clinician communication skills, individualized care, supervision and motivation, system inflexibility, fear of pain, and compatibility with daily life. In all the included studies people classified exercise into formal exercise, which was exercise that they undertook with the purpose of being active, medical exercise for specific rehabilitation, physical activity involved in everyday life, and competitive sports. These clear distinctions between different forms of exercise and physical activity may provide a framework for shaping recommendations to undertake more exercise or be more physically active. This may take the form of raising awareness of incidental exercise and the World Health Organization and NHMRC recommendations for physical activity in daily activities (http://www.who.int/dietphysicalactivity/factsheet_ recommendations/). Those who are more confident or physically advanced could be directed to more demanding programs in a preferred environment or format.
The decision whether or not to exercise was influenced by beliefs about who should take responsibility for the decision to exercise (the participant or the clinician), participant’s feelings of self-efficacy to exercise, and the role of fear of exercise or fear avoidance. Exercise is unlikely to produce an immediate tangible benefit, such as substantial pain relief, and may require sustained commitment. It may therefore be difficult for many patients, for whom pain relief is their primary concern, to recognize the value of exercise. If pain relief is a factor that is known to feature highly in treatment expectations, the use of treatment programs that promote the improvement of functional activities despite pain will consistently fall short of patient expectations. The practitioner’s core listening and interpretation skills may have as much of an influence on treatment outcomes as the technical aspects of treatment. Factors such as access to facilities and programs, time constraints, work and/or family responsibilities, and environmental structure may not be modifiable but exercises can be designed to accommodate these variables by using, for example, alternate forms of equipment, low-cost community programs, work or home-based facilities, email and telephone coaching, and periodic face-to-face follow-up.
The incorporation of exercise into daily activity and exercising in a nonclinical environment is perceived as helpful. Investing in routine exercise could help reinterpret LBP as part of everyday life. If LBP is placed within a nonmedical context and becomes part of everyday life then addressing it with exercise might not be perceived as very disruptive. Exercise becomes routine or habitual; it is no longer a treatment belonging to the health care domain.
CONCLUSIONS
Clinical practice guidelines recommend individualized exercise (tailored to the person) and consideration of patient preferences for NSCLBP. Participants reported a preference for supervised exercise over advice to exercise. People feel encouraged to continue exercising when they have regular contact with a health care professional and feel understood. Countering fear-avoidance beliefs, building confidence, and providing support were also important. Individual exercise experience, ability, and preference may influence interpretation of the message to stay active and necessitate clarification by good health care provider communication skills. Consideration may be given to the wellness rather than the sickness model of normalizing or demedicalizing the implementation of exercise programs and framing them in the context of participant preferences.
LIMITATIONS
Throughout the metastudy process, we remained aware of 2 important limitations. First, the process decontextualizes data, removing it from the context in which it was originally presented or reported. Our access to this original context was limited by the primary research report, which could omit contextual factors. Second, a metasynthesis of this nature does not analyze original data; the synthesis relies on the data reported by the primary researchers. Two included studies (4 papers) were conducted and reported by review authors (S.C.S., J.L.K. and M.U.). We have endeavored to reduce bias by using a priori inclusion/exclusion criteria, assigning data extraction and method quality assessments to those review authors not involved in the studies, and ensuring a range of supporting quotes from across the included studies. The inclusion of only English language publications may be considered a limitation; however, examination of the entire search yield revealed that there were no non-English titles from the searched databases.
Recommendations for Research
Research is recommended to test the effectiveness of patient input into their exercise, activity, and rehabilitation programs. Studies that do not involve an intervention but explore patients’ beliefs specifically toward exercise or comparing before and after exercise interventions are required to replicate and build on the findings of this review and explore additional cultural contexts. A decision-aid for exercise prescription is currently not available. A questionnaire that clinicians can use to determine participant exercise preferences and inform their practice of exercise prescription has been recommended by Slade et al. [39] This questionnaire requires testing of the effects of participant-preferred exercise programs on outcomes in NSCLBP in the clinical environment to determine its utility as a method of systematic evaluation of care-seeker needs and preferences related to exercise. [39]
Investigation of important and effective communication skills to determine explicit forms of communication that are helpful in conversations designed to encourage healthy behaviors or attitudes and activity participation are recommended. This may be done through identification of communication skills essential to best practice, investigation of methods to teach and assess these skills, and the measurement and efficacy of behavior change and communication training for health professionals.
Recommendations for Clinical Practice
Often assumptions are made that health care professionals inherently understand patients’ beliefs. This may lead to patients becoming stereotyped and generalizations being made about their behavior. Effective communication and listening skills enhance and facilitate the clinical encounter. It is appropriate for practitioners to consider factors that facilitate participant engagement and incorporate these into exercise program design and to identify and remove barriers to participation. This experiential knowledge of people who have experience of back pain and beliefs about exercise may be used to inform and engage potential exercise participants.
ACKNOWLEDGMENTS
The authors thank Laura Blackman, BMedSci, for her initial work on this topic.
References:
Murray CJ, Vos T, Lozano R, et al.
Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990-2010:
a systematic analysis for the Global Burden of Disease Study 2010
Lancet 2013 Dec 15;380(9859):2197–223.Cassidy JD, Cote P, Carroll LJ, et al.
Incidence and course of low back pain episodes in the general population.
Spine. 2005; 30:2817–2823Boos N, Lander PH.
Clinical efficacy of imaging modalities in the diagnosis of low-back disorders.
Eur Spine J. 1996;5:2–22.Chou R, Fu R, Carrino J, et al.
Imaging strategies for low back pain: a systematic review and meta-analysis.
Lancet. 2009;373: 463–472.Jarvik JG, Deyo RA.
Diagnostic evaluation of low back pain with emphasis on imaging.
Ann Intern Med. 2002;137:586–597.Henschke N, Maher CG, Refshauge KM et al.
Prognosis in Patients with Recent Onset Low Back Pain in Australian Primary Care:
Inception Cohort Study
British Medical Journal 2008 (Jul 7); 337: a171Hestbaeck L, Leboeuf-Yde C, Engberg M, et al.
The Course of Low Back Pain in a General Population.
Results From a 5-year Prospective Study
J Manipulative Physiol Ther. 2003 (May); 26 (4): 213–219Hestbaek L, Leboeuf-Yde C, Manniche C.
Low Back Pain: What Is The Long-term Course?
A Review of Studies of General Patient Populations
European Spine Journal 2003 (Apr); 12 (2): 149–165Hoy D, Brooks P, Blyth F, et al.
The epidemiology of low back pain.
Best Pract Res Clin Rheumatol. 2010;24:769–781.Pengel L, Herbert RD, Maher CG, et al.
Acute low back pain: systematic review of its prognosis.
BMJ. 2003;327:323–325.Tamcan O, Mannion AF, Eisenring C, et al.
The course of chronic and recurrent low back pain in the general population.
Pain. 2010;150:451–457.Bystrom MG, Rasmussen-Barr E, Grooten WJ.
Motor control exercises reduces pain and disability in chronic and recurrent low back pain: a meta-analysis.
Spine. 2013;38:E350–E358.Clare HA, Adams R, Maher CG.
A systematic review of efficacy of McKenzie therapy for spinal pain.
Aust J Physiother. 2004;50:209–216.Hayden JA, van Tulder MW, Malmivaara AV, et al.
Metaanalysis: exercise therapy for nonspecific low back pain.
Ann Intern Med. 2005;142:765–776.Hayden JA, van Tulder MW, Malmivaara AV, et al.
Exercise therapy for treatment of non-specific low back pain.
Cochrane Database Syst Rev. 2005.Hayden JA, van Tulder MW, Tomlinson G.
Systematic review: strategies for using exercise therapy to improve outcomes for chronic low back pain.
Ann Intern Med. 2005;1:776–785.Keller A, Hayden J, Bombardier C, et al.
Effect sizes of nonsurgical treatments of non-specific low back pain.
Eur Spine J. 2007;16:1776–1788.Kent P, Mojound HL, Petersen DHD.
Does targeting manual therapy and/or exercise improve patient outcomes in nonspecific low back pain: a systematic review.
BMC Med. 2010;8:22.Macedo LG, Maher CG, Latimer J, et al.
Motor control exercise for persistent nonspecific low back pain: a systematic review.
Phys Ther. 2009;89:9–25.Macedo LG, RJEM Smeets, Maher CG, et al.
Graded activity and graded exposure for persistent nonspecific low back pain: a systematic review.
Phys Ther. 2010;90:860–879.Machado LAC, De Souza MVS, Ferreira PH, et al.
The McKenzie method for low back pain: a systematic review of the literature with a meta-analysis approach.
Spine. 2006;31: E254–E262.Pereira LM, Obara K, Dias JM, et al.
Comparing the Pilates method with no exercise or lumbar stabilization for pain and functionality in patients with chronic low back pain: systematic review and meta-analysis.
Clin Rehabil. 2012;26:10–20.Richards MC, Ford JJ, Slater SL, et al.
The effectiveness of physiotherapy functional restoration for post-acute low back pain: a systematic review.
Man Ther. 2013;18:4–25.Slade SC, Keating JL.
Unloaded movement facilitation exercise compared to no exercise or alternative therapy on outcomes for people with non-specific chronic low back pain: a systematic review.
J Manipulative Physiol Ther. 2007;30:301–331.Slade SC, Keating JL.
Trunk strengthening exercises for chronic low back pain: a systematic review.
J Manipulative Physiol Ther. 2006;29:163–173.van der Giessen RN, Speksnijder CM, Helders PJ.
The effectiveness of graded activity in patients with non-specific low-back pain: a systematic review.
Disabil Rehabil. 2012;34: 1070–1076.van Tulder MW, Malmivaara A, Hayden J, et al.
Statistical significance versus clinical importance: trials on exercise therapy for chronic low back pain as example.
Spine. 2007; 32:1785–1790.van Tulder MW, Koes BW, Malmivaara A.
Outcome of noninvasive treatment modalities on back pain: an evidence-based review.
Eur Spine J. 2006;15:S64–S81.van Tulder MW, Malmivaara A, Esmail R, et al.
Exercise therapy for low back pain. Exercise therapy for low back pain.
Cochrane Database Syst Rev. 2005.Wells C, Kolt GS, Marshall P, et al.
Effectiveness of Pilates exercise in treating people with chronic low back pain: a systematic review of systematic reviews.
BMC Med ResMethodol. 2013;13:7.National Institute for Health and Clinical Excellence (NICE).
Low Back Pain: Early Management of Persistent Nonspecific Low Back Pain
London: National Institute for Health and Care Excellence; 2009.
[Report No.: Clinical guideline 88].Kolt GS, McEvoy JF.
Adherence to rehabilitation in patients with low back pain.
Man Ther. 2003;8:110–116.Jordan JL, Holden MA, Mason EEJ, et al.
Interventions to Improve Adherence to Exercise for Chronic Musculoskeletal Pain in Adults
Cochrane Database Syst Rev 2010 (Jan 20); 2010 (1): CD005956McLean SM, Burton M, Bradley L, et al.
Interventions for enhancing adherence with physiotherapy: a systematic review.
Man Ther. 2010;15:514–521.Hall AM, Ferreira PH, Maher CG, et al.
The influence of the therapist-patient relationship on treatment outcome in physical rehabilitation: a systematic review.
Phys Ther. 2010;90: 1099–1110.Carnes D, Homer KE, Miles CL, et al.
Effective delivery styles and content for self-management interventions for chronic musculoskeletal pain: a systematic literature review.
Clin J Pain. 2012;28:344–354.Miles CL, Pincus T, Carnes D, et al.
Can we identify how programmes aimed at promoting self-management in musculoskeletal pain work and who benefits? A systematic review of sub-group analysis within RCTs.
Eur J Pain. 2011;15: 775.e1–11.Jack K, McLean SM, Moffett JK, et al.
Barriers to treatment adherence in physiotherapy outpatient clinics: a systematic review.
Man Ther. 2010;15:220–228.Slade SC, Keating JL.
Effects of preferred-exercise prescription compared to usual exercise prescription on outcomes for people with non-specific low back pain: a randomized controlled trial.
BMC Musculoskelet Disord. 2009;10:14.Jenkinson C, Coulter A, Gyll R, et al.
Measuring the experiences of health care for patients with musculoskeletal disorders (MSD): development of the Picker MSD questionnaire.
Scand J Caring Sci. 2002;16:329–333.Greenhalgh J, Meadows K.
The effectiveness of the use of patient-based measures of health in routine practice for improving the process and outcomes of patient care: a literature review.
J Eval Clin Pract. 1999;5:401–416.Verbeek J, Sengers M, Riemens L, Haafkens J.
Patient Expectations of Treatment for Back Pain:
A Systematic Review of Qualitative and Quantitative Studies
Spine (Phila Pa 1976). 2004 (Oct 15); 29 (20): 2309–2318Alderson P, Green S, Higgins J.
Cochrane Reviewers’ Handbook 4.2.1 (Vol. Section 8:
The Cochrane Library, Issue 1.
Chichester, UK: John Wiley & Sons Ltd.; 2004.Furlan A, Pennick V, Bombadier C, et al.
Updated method guidelines for systematic reviews in the cochrane collaboration back review group.
Spine. 2009;34:1929–1941.Altman DG, Sculz KF, Moher D, et al.
The revised CONSORT statement for reporting randomized trials: explanation and elaboration.
Ann Intern Med. 2001;134:663–694.Moher D, Liberati A, Tetzlaff J, et al.
Preferred reporting items for systematic review and meta-analyses: the PRISMA statement.
BMJ. 2009;339:332–336.Evans D.
Database searches for qualitative research.
J Med Libr Assoc. 2002;90:290–293.Flemming K, Briggs M.
Electronic searching to locate qualitative research: evaluation of three strategies.
J Adv Nurs. 2007;57:95–100.McKibbon KA, Wilczynski NL, Haynes RB.
Developing optimal search strategies for retrieving qualitative studies in PsycINFO.
Eval Health Prof. 2006;29:440–454.PearsonM,MoxhamT, AshtonK.
Effectiveness of search strategies for qualitative research.
Eval Health Prof. 2011;34:297–308.Walters LA, Wilczynski NL, Haynes RB.
Developing optimal search strategies for retrieving clinically relevant qualitative studies in EMBASE.
Qual Health Res. 2006;16:162–168.Wilczynski NL, Marks S, Haynes RB.
Search strategies for identifying qualitative studies in CINAHL.
Qual Health Res. 2007;17:705–710.CASP.
Critical Skills Appraisal Programme: 10 Questions to Help YouMake Sense of Qualitative Research.
Public Health Resource Unit, England:
Milton Keynes Primary Care Trust; 2002.Newton BJ, Rothlingova Z, Gutteridge R, et al.
No room for reflexivity? Critical reflections following a systematic review of qualitative research.
J Health Psychol. 2012;17:866–885.Kitto SC, Chesters J, Grbich C.
Quality in qualitative research.
Med J Aust. 2008;188:243–246.Kuper A, Lingard L, Levinson W.
Critically appraising qualitative research.
BMJ. 2008;337:687–689.Kuper A, Reeves S, Levinson W.
An introduction to reading and appraising qualitative research.
BMJ. 2008;337:404–407.Mays N, Pope C.
Assessing quality in qualitative research.
BMJ. 2000;320:50–52.Miyata H, Kai I.
Reconsidering evaluation criteria for scientific adequacy of health care research: an integrative framework of quantitative and qualitative research.
Int J Qual Methods. 2009;8:64–75.Pope C, Ziebland S, Mays N.
Qualitative research in health care: analysing qualitative data.
BMJ. 2000;320:114–116.Tong A, Sainsbury P, Craig J.
Consolidated Criteria for Reporting Qualitative Research (COREQ): a 32-item checklist for interviews and focus groups.
Int J Qual Health Care. 2007;19: 349–357.Dixon-Woods M, Booth A, Sutton AJ.
Synthesizing qualitative research: a review of published reports.
Qual Res. 2007;7: 375–422.Sandelowski M, Barroso J, Voils CI.
Using qualitative metasummary to synthesize qualitative and quantitative descriptive findings.
Res Nurs Health. 2007;30:99–111.Buijis PC, Lambeek LC, Koppenrade V, et al.
Can workers with chronic back pain shift from pain elimination to function restore at work?
J Back Musculoskelet Rehabil. 2009;22: 65–73.Cook FM, Hassenkamp AM.
Active rehabilitation for chronic low back pain.
Physiotherapy. 2000;86:61–68.Cooper K, Smith BH, Hancock E.
Patient-centredness in physiotherapy from the perspective of the chronic low back pain patient.
Physiotherapy. 2008;94:244–252.Cooper K, Smith BH, Hancock E.
Patients’ perceptions of self-management of chronic low back pain: evidence for enhancing patient education and support.
Physiotherapy. 2009;95:43–50.Crowe M, Whitehead L, Jo Gagan M, et al.
Self-management and chronic low back pain: a qualitative study.
J Adv Nurs. 2010;66:1478–1486.Dean SG, Smith JA, Payne S, et al.
Managing time: an interpretive phenomenological analysis of patients’ and physiotherapists’ perceptions of adherence to therapeutic exercise for low back pain.
Disabil Rehabil. 2005;27:625–636.Keen S, Dowell ACV, Hurst K, et al.
Individuals with low back pain: how do they view physical activity?
Fam Pract. 1999;16:39–45.Liddle SD, Baxter GD, Gracey JH.
Chronic low back pain: patients’ experiences, opinions and expectations for clinical management.
Disabil Rehabil. 2007;29:1899–1909.Morris AL.
Patients’ perspectives on self-management following a back rehabilitation programme.
Musculoskelet Care. 2004;2:165–179.Slade SC, Molloy E, Keating JL.
“Listen to me. Tell me”: a qualitative study of partnership in care for people with non-specific chronic low back pain.
Clin Rehabil. 2009;23: 270–280.Slade SC, Molloy E, Keating JL.
Stigma experienced by people with non-specific chronic low back pain: a qualitative study.
Pain Med. 2009;10:143–154.Slade SC, Molloy E, Keating JL.
People with non-specific chronic low back pain who have participated in exercise programs have preferences about exercise: a qualitative study.
Aust J Physiother. 2009;55:115–121.Sokunbi O, Cross V, Watt P, et al.
Experiences of individuals with chronic low back pain during and after their participation in a spinal stabilisation exercise programme - a pilot qualitative study.
Man Ther. 2010;15:179–184.Underwood MR, Harding G, Klaber-Moffett J.
Patient perceptions of physical therapy within a trial for back pain treatment.
Rheumatology. 2006;45:751–756.Yardley L, Dennison L, Coker R, et al.
Patients’ views of receiving lessons in the Alexander Technique and an exercise prescription of managing back pain in the ATEAM trial.
Fam Pract. 2010;27:198–204.

Return to LOW BACK PAIN
Return to EXERCISE AND CHIROPRACTIC
Since 7-21-2018


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |