

Contemporary Biopsychosocial Exercise Prescription for
Chronic Low Back Pain: Questioning Core Stability
Programs and Considering ContextThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: J Can Chiropr Assoc. 2017 (Mar); 61 (1): 6–17 ~ FULL TEXT
OPEN ACCESS Peter Stilwell, B Kin, DC, MSc and Katherine Harman, PT, PhD
Dalhousie University,
5869 University Ave.
PO Box 15000
Halifax, NS B3H 4R2
ac.lad@llewlitsretep
This commentary explores the importance of considering the biopsychosocial model and contextual factors when prescribing exercise. Diverse exercise programs for patients with chronic low back pain (CLBP) produce similar outcomes, without one specific exercise protocol demonstrating clear superiority. One clear barrier to positive outcomes is poor exercise adherence. We suggest that there are certain common contextual factors present in all exercise prescription scenarios that may impact adherence and health-related outcomes. While challenging common core stability exercise prescription, we present an argument for enhancing and intentionally shaping the following contextual factors: the therapeutic alliance, patient education, expectations and attributions of therapeutic success or failure, and mastery or cognitive control over a problem. Overall, this commentary argues that to improve exercise adherence and outcomes in the CLBP population, the context in which exercise is delivered and the meaning patients embody need to be considered and shaped by clinicians.
KEYWORDS: chiropractic; chronic; exercise; low back pain; prescription
From the FULL TEXT Article:
Burden of low back pain
Low back pain (LBP) is the leading cause of disability worldwide. [1] Many individuals with a LBP episode will not be pain-free within a year, despite seeking care from a general practitioner or chiropractor. [2] Although many individuals with acute LBP (pain for less than three weeks) see improvements over time; up to 73% will have a recurrence within 12 months. [3] Individuals with chronic low back pain (CLBP; pain for greater than three months) also have poor outcomes; 60–80% of those seeking help will continue to have LBP after one year. [4] Data shows that disability from back pain has increased since the late 1990’s, despite advances in technology, improved imaging techniques, and a plethora of available passive interventions. [5] In light of this high burden, it is worthwhile to examine the effectiveness of CLBP treatments; including frequently prescribed exercise programs.
Prescribing exercise for CLBP
Exercise is one of the few interventions for CLBP that has consistently been demonstrated to reduce pain and improve function. [6] Exercise alone or in combination with education is also an effective LBP prevention strategy. [7] Although effect sizes for exercise are modest in reducing pain and improving function [8, 9] it is a desirable part of a treatment program because it is a safe self-management technique that can be performed outside of the clinical environment. As a result, it is possibly the most cost-effective and evidence-informed intervention currently available for CLBP. Unfortunately, while exercise can be effective, only a small percentage of patients with CLBP adhere to a prescribed exercise program, and poor adherence is associated with poor outcomes. [10, 11] In other words, patients have to do the exercise to reap the benefit. While there are many potential barriers to exercise adherence in patients with CLBP, diagnostic uncertainty and fear of pain or harm are among the most commonly cited. [12]
Clinicians often prescribe exercise for CLBP with a focus on biomechanics and the musculoskeletal system. This includes a focus on muscle strength, endurance, timing, or mobility. Although targeting the musculoskeletal system can lead to physical changes, current evidence suggests that these changes do not correlate well with meaningful clinical outcomes [13, 14] and these structured impairment-based programs may not facilitate long-term adherence. [12] As outlined in the next sections, a contemporary biopsychosocial approach to exercise prescription with an increased focus on clinician-patient communication and contextual factors surrounding exercise prescription may improve adherence and patient outcomes.
What type of exercise to prescribe?
Despite years of research, the active agent in therapeutic exercise for CLBP is elusive and we also lack high quality evidence to support the long-term effectiveness of one form of exercise over another for non-specific CLBP. [8, 15–25]
This includes a comparison of programs focused on:general exercise,
low back strengthening,
increasing flexibility,
improving motor control,
Pilates,
Yoga, and
various forms of aerobic exercise. [8, 15–25]To further complicate things, many clinicians, researchers, and patients may be looking in the wrong place for the beneficial effect (i.e., the musculoskeletal system). In a systematic review of exercise therapy for non-specific CLBP, Steiger and colleagues concluded that the treatment effects are not directly attributable to changes in the musculoskeletal system (e.g., muscle strength, mobility, or muscular endurance). [13] Their findings challenge long-held beliefs that exercise programs specifically targeting core stability/neuromuscular control have a regional structural or biomechanical impact and are key to successful CLBP rehabilitation. Furthermore, a systematic review of studies of transversus abdominis training for LBP patients reported that changes in muscle morphometry or activation were not associated with clinical outcomes. [14]
They also found that the relationship between clinical improvements and changes in lumbar multifidus characteristics were unclear. [14] Another study found that even when individuals with LBP were subgrouped and those with motor control impairments were identified, there was no additional benefit to prescribing ‘corrective’ motor control impairment exercises compared to a general exercise program. [19] This finding is consistent with a recent Cochrane systematic review of studies of motor control exercises for non-specific CLBP which reported that no form of exercise is superior to another. [21]
Rather than only focusing on clinician-identified musculoskeletal impairments that have questionable relevance, we hypothesize that exercises for CLBP may be better selected and taught using a biopsychosocial approach [26]; considering patients’ cognitions and self-identified functional goals or meaningful movements that have been avoided due to provoked pain or the expectation of pain. This could be combined with encouraging patients to engage in regular exercise that they expect will help and that they personally enjoy (e.g., walking in nature or yoga with meditation etc.). This is consistent with the World Health Organization (WHO) approach to disability, where a biopsychosocial approach is recommended, without making the mistake of “...reducing the whole, complex notion of disability to one of its aspects”. [27] p.9 Unfortunately, many exercise programs used in clinical practice have deep-rooted patho-anatomic underpinnings that may be hard for clinicians to change from. The concern is that outdated or unfounded unidimensional tissue-based approaches that appear ubiquitous, ignore the current biopsychosocial understanding of pain. [28] Using the example of core stability exercises for CLBP that are popular with chiropractors and other clinicians, the next section describes how there may be drawbacks to the way they are widely explained and prescribed. In turn, the benefits of viewing exercise prescription through a contemporary biopsychosocial lens and harnessing the therapeutic context may be better appreciated.
Questioning core stability exercise prescription
Popular core stability exercise programs commonly focus on bracing or activating the trunk muscles that are believed to support the spine. This includes exercises such as: crunches, planks, bird-dogs, or those aimed at specifically targeting the transversus abdominis. While it is agreed that core stability/neuromuscular control are needed to perform activities of daily living, only low levels of muscle contraction that occur beyond conscious control are needed to stabilize the spine. [29, 30] Meanwhile, current biomechanics literature demonstrates that individuals with LBP already have increased levels of abdominal and lumbar muscle activity [31], which persist despite symptom improvement. [32] With this increased muscle activity, it is of little surprise that patients with LBP have increased trunk stiffness [33], which is even higher in patients with kinesiophobia [34, 35] and catastrophizing. [36] Although this increased muscle co-contraction and trunk stiffness may provide short-term protection, in the long-term it appears to be maladaptive as it can increase lumbar spine compression and limit movement. [33, 37–39 ]
Considering this evidence, we must question the value of core stability exercise programs that promote bracing or excessively increasing trunk muscle activation, especially for CLBP patients that are exhibiting fear and guarding to avoid lumbar spine movement. Alternatively, many CLBP patients may be better instructed to perform trunk muscle relaxation techniques with movement, rather than trunk muscle activation. [40] Indeed, many contemporary approaches to core stability focus on neuromuscular control, where patients are instructed to find a balance between movement and spinal stiffness to optimally perform a task. While this is a positive step away from programs promoting excessive bracing and stiffness; still, the relationships among pain, movement, and injury remain unclear [41] and the theories of dysfunctional neuromuscular control in patients with LBP continue to be challenged. [19, 42–45]
Furthermore, the way core stability exercises are prescribed may be problematic, as it may create rather than reduce negative cognitions about the patient’s back. A systematic review with meta-analysis of stabilization exercises for LBP by Smith and colleagues found that there is strong evidence that core stability exercises are not more effective than any other form of exercise in the long-term (pain or disability) and that the rationale provided for the need of core stability could increase fear-avoidance as compared to other exercises. [22] In addition, the Military (POLM) cluster randomized trial (n = 4,147) by George et al. [46] found, as compared to traditional lumbar exercises, there was no benefit of core stability exercises for preventing the onset of LBP that resulted in healthcare seeking. Instead, a brief psychosocial education program aimed at reducing fear and threat of LBP in combination with either exercise program resulted in lower two-year incidence of healthcare seeking for LBP. These studies suggest that the context of exercise prescription is important. When anatomical explanations or words like spinal ‘weakness’ or ‘instability’ are used to explain why patients get pain or continue to have pain, the meaning patients embody may create and reinforce hyper-vigilance and enduring beliefs that the spine is vulnerable and in need of protection. [47–50]
As clinicians focus on structural explanations for persistent pain, this presents a dilemma which is nicely summarized by Moseley (2003): “However, there is a vast body of evidence to the contrary; nociception is neither sufficient nor necessary to evoke pain and psychosocial factors are more important than physical factors in the development of chronic nonspecific pain. The latter finding is reflected in management guidelines for spinal pain throughout the world.” [51] p.184 Furthermore, there is research suggesting that patients are actually quite unfamiliar with words such as ‘instability’ and ‘muscle weakness’, leading to misunderstanding. [52] This includes believing that their problem is permanent, it will progress, and that their spine can ‘go’ at any time – so they must remain on edge, expecting the worst and unable to relax. [52] As highlighted above, these beliefs may unconsciously produce more lumbar spine compression, fear-avoidance, and reduced range of motion. Once again, this demonstrates the importance of exploring the context of exercise prescription and considering the complex interplay between biological, psychological, and social factors.
Common contextual factors
If there are similar effect sizes and long-term outcomes for a large variety of exercise programs, this leads us to consider the context of exercise prescription. The context of exercise prescription may produce positive or negative effects, in addition to any specific exercise-derived musculoskeletal effects. A similar inquiry applied to psychotherapy interventions led to what is now understood as common contextual factors that are therapeutically valuable, possibly producing even more potent effects than those derived from specific intended interventions. [53, 54] Common contextual factors are clearly not limited to just psychotherapy; they are also present in the clinical encounters that chiropractors [55] and physiotherapists [56] create with their patients – they are just not commonly appreciated or discussed.
Placebo and nocebo effects
While exercise behavior change is ultimately the responsibility of the patient, clinicians can have a significant impact because “...with every utterance, the practitioner has the power to make things better or worse, and influence the outcome.” [57] p.3 The concept of common contextual factors overlap with placebo and nocebo effects. As clinicians work with patients, the context that is created can have a positive impact beyond the specific efficacy of the treatment intervention or natural fluctuations in pain and function. [58] This is commonly known also as the placebo effect. In contrast, clinicians can also promote a negative context and poor outcomes; the lesser-discussed nocebo effect. [59, 60]
Historically, the term placebo has carried negative connotations, viewed as something inert, non-specific, or fake. [58] More recently, placebo is not being viewed just as a sugar pill or an inactive ‘sham’ treatment, instead clinicians are being encouraged to embrace the contextual elements of treatment that can produce positive effects. [54, 58, 61] Indeed, Miller and Kaptchuck have suggested that the term placebo effect should be abandoned, promoting a non-stigmatized term such as ‘contextual healing’. [58] Häuser and colleagues recently published a concise and all-encompassing description of placebo and nocebo effects, stating that they can be viewed as: “...psychobiological phenomena that arise from the therapeutic context in its entirety (sham treatments, the patients’ treatment expectations and previous experience, verbal and non-verbal communications by the person administering the treatment, and the interaction between that person and the patient).” [62] p.465
While harnessing placebo effects or ‘contextual healing’ is a worthy endeavor, avoiding nocebo effects may be just as, or even more important, because the magnitude of nocebo effects in pain can be large. [63] Furthermore, the power of negative communication and nocebo in health care consultations has been suggested to be stronger than positive communication and placebo. [64] Studying placebo and nocebo effects in health care is complex, as there are many contextual factors linked to these effects. Furthermore, some patients and conditions may be more susceptible to placebo and nocebo than others. [60, 65, 66] By exploring common exercise prescription contextual factors and their possible effects, a clinician can see beyond the spine for the positive or negative impacts of their interactions and interventions.
Exploring common contextual factors
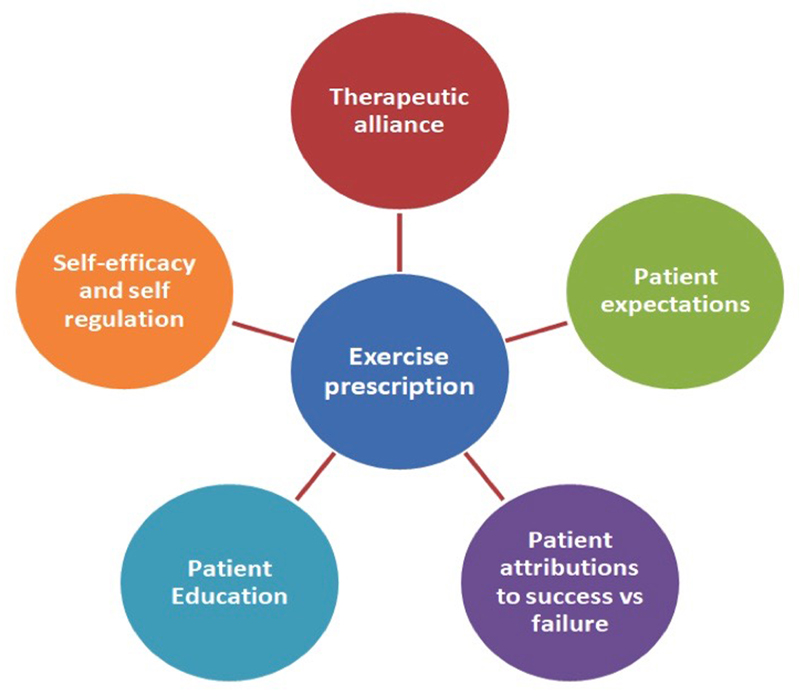
We argue that the following contextual factors can significantly impact prescribed exercise adherence and outcomes:1. The therapeutic alliance (relationship between the clinician and the patient),
2. Patient education,
3. Expectations (of therapeutic success or failure),
4. Attributions (of therapeutic success or failure), and
5. Providing an experience of mastery or cognitive control over a problem. [54]The therapeutic alliance
The therapeutic alliance has been defined as “a trusting connection and rapport established between therapist and client through collaboration, communication, therapist empathy and mutual understanding and respect”. [67] p.44 Furthermore, the therapeutic alliance is based on: collaborative goal setting, agreeing upon interventions, assigning tasks linked to goals, and bonding as rapport and trust are established. [68] Specific to chiropractic, the therapeutic alliance is known to be forged in an environment of emotional support, which fosters the growth of the belief that the problem (i.e., CLBP) is manageable [69] promoting the placebo effect. [55] As noted in Figure 1, we are suggesting that the therapeutic alliance provides the central foundation for patients to receive the benefits from other contextual factors and their placebo effects, further improving health-related outcomes and exercise adherence. Research is starting to support this as positive effects on pain and disability have been found when the therapeutic alliance is enhanced during the delivery of LBP interventions. [70–73] In contrast, the therapeutic alliance can be weakened by clinician behaviors such as discrediting and blaming a patient, or being non-supportive. [64] We hypothesize that this may stimulate potent nocebo effects, and have a negative impact on self-efficacy, exercise adherence, and patient outcomes.
Figure 1. Common contextual factor interplay.

Education
Not all education and exercise prescription are equal, as during their delivery there is potential for both placebo and nocebo effects. The following quotations from a qualitative study by Slade and colleagues [74] p.563 highlight how, in the absence of an easy explanation for CLBP, clinicians may resort to blaming past practitioners and the patient:“You’ve got to sell it, show them what they do wrong, and that’s the hardest thing” and
“It’s because you’re doing everything wrong, you’ll continue to get your back pain”. [74] p.563
Yet, they deliver their own questionable and potentially fear-inducing persistent LBP explanations and exercise advice:“I generally talk about instability... you’ve got instability at this level and your movement pattern aggravates and it’s because you’re moving through one area too much” and “We see bad movement patterns... it’s all about correcting movement patterns”. [74] p.563
This type of blaming may not only cause patient confusion, the language delivered to certain patients may elicit nocebo effects and reinforce the fear that they are failing to get better because they are incompetent and that they have something seriously wrong with their back.
Instead, explaining persistent pain using modern neuroscience approaches may not only open the door to exercise prescription, it may also improve exercise adherence and patient outcomes. [48] Pain neuroscience education resources such as Explain Pain [76] or Therapeutic Neuroscience Education [77] are becoming popular as they can help demystify and unravel the complex and sometimes unpredictable nature of CLBP. These resources provide illustrations and explanations about the neurophysiology of pain and can be used to help patients change their understanding and beliefs about the pain that they are experiencing. [78] In essence, education and learning about pain can reduce uncertainty and perceived threat, which can reduce pain. [76] We believe that patients with CLBP can then begin to view their backs as sensitized rather than fragile and prone to injury or damage. While research examining pain science education is relatively new, evidence is rapidly building that supports its use with patients experiencing CLBP. [79–84]
Expectations of therapeutic success or failure
There is a large body of literature that demonstrates the strong positive relationship between beliefs and outcomes [for review see Maddux] [85] – that is, if a patient expects they will have a positive result from a treatment, there is a strong likelihood that they will experience a positive result from that treatment. [86–89] There is also evidence that expectations can be modified to produce better intervention outcomes through placebo effects. [71, 90, 91] But we must also consider potential nocebo effects on patients. Individuals in stressful positions are vulnerable to nocebo effects [60] and living with CLBP is distressing, accompanied by a sense of loss, lowered self-worth, and fear of the future. [92] Unfortunately, as previously discussed, clinicians may create or facilitate negative expectations through poor communication or inappropriate language, which can then lead to poorer patient outcomes. [59] It is also possible that messages from the media, family, and friends could facilitate negative expectations about the back and exercise, impacting exercise adherence and health-related outcomes. When clinicians explain pain and the purpose of an exercise, “... it may be healthier to err on the side of optimism...”. [60] p.610 This is especially true with the non-specific LBP population where there is no significant underlying pathology, yet patient fear-avoidance beliefs can be high – already negatively affecting outcomes. [93] Once again, we argue that evidence-based pain neuroscience education should be used to promote positive expectations while avoiding nocebo effects (e.g., pain does not equal damage, the back is inherently strong, and the spine/nervous system is adaptable).
Attributions of therapeutic success or failure
Attributions are an individual’s explanation or understanding of why things have occurred the way they did – it is a way of making sense of past experiences. [54] Attributions help us to create a useful understanding of the world, as far as we can predict or control events. [94] When an intervention is judged as a success or failure in the past, it shapes expectations of success/failure for similar interventions in the future. [85] Another important impact of attribution is on the strength or stability of treatment outcomes. If a patient believes that their improvement was due to what a clinician did, then any beneficial effect is significantly shorter than if a patient believes that they improved because of their own actions. [54] Furthermore, people act on their beliefs, [95] if a patient attributes their back pain to the fact that their spine is unstable or weak, and they are educated on how they are failing to do an exercise properly, it should not be a surprise that they would expect to get worse if they engaged in exercise or load their spine. This type of unintended nocebo effect created by clinicians is clearly demonstrated in the following quote from a study by Darlow and colleagues:“Basically all I’ve kind of been told to do by physios is to work on my core...I’ve been tested by various different physios, and Pilates, and I’m apparently ridiculously weak .... I had an abortion because I didn’t think I could have a baby. I didn’t think I could handle it...carrying it, and having extra weight on my stomach.” [47] p.532
This last quote may be an extreme example of how education can shape attributions and expectations, and how these beliefs can shape behaviors. Still, as highlighted above, the increased use of individualized approaches that facilitate positive beliefs about the back and empower patients with CLBP is clearly needed.
Mastery or cognitive control over a problem
Mastery is defined as “control over those circumstances that importantly bear on the life of the individual”. [96] p.164 In the context of musculoskeletal rehabilitation, both cognitive and physical control is needed to achieve mastery - which often requires deliberate practice with performance feedback. [97–100] Emerging neuroscience research suggests that positive neuroplastic changes appear to be enhanced by slowly increasing the complexity of motor skill tasks, promoting cognitive effort and learning. [101] This process is thought of as ‘working through’ the new behavior while paying attention to thoughts and responses to the movement. [54] With practice, patients can learn and believe that they are capable of consistently overcoming their challenging movement tasks, which can increase their self-efficacy and result in mastery. [95] These ideas are supported by findings in a recent synthesis of systematic reviews that identified self-efficacy as one of the most consistent predictors of exercise participation. [102] Furthermore, a reciprocal relationship between improved exercise adherence and self-efficacy has been demonstrated. Simply put: participation in exercise tends to increase exercise self-efficacy, which in turn reinforces exercise behavior and continued exercise participation. [103] Positive beliefs are a key feature in self-efficacy and mastery, but they can also modulate the placebo effect. [104]
This suggests that if an exercise is expected by a patient to reduce pain and improve function, the patient is not only more likely to do it, they are also more likely to derive benefit from it. In contrast, the potential for nocebo effects through conditioning and expectation should also be considered. If a patient repeatedly fails when attempting their meaningful movement task(s) and the clinician provides poor education and negative comments, such as telling them how they move wrong, their spine is unstable, or how a passive ‘fix’ is the key to success – the end result can be something like learned helplessness. [105] This occurs when a patient feels that they do not have control over their situation and their pain, and that they only make things worse when they try to help themselves, so they give up.
We believe that once the patients’ self-identified movement goals are achieved, they should be encouraged to engage in regular exercise that they expect will help and that they personally enjoy. Here, patient preferences should be key considerations when prescribing exercise. When a patient can select the exercise they enjoy and/or expect will help, the beneficial effects of the exercise may not only be potentiated through expectations/placebo effects [104], but also through improved practice/adherence, leading to improved self-efficacy and mastery. [106] Research supports this idea, as it has been found that incorporating patient preference and tailoring treatment programs to patients is associated with improved self-management adherence and health-related outcomes. [107, 108]
The complex positive feedback loop in Figure 1 can now be better appreciated; a strong therapeutic alliance with effective education can promote placebo effects, while avoiding nocebo effects. We argue that positive changes in attribution and expectations can then result in exercise engagement, which can feed forward into increased exercise self-efficacy and mastery.
Conclusion
Evidence keeps building about the multi-system benefits of exercise [109]; this includes therapeutic exercise for chronic low back pain (CLBP). As suggested throughout this commentary, a focus on gross biological changes alone (muscle strength, endurance etc.) has limited value. Instead, more research is needed to examine the interplay between biological, psychological, and social factors - as this may have novel exercise prescription implications for patients with CLBP. This commentary provided an overview of some of the contextual factors that have biopsychosocial implications. It was described how these contextual factors can facilitate placebo or nocebo effects, impacting patients’ behaviors and outcomes. The therapeutic alliance was presented as an important foundation, impacting patient education, expectations and attributions of therapeutic success or failure, and the patient’s sense of mastery or control. Current evidence suggests that a strong therapeutic alliance, pain neuroscience education, and incorporating the functional needs and preferences of the patient can positively impact patients’ beliefs and behaviors. Overall, this commentary suggests that to improve exercise adherence and health-related outcomes in the CLBP population, the context in which exercise is delivered and the meaning patients embody need to be carefully considered and shaped by clinicians. More research is needed to further define and measure the active components within the common contextual factors presented in this commentary, as well as others factors shaping patients’ exercise beliefs and behaviors.
Acknowledgments
We would like to thank and acknowledge Dr. Warren Hefford, Selena Glover, and Marsha MacRae for providing feedback on an early draft of this commentary.
References:
Global Burden of Disease 2013 Collaborators (2013)
Global, Regional, and National Incidence, Prevalence, and Years Lived with Disability for 301 Acute
and Chronic Diseases and Injuries in 188 Countries, 1990-2013: A Systematic Analysis
for the Global Burden of Disease Study 2013
Lancet. 2015 (Aug 22); 386 (9995): 743–800Kongsted, A, Kent, P, Hestbaek, L, and Vach, W.
Patients With Low Back Pain Had Distinct Clinical Course Patterns
That Were Typically Neither Complete Recovery Nor Constant Pain.
A Latent Class Analysis of Longitudinal Data
Spine J. 2015 (May 1); 15 (5): 885–894Pengel LH, Herbert RD, Maher CG, et al.
Acute low back pain: systematic review of its prognosis.
BMJ. 2003;327(7410):323Hayden JA, Dunn KM, Van der windt DA, et al.
What is the prognosis of back pain?
Best Pract Res Clin Rheumatol. 2010;24(2):167–179Deyo RA, Mirza SK, Turner JA, Martin BI.
Overtreating Chronic Back Pain: Time to Back Off?
J Am Board Fam Med. 2009 (Jan); 22 (1): 62–68Chou R, Huffman LH; American Pain Society.
Nonpharmacologic Therapies for Acute and Chronic Low Back Pain:
A Review of the Evidence for an American Pain Society/
American College of Physicians Clinical Practice Guideline
Annals of Internal Medicine 2007 (Oct 2); 147 (7): 492–504Steffens D, Maher CG, Pereira LS, et al.
Prevention of Low Back Pain: A Systematic Review and Meta-analysis
JAMA Intern Med. 2016 (Feb); 176 (2): 199–208van Middelkoop M, Rubinstein SM, Verhagen AP, et al.
Exercise Therapy for Chronic Nonspecific Low-back Pain
Best Pract Res Clin Rheumatol. 2010 (Apr); 24 (2): 193–204Keller A, Hayden J, Bombardier C, et al.
Effect sizes of non-surgical treatments of non-specific low-back pain.
Eur Spine J. 2007;16(11):1776–1788Beinart NA, Goodchild CE, Weinman JA, et al.
Individual and intervention-related factors associated with adherence to home exercise in chronic low back pain: a systematic review.
Spine J. 2013;13(12):1940–1950Cecchi F, Pasquini G, Paperini A, et al.
Predictors of response to exercise therapy for chronic low back pain: result of a prospective study with one year follow-up.
Eur J Phys Rehabil Med. 2014;50(2):143–151Slade SC, Patel S, Underwood M, et al.
What Are Patient Beliefs and Perceptions About Exercise for Nonspecific Chronic Low Back Pain?
A Systematic Review of Qualitative Studies
Clin J Pain. 2014 (Nov); 30 (11): 995–1005Steiger F, Wirth B, de Bruin ED, et al.
Is a positive clinical outcome after exercise therapy for chronic non-specific low back pain contingent upon a corresponding improvement in the targeted aspect(s) of performance? A systematic review.
Eur Spine J. 2012;21(4):575–598Wong AY, Parent EC, Funabashi M, et al.
Do changes in transversus abdominis and lumbar multifidus during conservative treatment explain changes in clinical outcomes related to nonspecific low back pain? A systematic review.
J Pain. 2014;15(4):377.e1–e35Aleksiev AR.
Ten-year follow-up of strengthening versus flexibility exercises with or without abdominal bracing in recurrent low back pain.
Spine. 2014;39(24):1495–1497Macedo LG, Maher CG, Latimer J, et al.
Motor control exercise for persistent, nonspecific low back pain: a systematic review.
Phys Ther. 2009;89(1):9–25Macedo LG, Smeets RJ, Maher CG, et al.
Graded activity and graded exposure for persistent nonspecific low back pain: a systematic review.
Phys Ther. 2010;90(6):860–879O’Keeffe M, Nolan D, O’Sullivan P, et al. Re: Aleksiev AR.
Ten-year follow-up of strengthening versus flexibility exercises with or without abdominal bracing in recurrent low back pain.
Spine. 2014;39(24):E1495–1497Saner J, Kool J, Sieben JM, et al.
A Tailored Exercise Program Versus General Exercise for a Subgroup of
Patients with Low Back Pain and Movement Control Impairment:
A Randomised Controlled Trial with One-year Follow-up
Manual Therapy 2015;20(5):672–679Shnayderman I, Katz-leurer M.
An aerobic walking programme versus muscle strengthening programme for chronic low back pain: a randomized controlled trial.
Clin Rehabil. 2013;27(3):207–214Saragiotto BT, Maher CG, Yamato TP, et al.
Motor control exercise for chronic non-specific low-back pain.
Cochrane Database Syst Rev. 2016;1:CD012004Smith BE, Littlewood C, May S.
An update of stabilisation exercises for low back pain: a systematic review with meta-analysis.
BMC Musculoskelet Disord. 2014;15:416van der Giessen RN, Speksnijder CM, Helders PJ.
The effectiveness of graded activity in patients with non-specific low-back pain: a systematic review.
Disabil Rehabil. 2012;34(13):1070–1076Haavik, H and Murphy, B.
The Role of Spinal Manipulation in Addressing Disordered Sensorimotor Integration and
Altered Motor Control
J Electromyogr Kinesiol. 2012 (Oct); 22 (5): 768–776Yamato TP, Maher CG, Saragiotto BT, et al.
Pilates for low back pain.
Cochrane Database Syst Rev. 2015;2(7):CD010265O’Sullivan K, Dankaerts W, O’Sullivan L, et al.
Cognitive functional therapy for disabling nonspecific chronic low back pain: multiple case-cohort study.
Phys Ther. 2015;95(11):1478–1488World Health Organization .
International Classification of Functioning, Disability and Health (ICF)
Geneva: 2001.Melzack R, Katz J.
Pain.
Wiley Interdiscip Rev Cogn Sci. 2013;4(1):1–15Cholewicki J, Panjabi MM, Khachatryan A.
Stabilizing function of trunk flexor-extensor muscles around a neutral spine posture.
Spine. 1997;22(19):2207–2212Lederman E.
The myth of core stability.
J Bodyw Mov Ther. 2010;14(1):84–98Ghamkhar L, Kahlaee AH.
Trunk muscles activation pattern during walking in subjects with and without chronic low back pain: a systematic review.
PMR. 2015;7(5):519–526Moreside JM, Quirk DA, Hubley-Kozey CL.
Temporal patterns of the trunk muscles remain altered in a low back-injured population despite subjective reports of recovery.
Arch Phys Med Rehabil. 2014;95(4):686–698Hodges P, van den Hoorn W, Dawson A, et al.
Changes in the mechanical properties of the trunk in low back pain may be associated with recurrence.
J Biomech. 2009;42(1):61–66Karayannis NV, Smeets RJ, van den Hoorn W, et al.
Fear of movement is related to trunk stiffness in low back pain.
PLoS ONE. 2013;8(6):e67779Massé-Alarie H, Beaulieu LD, Preuss R, et al.
Influence of chronic low back pain and fear of movement on the activation of the transversely oriented abdominal muscles during forward bending.
J Electromyogr Kinesiol. 2016;27:87–94Pakzad M, Fung J, Preuss R.
Pain catastrophizing and trunk muscle activation during walking in patients with chronic low back pain.
Gait Posture. 2016;49:73–77Butler HL, Hubley-Kozey CL, Kozey JW.
Changes in electromyographic activity of trunk muscles within the sub-acute phase for individuals deemed recovered from a low back injury.
J Electromyogr Kinesiol. 2013;23(2):369–377Geisser ME, Haig AJ, Wallbom AS, et al.
Pain-related fear, lumbar flexion, and dynamic EMG among persons with chronic musculoskeletal low back pain.
Clin J Pain. 2004;20(2):61–69Marras WS, Ferguson SA, Burr D, et al.
Spine loading in patients with low back pain during asymmetric lifting exertions.
Spine J. 2004;4(1):64–75Wong AY, Parent EC, Prasad N, et al.
Does experimental low back pain change posteroanterior lumbar spinal stiffness and trunk muscle activity? A randomized crossover study.
Clin Biomech (Bristol, Avon) 2016;34:45–52Hodges PW, Smeets RJ.
Interaction between pain, movement, and physical activity: short-term benefits, long-term consequences, and targets for treatment.
Clin J Pain. 2015;31(2):97–107Allison GT, Morris SL.
Transversus abdominis and core stability: has the pendulum swung?
Br J Sports Med. 2008;42(11):930–931Gubler D, Mannion AF, Schenk P, et al.
Ultrasound tissue Doppler imaging reveals no delay in abdominal muscle feed-forward activity during rapid arm movements in patients with chronic low back pain.
Spine. 2010;35(16):1506–1513Laird RA, Kent P, Keating JL.
Modifying patterns of movement in people with low back pain -does it help? A systematic review.
BMC Musculoskelet Disord. 2012;13:169Mehta R, Cannella M, Henry SM, et al.
Trunk postural muscle timing is not compromised in low back pain patients clinically diagnosed with movement coordination impairments.
Motor Control. 2015 In PressGeorge SZ, Childs JD, Teyhen DS, et al.
Brief Psychosocial Education, Not Core Stabilization, Reduced Incidence of Low Back Pain:
Results from the Prevention of Low Back Pain in the Military (POLM) Cluster Randomized Trial
BMC Medicine 2011 (Nov 29); 9: 128Darlow B, Dowell A, Baxter GD, et al.
The enduring impact of what clinicians say to people with low back pain.
Ann Fam Med. 2013;11:527–534Darlow B, Dean S, Perry M, et al.
Easy to harm, hard to heal.
Spine. 2015;40(11):842–850Domenech J, Sánchez-Zuriaga D, Segura-Ortí E, et al.
Impact of biomedical and biopsychosocial training sessions on the attitudes, beliefs, and recommendations of health care providers about low back pain: a randomised clinical trial.
Pain. 2011;152(11):2557–2563Nijs J, Roussel N, Wilgen C, et al.
Thinking beyond muscles and joints: Therapists’ and patients’ attitudes and beliefs regarding chronic musculoskeletal pain are key to applying effective treatment.
Man Ther. 2013;18:96–102Moseley L.
Unraveling the barriers to reconceptualization of the problem in chronic pain: the actual and perceived ability of patients and health professionals to understand the neurophysiology.
J Pain. 2003;4(4):184–189Barker KL, Reid M, Minns Lowe CJ.
Divided by a lack of common language? A qualitative study exploring the use of language by health professionals treating back pain.
BMC Musculoskelet Disord. 2009;10(123):1–10Rosenzweig S.
Some implicit common factors in diverse methods of psychotherapy.
Am J Orthopsych. 1936;6:412–415.Weinberger J.
Common factors aren’t so common: the common factors dilemma.
Clin Psych Sci Pract. 1995;2(1):45–69.Jamison JR.
Nonspecific intervention in chiropractic care.
J Manipulative Physiol Ther. 1998;21(6):423–425Miciak M, Gross DP, Joyce A.
A review of the psychotherapeutic ‘common factors’ model and its application in physical therapy: the need to consider general effects in physical therapy practice.
Scand J Caring Sci. 2012;26(2):394–403Mason P, Butler C.
Health Behavior Change: A Guide for Practitioners. Second edition.
Churchill Livingston; Edinburgh: 2010.Miller F, Kaptchuk T.
The power of context: reconceptualizing the placebo effect.
JRSM. 2008;101(5):222–225Bingel U.
Avoiding nocebo effects to optimize treatment outcome.
JAMA. 2014;312(7):693–694Hahn R.
The nocebo phenomenon: concept, evidence and implications for public health.
Prevent Med. 1997;26:607–611Howick J, Friedemann C, Tsakok M, et al.
Are treatments more effective than placebos? A systematic review and meta-analysis.
PLoS ONE. 2013;8(5):e62599Häuser W, Hansen E, Enck P.
Nocebo phenomena in medicine: their relevance in everyday clinical practice.
Dtsch Arztebl Int. 2012;109(26):459–465Petersen GL, Finnerup NB, Colloca L, et al.
The magnitude of nocebo effects in pain: a meta-analysis.
Pain. 2014;155(8):1426–1434Greville-Harris M, Dieppe P.
Bad is More Powerful Than Good: The Nocebo Response in Medical Consultations
American Journal of Medicine 2015 (Feb); 128 (2): 126–129Hashmi JA, Kong J, Spaeth R, et al.
Functional network architecture predicts psychologically mediated analgesia related to treatment in chronic knee pain patients.
J Neurosci. 2014;34(11):3924–3936Hashmi JA, Baria AT, Baliki MN, et al.
Brain networks predicting placebo analgesia in a clinical trial for chronic back pain.
Pain. 2012;153(12):2393–2402Cole MB, McLean V.
Therapeutic relationships re-defined.
Occ Ther Mental Health. 2003;19(2):33–56.Bordin E.
The generalizability of the psychoanalytic concept of the working alliance.
Psychother. 1979;16(3):252–260.Jamison JR.
Reflections on chiropractic’s patient-centered care.
J Manipulative Physiol Ther. 2001;24(7):483–486Ferreira PH, Ferreira ML, Maher CG, et al.
The therapeutic alliance between clinicians and patients predicts outcome in chronic low back pain.
Phys Ther. 2013;93:470–478Fuentes J, Armijo-Olivo S, Funabashi M, et al.
Enhanced therapeutic alliance modulates pain intensity and muscle pain sensitivity in patients with chronic low back pain: an experimental controlled study.
Phys Ther. 2014;94(4):477–489Hall AM, Ferreira PH, Maher CG, et al.
The influence of the therapist-patient relationship on treatment outcome in physical rehabilitation: a systematic review.
Phys Ther. 2010;90:1099–1110Lewis M, Morley S, van der Windt DA, et al.
Measuring practitioner/therapist effects in randomised trials of low back pain and neck pain interventions in primary care settings.
Eur J Pain. 2010;14:1033–1039Slade SC, Molloy E, Keating JL.
The dilemma of diagnostic uncertainty when treating people with chronic low back pain: a qualitative study.
Clin rehab. 2012;26(6):558–569Nijs J, Meeus M, Cagnie B, et al.
A Modern Neuroscience Approach to Chronic Spinal Pain: Combining Pain Neuroscience Education
with Cognition-targeted Motor Control Training
Phys Ther. 2014 (May); 94 (5): 730–738Butler DS, Moseley G.
Explain Pain.
Adelaine City West:
Noigroup Publications; 2003.Louw A, Puentedura E.
Therapeutic neuroscience education: teaching patients about pain: a guide for clinicians.
International Spine and Pain Institute. 2013Moseley GL, Butler DS.
Fifteen years of explaining pain: the past, present, and future.
J Pain. 2015;16(9):807–813Moseley GL.
Combined physiotherapy and education is effective for chronic low back pain. A randomised controlled trial.
Aust J Physioth. 2002;48:297–302Moseley GL.
Joining forces - combining cognition-targeted motor control training with group or individual pain physiology education: a successful treatment for chronic low back pain.
J Man Manip Therap. 2003;11:88–94.Moseley GL.
Evidence for a direct relationship between cognitive and physical change during an education intervention in people with chronic low back pain.
Eur J Pain. 2004;8:39–45Moseley GL, Nicholas MK, Hodges PW.
A randomized controlled trial of intensive neurophysiology education in chronic low back pain.
Clin J Pain. 2004;20:324–330Pires D, Cruz EB, Caeiro C.
Aquatic exercise and pain neurophysiology education versus aquatic exercise alone for patients with chronic low back pain: a randomized controlled trial.
Clin Rehabil. 2015;29(6):538–547Ryan CG, Gray HG, Newton M, et al.
Pain biology education and exercise classes compared to pain biology education alone for individuals with chronic low back pain: a pilot randomized controlled trial.
Man Ther. 2010;15:382–387Maddux J.
Expectancies and the social-cognitive perspective: basic principles, processes and variables.
In: Kirsch I, editor.
How Expectancies Shape Experience.
Washington, DC: American Psychological Association; 1999.Iles R, Davidson M, Taylor N, et al.
Systematic review of the ability of recovery expectations to predict outcomes in non-chronic non-specific low back pain.
J Occup Rehabil. 2009;19(1):25–40Mondloch M, Cole D, Frank J.
Does how you do depend on how you think you’ll do? A systematic review of the evidence for a relation between patients’ recovery expectations and health outcomes.
CMAJ. 2001;165(2):174–179George S, Robinson M.
Preference, expectation, and satisfaction in a clinical trial of behavioral interventions for acute and sub-acute low back pain.
J Pain. 2010;11(11):1074–1082Smeets R, Beelen S, Goossens M, et al.
Treatment expectancy and credibility are associated with the outcome of both physical and congitive-behavioural treatment in chronic low back pain.
Clin J Pain. 2008;24(4):305–315Crum AJ, Langer EJ.
Mind-set matters: exercise and the placebo effect.
Psychol Sci. 2007;18(2):165–171Wulf G, Chiviacowsky S, Lewthwaite R.
Altering mindset can enhance motor learning in older adults.
Psychol Aging. 2012;27(1):14–21Snelgrove S, Liossi C.
Living with chronic low back pain: a metasynthesis of qualitative research.
Chronic Illn. 2013;9(4):283–301Wertli MM, Rasmussen-Barr E, Weiser S, et al.
The role of fear avoidance beliefs as a prognostic factor for outcome in patients with nonspecific low back pain: a systematic review.
Spine J. 2014;14(5):816–836. e4Anderson C, Krull D, Weiner B.
Explanations: Proceeses and Consequences.
In: Higgins E, Kruglanski A, editors.
Social Psychology: Handbook of Basic Principles.
New York: Guilford; 1996.Bandura A.
Self-Efficacy: The Exercise of Control.
New York: W.H. Freeman; 1997.Pearlin LI, Nguyen KB, Schieman S, et al.
The life-course origins of mastery among older people.
J Health Soc Behav. 2007;48:164–179Ericsson KA, Krampe RT, Tesch-Römer C.
The role of deliberate practice in the acquisition of expert performance.
Psych Rev. 1993;100(3):363–406.Ericsson KA.
Deliberate practice and acquisition of expert performance: a general overview.
Acad Emerg Med. 2008;15(11):988–994Kitago T, Krikauer J.
Motor learning principles for neurorehabilitation.
In: Barnes M, Good D, editors.
Neurological Rehabilitation. Elsevier; 2013.Winstein C, Lewthwaite R, Blanton S, et al.
Infusing motor learning research into neurorehabilitation practice: a historical perspective with case exemplar from the accelerated skill acquisition program.
J Neurol Phys Ther. 2014;38:190–200Boudreau SA, Farina D, Falla D.
The role of motor learning and neuroplasticity in designing rehabilitation approaches for musculoskeletal pain disorders.
Man Ther. 2010;15(5):410–414Bauman AE, Reis RS, Sallis JF, et al.
Correlates of physical activity: Why are some people physically active and others not?
Lancet. 2012;380(9838):258–271Weinberg RS, Gould D.
Foundations of sport and exercise psychology. 3rd ed.
Champaign, IL: Human Kinetics; 2003.Stewart-Williams S, Podd J.
The placebo effect: dissolving the expectancy versus conditioning debate.
Psychol Bull. 2004;130(2):324–340Roland M, Jenner J.
Back Pain: New Approaches to Rehabilitation and Education.
Manchester Univ Pr. 1989Harman K, MacRae M, Vallis M, et al.
Working with people to make changes: a behavioural change approach used in chronic low back pain rehabilitation.
Physiother Can. 2014;66(1):82–90Lorig K, Holman HR.
Self-management education: History, definition, outcomes, and mechanisms.
Ann Behav Med. 2003;26(1):1–7Peek K, Sanson-Fisher R, Carey M, et al.
Physiother. 2015. Interventions to aid patient adherence to physiotherapist prescribed self-management strategies: a systematic review.
In PressPedersen BK, Saltin B.
Exercise as medicine - evidence for prescribing exercise as therapy in 26 different chronic diseases.
Scand J Med Sci Sports. 2015;25(Suppl 3):1–72

Return to LOW BACK PAIN
Return to EXERCISE AND CHIROPRACTIC
Since 2-16-2018


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |