

Parent Reports of Exclusive Breastfeeding After Attending
a Combined Midwifery and Chiropractic Feeding Clinic in
the United Kingdom: A Cross-Sectional Service EvaluationThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: J Evid Based Complementary Altern Med. 2016 (Apr); 21 (2): 85–91 ~ FULL TEXT
OPEN ACCESS Joyce Miller, BS, DC, PhD, Monica Christine Beharie, MChiro, Alison M. Taylor, RM,
Elisabeth Berg Simmenes, MChiro, and Susan Way, PhD, RM
Anglo-European College of Chiropractic,
Bournemouth, UK
This service evaluation investigated an interdisciplinary allied professional health care strategy to address the problem of suboptimal breastfeeding. A clinic of midwives and chiropractors was developed in a university-affiliated clinic in the United Kingdom to care for suboptimal feeding through a multidisciplinary approach. No studies have previously investigated the effect of such an approach. The aim was to assess any impact to the breastfeeding dyad and maternal satisfaction after attending the multidisciplinary clinic through a service evaluation. Eighty-five initial questionnaires were completed and 72 (85%) follow-up questionnaires were returned. On follow-up, 93% of mothers reported an improvement in feeding as well as satisfaction with the care provided. Prior to treatment, 26% of the infants were exclusively breastfed. At the follow-up survey, 86% of mothers reported exclusive breastfeeding. The relative risk ratio for exclusive breastfeeding after attending the multidisciplinary clinic was 3.6 (95% confidence interval = 2.4–5.4).
KEYWORDS: children; complementary and alternative medicine
From the FULL TEXT Article:
Introduction
Suboptimal breastfeeding is a recognized problem among mothers and health care professionals worldwide. According to government statistics, 81% of UK mothers initiate breastfeeding, 46% exclusively breastfeed at 1 week declining to 23% at 6 weeks. [1] Despite the high initiation rate, only 1% of mothers exclusively breastfeed for the recommended length of 6 months, [1] and the United Kingdom remains one of the countries in the world with the lowest rates of exclusive breastfeeding. [2, 3]
The World Health Organisation, [4] UNICEF, [5] and government policy in the United Kingdom [1] recommend exclusive breast milk until the age of 6 months. Extensive evidence has underlined several health benefits from exclusive breastfeeding including reduced risks for common childhood illnesses along with childhood leukemia and sudden infant death, [6] as well as reduced obesity, type 1 and 2 diabetes, and improved psychological health and emotional bonding. [6–8] In addition to health advantages, breastfeeding can be valuable financially and emotionally to the individual family as well as cost-effective to society. [9, 10] Simply supporting women who breastfeed at 1 week to continue to 4 months could result in the National Health Service saving Ł11 million (US $19 million) annually. [11] More than Ł3.6 million ($5 million) could be saved in treatment cost of gastrointestinal infection, Ł6.7 million ($10 million) for respiratory tract infection, and Ł6 million ($9.3 million) for necrotizing enterocolitis and Ł750 000 ($1 million) for acute otitis media. In total, over Ł17 million ($26 million) could be saved annually by reducing just these 4 infant diseases. [12] Doubling the number of breastfeeding mothers could also reduce the incidence of breast cancer, saving Ł31 million ($47 million) annually and Ł959 million ($1.4 billion) in 2010 lifetime costs. [12]
Despite the benefits of breastfeeding and the risks of artificial feeding, there is little evidence for interventional strategies that change the trajectory toward suboptimal breastfeeding levels in the modern Western world in conjunction with assessing maternal satisfaction of the interventional experience. One in every 4 women in the United Kingdom is critical of their routine postnatal care and feeding support. [13] Ninety percent of mothers who quit breastfeeding stated they would like to have continued but did not have sufficient support. [1, 14]
However, a variety of interventions have aimed to support breastfeeding mothers and enhance the rate of successful breastfeeding. Evidence suggests that advice, guidance, early skin to skin contact, and unrestricted feeding may assist mothers to overcome breastfeeding obstacles. [14–16] A 2012 study investigated the impact of additional breastfeeding support, compared with usual maternity care. The results demonstrated that all forms of extra support by both lay and professionals had some positive impact on breastfeeding outcomes; however, maternal satisfaction was poorly reported. [17]
Satisfaction has been described as the fulfilment of expectations, needs, or desires. [18] A few studies of maternal satisfaction have been identified. At a breastfeeding clinic in Quebec, 80% of 86 women reported being satisfied or highly satisfied with the clinic’s staff and care and agreed that it had enhanced their breastfeeding experience. [19] However, they did not measure or report any influence on long-term breastfeeding rates. At a Saskatchewan clinic, all of 43 respondents were satisfied with care and felt that the support they received helped them breastfeed. [20] However, the sample size was small and they did not demonstrate long-term breastfeeding rates.
There is modest evidence that manual therapy can be useful in solving the infant’s biomechanical problems that affect breastfeeding. [21–23] Midwives as well play a key role in achieving exclusive breastfeeding through their information and support to ensure effective positioning of the baby and attachment to the breast. [24] Midwives utilize the UNICEF UK Baby Friendly Initiative to support effective positioning and attachment. [5]
Both midwifery and chiropractic support were available separately to mothers prior to the development of the interdisciplinary clinic. As the process of suboptimal feeding is complex, combining professions could add value in addressing these problems. Evidence is lacking on this type of collaborative effort for suboptimal feeding; however, research has shown that there is a need for cooperation between health professionals to manage feeding difficulties efficiently. [21]
The purpose of this investigation was to evaluate maternal perception and satisfaction, along with long-term rates of exclusive breastfeeding with a service evaluation during and after attendance at a chiropractic and midwifery multidisciplinary feeding clinic on the south coast of England.
Methods
This was a cross-sectional evaluation of service provided at a chiropractic teaching clinic incorporating the complementary profession of chiropractic and the allied profession of midwifery in the same setting during the time frame from February 2013 to October 2013. A service evaluation was considered appropriate as there was minimal research from other settings that both types of interventions showed some efficacy, [21–24] but there was no evidence for provision of using a dual service indicative of a need for a service evaluation. [25] This would inform any future large-scale study. This service evaluation was developed as an early step in research to address the question whether the unified approach of chiropractic and midwifery clinical care was a useful way forward to tackle the public health problem of suboptimal breastfeeding.
Questionnaires were developed as a pilot project by experienced researchers as there were no previously validated instruments for this purpose. Data collected were sociodemographic characteristics (maternal and infant ages, ethnic origin, type of birth) and graded responses to the clinical experience provided. Sampling was by convenience, and all mothers who presented to the clinic with an infant feeding complaint and could read and write English were included. All mothers entering the clinic signed a consent form for inclusion and were informed that their inclusion was voluntary and all information was confidential. They also consented to a postal questionnaire by writing their own name and address on an envelope, which was then sent approximately 6 to 12 weeks later to assess feeding practices timed to arrive (with a date in the corner) prior to predicted weaning age and to investigate feeding practices after common ages of cessation. Exclusive breastfeeding or not was considered a long-term outcome if occurring from 7 weeks of age, as less than one fourth of mothers in the United Kingdom exclusively breastfeed at 6 weeks1 and other very large studies show that exclusive breastfeeding is exceedingly rare after that age. [26] The clinical experience included an obstetric-specific history taken by the midwife including delineation of breastfeeding difficulties. The midwives provided guidance and demonstration of correct holding and attachment recommended by UNICEF Baby Friendly Guidelines. The chiropractor provided a service that included a physical examination of the infant for biomechanical fault that could be related to suboptimal feeding and gave treatment with consent, where indicated. The infant’s suck technique was evaluated for rate, rhythm, suck-swallow-respiration cycle, masticatory muscle strength and tone, position of mandible, hyoid, general symmetry, and feeding efficiency, along with nociceptive input to mother.
Descriptive data analysis was performed using Microsoft Excel and SPSS. Change was determined by the report of the mother because mothers have been shown to be excellent historians for their infant’s behaviors. [22] All data were held in complete confidentiality, and all reports were anonymous and untraceable to any specific mother or infant. A university ethics committee determined that these surveys were considered evaluations of a service provided and all ethical standards were met.
Results
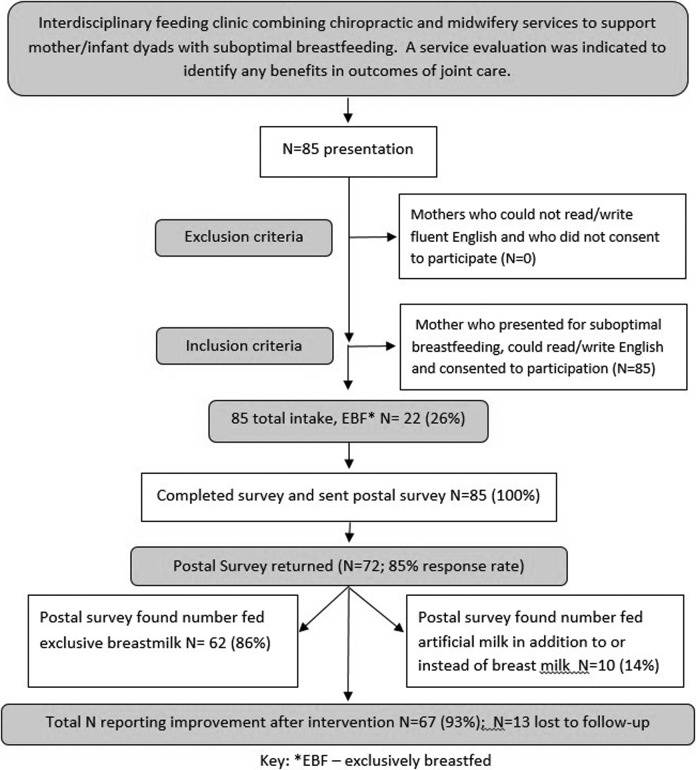
Figure 1

Table 1 During the time of the service evaluation, 85 mother-infant dyads entered the clinic. All 85 of the mothers were eligible for the study and completed the first questionnaire and agreed to receive a postal questionnaire. Follow-up surveys were sent 6 to 12 weeks after attendance at the clinic (to arrive at predicted time of weaning). There was a wide timeline in which the postal questionnaires were returned. Seventy-two mothers (85% response rate) returned the postal questionnaire. Figure 1 shows the flow of mother-infant dyads through the study.
Table 1 presents the demographic characteristics of mothers and babies attending the feeding clinic. When the first questionnaire was completed, 60% (n = 51) infants were 4 weeks of age or less. At the time of the follow-up questionnaire, 69% (n = 50) were 12 weeks and above. The median age of the mothers was 34 years. A full 96% (n = 81) were of white ethnic origin. Out of 85 infants, 48 (56%) had experienced an assisted birth.
The mothers could give more than one reason for attending the clinic. Eighty percent (n = 68) stated feeding-related problems, 42% (n = 36) had painful nipples, 39% (n = 33) reported having an unsettled baby, 39% (n = 33) had pain during feeding, 24% (n = 20) presented with birth-related difficulties, 25% (n = 21) for weight loss, 9% (n = 8) attended due to their health, and 11% (n = 9) had other reasons for attending the clinic.

Table 2 Maternal perception of the clinic is demonstrated in Table 2. At the first questionnaire after the clinical encounter, 100% (n = 85) of mothers agreed that they had understood the information given by the midwife. All the mothers understood the treatment done by the chiropractor (N = 80; 5 of the infants demonstrated no biomechanical fault and did not require chiropractic care). In all, 98% (n = 83) agreed that the clinic was well organized, planned to continue breastfeeding their baby, and would recommend the clinic to friends.
Several weeks later at the follow-up questionnaire, 93% (n = 67) reported improvement in infant feeding. Seven percent (n = 5) reported no difference in feeding after attending the clinic. Twenty-six percent of infants were exclusively breastfed at presentation to the clinic and 86% reported exclusive breastfeeding at follow-up. The relative risk ratio of exclusive breastfeeding after attending the clinic was 3.6 (95% confidence interval = 2.4–5.4), indicating that mothers were almost 4 times as likely to exclusively breastfeed after attending the clinic than before treatment.
Discussion
A growing amount of evidence reveals the importance to the health of both mother and baby of exclusive breastfeeding to 6 months of age and worldwide statistics show a devastatingly poor rate of success. The main problem with exclusive breastfeeding is not uptake, but continuation past the first few days and weeks. Even in a highly motivated population, mothers commonly stopped by 3 weeks of age and if they had problems in the first month, they had a high risk for discontinuing full breastfeeding. [27] When the first questionnaire was completed, over half of the infants (60%) were 4 weeks of age or less and possibly at great risk of discontinuation of breastfeeding considering their reported problems. At the time of the follow-up questionnaire, most of the infants (69%) were 12 to 24 weeks of age. Government statistics report a low rate of exclusive breastfeeding with an average of 23% at 6 weeks and 1% by the recommended length of 6 months. [1]
Our sample demonstrated that 71% of infants were solely breastfed following their intervention at the interdisciplinary clinic, which is much higher than the national UK average. An additional 15% were weaned onto solids alongside breastmilk resulting in a total of 86% of infants solely breastfeeding and no formula. This likely indicates a highly motivated population to breastfeed. However, only 26% were exclusively breastfeeding at first presentation to the clinic, showing a positive rate of change in breastfeeding after the intervention. Despite these positive findings, this type of evaluation cannot infer cause and effect, only associations. Mothers were almost 4 times more likely to exclusively breastfeed after attending the clinic than before the intervention. The narrow confidence interval suggests the results could be applicable to a wider population even though the sample size was small.
Maternal perception is essential when addressing reasons for improvement in breastfeeding rates, as continuous support, encouragement, and advice are important factors associated with successful breastfeeding. [24] This corroborates the findings from our study where 93% of mothers reported an improvement in feeding after receiving information and support from the feeding clinic. Reassurance, positive affirmation, support to attach their baby more effectively, and information about breastfeeding were well received by most mothers. In fact almost all (98%) mothers claimed that they would continue breastfeeding after the intervention. This may have enhanced the breastfeeding rates, as positive attitude and determination are associated with longer duration of breastfeeding. [19]
At the follow-up questionnaire, 93% of mothers reported being satisfied with information given at the clinic (Table 2). The high rate of breastfeeding after attending the clinic may potentially be linked with the high maternal satisfaction rates as well as the highly motivated population. One should also consider that the average appointment lasts up to an hour, which is likely longer than many other individual support alternatives. The amount of time offered with each mother is a valuable advantage that may be difficult to find and may have a positive correlation with the outcome. The hour spent with the mother in the feeding clinic may in the long term also reduce costs to the UK National Health Service. Increasing duration of breastfeeding from 1 week to 4 months can reduce childhood diseases and save the health services Ł17 million ($26 million) annually in just 4 common infant disorders, [11] demonstrating the importance and perhaps even cost-effectiveness of spending sufficient time to address all the reasons for feeding difficulty. The time also allowed for 2 types of interventions, advice for mother and physical treatment for baby.
Mothers who are encouraged by their clinician are more likely to sustain feeding beyond 12 weeks. [28] However, nonspecific, inconsistent, and conflicting advice may cause the mother distress [29] and 25% of UK mothers were critical of their postnatal care and feeding support. [13] The clinic emphasized giving positive reinforcement along with contextualized and individualized treatment and information to each mother-infant dyad attending. Nearly all of mothers reported that they understood the explanation of why they were experiencing problems. Additionally, all mothers said they had understood the explanations by the midwife and the treatment given by the chiropractor to the infant suggesting that the clinic has been transparent in these areas.
Both psychological and biophysical factors may influence early cessation of breastfeeding. [30, 31] It is therefore essential to take both aspects into consideration to address and treat the primary cause of feeding difficulties. Mothers that receive only information and support for breastfeeding technique may not get the desired result if the underlying cause is mechanical imbalance in the infant’s spine or muscles of mastication required for efficient feeding. It has been shown that infants suffering from a traumatic birth history often have dysfunctions of the spine and cranium, which can affect feeding ability. [31] A majority of infants in the clinic had an assisted birth, and evidence suggests a correlation between complicated births and early cessation of breastfeeding. [23, 31–33]
This emphasizes the importance of person-centered care in which both mother and baby are considered and that each case is treated as an individual problem. It also recognizes the fact that mothers’ feeding problems, though on the surface appearing similar, may have entirely different causes. The scope of possible problems is wide and a more generic approach such as group training and advice may not achieve the same results. The double approach of support from the midwife for the mother and treatment from the chiropractor for the baby may define a new approach that is more specific for each mother and baby.
A majority of infants presented to the clinic were diagnosed with muscular and biomechanical imbalances as well as positioning difficulties preventing them from feeding efficiently. Therefore, chiropractic care may be an important feature of management of infant’s neuromuscular dysfunction and may help improve feeding through treatments of specific biomechanical problems. [21–23, 31] One should also consider that the mothers whose infants are being treated for musculoskeletal conditions may also need information and support with attachment having adopted compromised positions to cope with suboptimal feeding. The midwives at the clinic used UNICEF guidelines in order to provide mothers with an opportunity to learn the skill independently and simultaneously enhance her self-efficacy. This interdisciplinary clinic will continue to provide this type of care to support the public health agenda to improve breastfeeding rates in society.
The results from our study generated a testable hypothesis that collaboration between these professions that provide 2 different services that complement each other could improve breastfeeding rates. Furthermore, working side by side as midwife and chiropractor provided a valuable learning experience to gain knowledge from each other’s profession and the value of working as a team. Professions working together to enhance the patient experience may be beneficial for both patient and practitioners.
Limitations
There are several limitations to this study. Even though the questionnaire was anonymous, social desirability bias may have resulted in higher satisfaction scores since the first questionnaire was completed in the clinic. Another possible limitation is that the voluntary participation may have biased the result in a positive way. Evidence suggests that nonresponders tend to be less satisfied than responders. [34] Although the follow-up response rate in this study was high (85%), one can only speculate that the nonresponders may have less positive results.
Conclusions
The preponderance of evidence suggests that breastfeeding is the optimal nutrition for infants, emphasizing the importance of finding ways to enhance breastfeeding rates and assisting mothers and babies suffering from suboptimal feeding. The results from this study demonstrate high maternal satisfaction and improved breastfeeding rates associated with attending the clinic, although no cause and effect can be determined from this type of evaluation. The outcomes indicate that a cooperative approach between midwives and chiropractors can be a useful step toward effectively addressing the issue of suboptimal feeding. A testable hypothesis resulting from a service evaluation requires future research to determine if multidisciplinary care may provide additional benefits not accrued through routine care. Improving our understanding of what type of resources are helpful to the breastfeeding dyad has potential to positively influence public health.
Acknowledgements
We would like to thank all the mothers who participated in this study and took the time to respond to our questionnaires. We would like to thank Professor Jennifer Bolton for developing the questionnaires along with Sue Way.
Author Contributions:
Alison Taylor and Joyce Miller conceived of the idea to develop the multidisciplinary clinic and the research instruments and supervised the clinic on a daily basis.
Joyce Miller conceived the idea of the student research project, developed and supervised it, developed the methods, oversaw data collection and project writing, and assisted in writing the first draft and subsequent drafts of the manuscript and submitted the manuscript.
Sue Way helped direct the clinic, developed the survey instruments, and guided the project through ethics review.
Monica Beharie facilitated and wrote the student project, helped develop the methods, collated and analyzed the data, and assisted in designing tables and writing the first draft.
Elisabeth Simmenes assisted in designing the tables and writing the first draft and subsequent drafts of the manuscript for publication.
All authors gave final approval of the manuscript.
Declaration of Conflicting Interests:
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
References:
McAndrew F, Thompson J, Fellows L, Large A, Speed M, Renfrew MJ.
Infant Feeding Survey 2010.
Leeds, England: Health and Social Care Information Centre;
http://www.hscic.gov.uk/catalogue/PUB08694/Infant-Feeding-Survey-2010
-Consolidated-Report.pdf
Published November 20, 2012. Accessed April 19, 2015.Agboado G1, Michel E, Jackson E, Verma A.
Factors associated with breastfeeding cessation in nursing mothers in a peer
support programme in Eastern LancashireBartington S, Griffiths LJ, Tate AR, Dezateux C.
Millennium Cohort Study Health Group. Are breastfeeding rates higher among
mothers delivering in Baby Friendly accredited maternity units in the UK?
Int J Epidemiol. 2006;35(suppl 5):1178–1186World Health Organization.
Infant and Young Child Feeding: Model Chapter for Textbooks for Medical Students
and Allied Health Professionals. Geneva, Switzerland:
World Health Organization;
http://www.ncbi.nlm.nih.gov/books/NBK148965/
Published 2009. Accessed January 3, 2015Entwistle FM.
The evidence and rationale for the UNICEF UK Baby Friendly Initiative standards.
http://www.unicef.org.uk/Documents/Baby_Friendly/Research/baby_friendly_
evidence_rationale.pdf
Published 2013. Accessed July 31, 2015.Ip S, Chung M, Raman G, Trikalinos TA, Lau J.
A summary of the Agency for Healthcare Research and Quality’s evidence report
on breastfeeding in developed countries.
Breastfeed Med. 2009;4(suppl 1): S17–S30Gartner LM, Morton J, Lawrence RA, et al.
Breastfeeding and the use of human milk.
Pediatrics. 2005;115:496–506Kramer MS, Kakuma R.
Optimal duration of exclusive breastfeeding.
Cochrane Database Syst Rev. 2012;(8): CD003517Bartick M, Reinhold A.
The burden of suboptimal breastfeeding in the United States:
a pediatric cost analysis.
Pediatrics. 2010;125: e1048–e1056Weimer JP.
The economic benefits of breast feeding: A review and analysis (No. 33813).
Washington, DC: US Department of Agriculture, Economic Research Service;
https://ideas.repec.org/p/ags/uersfa/33813.html
Published 2001. Accessed April 19, 2015.Renfrew MJ, Pokhrel S, Quigley M, et al.
Preventing disease and saving resources: the potential contribution of increasing
breastfeeding rates in the UK.
http://www.unicef.org.uk/Documents/Baby_Friendly/Research/
Preventing_disease_saving_resources.pdf. Published 2012
Accessed December 23, 2015.Pokhrel S, Quigley MA, Fox-Rushby J, et al.
Potential economic impacts from improving breastfeeding rates in the UK.
Arch Dis Child. 2015;100:334–340Bick D, Bastos M.
Optimising the provision and outcomes of the “Cinderella” service—
why we need to prioritise post-natal care.
Eur J Obstet Gynaecol. 2012;7(suppl 1):22–24.Brown A, Raynor P, Lee M.
Healthcare professionals’ and mothers’ perceptions of factors that influence
decisions to breastfeed or formula feed infants: a comparative study.
J Adv Nurs. 2011;67:1993–2003Ahluwalia IB, Li R, Morrow B.
Breastfeeding practices: does method of delivery matter?
Matern Child Health J. 2012;16:231–237Labarere J, Gelbert-Baudino N, Ayral AS, et al.
Efficacy of breastfeeding support provided by trained clinicians during an early,
routine, preventive visit: a prospective, randomized, open trial of 226 mother-infant pairs.
Pediatrics. 2005;115: e139–e146Renfrew MJ, McCormick FM, Wade A, Quinn B, Dowswell T.
Support for healthy breastfeeding mothers with healthy term babies.
Cochrane Database Syst Rev. 2012;(5): CD001141Sitzia J, Wood N.
Patient satisfaction: a review of issues and concepts.
Soc Sci Med. 1997;45:1829–1843Lamontagne C, Hamelin AM, St-Pierre M.
The breastfeeding experience of women with major difficulties who use
the services of a breastfeeding clinic: a descriptive study.
Int Breastfeed J. 2008;3:17 20. Stefiuk W, Green KL, Turnell R, Smith B.
Process evaluation of the Saskatoon breastfeeding center.
J Hum Lact. 2002;18:29–37Tow J, Vallone SA.
Development of an integrative relationship in the care of the breastfeeding newborn:
lactation consultant and chiropractor.
J Clin Chiropr Pediatr. 2009;10:626–632.Miller, J. E., Miller, L., Sulesund, A. K., & Yevtushenko, A.
Contribution of Chiropractic Therapy to Resolving Suboptimal Breastfeeding:
A Case Series of 114 Infants
J Manipulative Physiol Ther 2009 (Oct); 32 (8): 670–674Holleman, A. C., Nee, J., & Knaap, S. F.
Chiropractic Management of Breast-feeding Difficulties: A Case Report
Journal of Chiropractic Medicine 2011 (Sep); 10 (3): 199–203Henderson J, Redshaw M.
Midwifery factors associated with successful breastfeeding.
Child Care Health Dev. 2011;37:744–753Brain J, Schofield J, Gerrish K, et al.
A Guide for Clinical Audit, Research and Service Evaluation. Sheffield, England:
Sheffield Teaching Hospitals NHS Foundation;
www.hqip.org.uk/assets/…/Audit-Research-Service-Evaluation.pdf
Published 2011. Accessed July 25, 2014.Druijts L, Jaddoe WVW, Hofman A, Moll HA.
Prolonged and exclusive breastfeeding reduces the risk of infectious diseases in infancy.
Pediatrics. 2010;126: e18–e25Mortazavi F, Mousavi SA, Chaman R, Khosravi A.
Validation of the breastfeeding experience scale in a sample of Iranian mothers.
Int J Pediatr. 2014;2014:608657Taveras EM, Capra AM, Braveman PA, Jensvold NG, Escobar GJ, Lieu TA.
Clinician support and psychosocial risk factors associated with breastfeeding discontinuation.
Pediatrics. 2003;112:108–115Miller A, Telford A, Huizing B, et al.
What breastfeeding mothers want: specific contextualized help.
Clin Lact. 2015;6:117–123.O’Brien M, Buikstra E, Hegney D.
The influence of psychological factors on breastfeeding duration.
J Adv Nurs. 2008;63:397–408Smith LJ.
Impact of birthing practices on the breastfeeding dyad.
J Midwifery Womens Health. 2007;52:621–630Torvaldsen S, Roberts CL, Simpson JM, Thompson JF, Ellwood DA.
Intrapartum epidural analgesia and breastfeeding: a prospective cohort study.
Int Breastfeed J. 2006;1:24Lothian JA.
The birth of a breastfeeding baby and mother.
J Perinat Educ. 2005;14:42–45Crow R, Gage H, Hampson S, et al.
The measurement of satisfaction with healthcare: implications for practice from
a systematic review of the literature.
http://www.journalslibrary.nihr.ac.uk/__data/assets/pdf_file/0009/
59895/ExecutiveSummary-hta6320.pdf
Published 2002. Accessed April 19, 2015
Return to PEDIATRICS
Since 11–28–2017


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |