

First Provider Seen for an Acute Episode of
Low Back Pain Influences Subsequent
Health Care UtilizationThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: Physical Therapy 2023 (Jun 28); 103 (9): pzad067 ~ FULL TEXT
OPEN ACCESS Christopher G Bise, PT, MS, DPT • Michael Schneider, DC, PhD • Janet Freburger, PT, PhD,
G Kelley Fitzgerald, PT, PhD • Galen Switzer, PhD • Garry Smyda, BS,
Pamela Peele, PhD • Anthony Delitto, PT, PhD
School of Health and Rehabilitation Science,
Department of Physical Therapy,
University of Pittsburgh.
Objective: Costs associated with low back pain (LBP) continue to rise. Despite numerous clinical practice guidelines, the evaluation and treatments for LBP are variable and depend largely on the individual provider. As yet, little attention has been given to the first choice of provider. Early research indicates that the choice of first provider and the timing of interventions for LBP appear to influence utilization. This study sought to examine the association between the first provider seen and utilization.
Methods: Using 2015-2018 data from a large insurer, this retrospective analysis focused on patients (29,806) seeking care for a new episode of LBP. The study identified the first provider chosen and examined the following year of medical utilization. Cox proportional hazards models were calculated using inverse probability weighting on propensity scores to evaluate the time to event and the relationship to the first choice of provider.
Results: The primary outcome was the timing and utilization of health care resources. Total health care utilization was lowest in those who first sought care with chiropractic care or physical therapy. Highest health care utilization was seen in those patients who chose the emergency department.
Conclusion: Overall, there appears to be an association between the first choice of provider and future health care utilization. Chiropractic care and physical therapy provide nonpharmacologic and nonsurgical, guideline-based interventions. Their participation appears related to a decrease in immediate and long-term utilization of health care resources. This study expands the existing body of literature and provides a compelling case for the influence of the first provider on an acute episode of LBP.
Impact: The first provider seen for an acute episode of LBP influences immediate treatment decisions, the trajectory of a specific patient episode, and future health care choices in the management of LBP.
Keywords: Economics; Health Care Costs; Low Back Pain; Quality Assurance: Health Care; Utiilzation Review.
From the FULL TEXT Article:
Introduction
In 2012, 126.6 million US adults (54%) reported the presence of a musculoskeletal condition. The most frequent complaint was low back pain (LBP). LBP accounts for 2.5% to 3.0% of all physician visits in the United States with annual expenditures in excess of $85 billion. [1, 2] In 2014, the direct per person costs to treat LBP were estimated at $9,035, with total aggregate direct costs estimated at $315,000,000. [3] Adoption of clinical practice guidelines (CPG) has been sub-optimal at best, [4-6] with considerable variation in treatments based on clinician preference or, in some cases, the simple availability of 1 test over another. [4, 7–12] Current treatment strategies are fraught with imaging, injections, surgery, and opioid prescriptions, [13, 14] with opioids still the most commonly prescribed medication for LBP. [4, 15]
Emerging research suggests the first provider seen and the timing of interventions for LBP influence health care utilization. [16, 17] Early studies were limited by small sample sizes, the number of providers studied, and a focus on patients with private health insurance. [17] More recently, Garrity et al [18] and Frogner et al [19] analyzed the impact of direct access to physical therapy. Garrity found that unrestricted direct access to physical therapy had significantly lower costs at 30 and 90 days. Additionally, provisional direct access to physical therapists had significantly increased rates of imaging and additional physician visits. [18] The instrumental variable analysis performed by Frogner et al supported these findings, showing significantly lower probability of receiving opioid prescriptions, advanced imaging, and emergency department (ED) visits. [19] Our study extends previous work by including patients with public and private insurance, increasing the number of provider types considered as the initial point of contact, and increasing sample size. The purpose of this study was to examine the association between patient choice of first provider and health care use in the 12 months after their index visit.
Methods
Data Source/Study Design
Data were extracted from a large health insurance plan serving 1.7 million beneficiaries. Products offered by this health plan included commercial insurance, Medicaid managed care, and Medicare Advantage. Using the available data, we conducted a retrospective analysis of patients seeking care for a new (acute) episode of LBP during the period from July 1, 2015, to June 30, 2018.
Cohort Identification
We identified patients using an extensive list of ICD-9/10 (Suppl. Appendix A) codes related to the diagnosis of LBP. To meet the definition of an acute episode, patients needed to have no claims with an associated LBP-related ICD-9/10 code for 3 months before their index visit. Three months was used as a “clean period” based on literature surrounding “resolution” of acute LBP. [20, 21] Three months of continuous health plan enrollment before the index visit and 12 months of continuous enrollment after the index visit were required for episode identification and analysis. Inclusion required that one of the identified LBP codes be in the primary billing position at the index visit. Claims were excluded if the patient did not meet continuous enrollment requirements or was younger than 18 years old. Claims were excluded in the presence of a code at the time of the index visit indicating pregnancy or evidence of serious pathology or disease, [22-25] including metastatic disease, cauda equina, spinal infection, ankylosing spondylitis, or fracture (Suppl. Appendix B).
Study Variables
Our independent variable was the first contact each patient had with the health care system. We termed this the “portal of entry.” A combination of point of service codes and internal financial services subgroup codes identified the following providers as independent variables: (1) Emergency Department (ED); (2) primary care; (3) surgery (orthopedics or neurosurgery); (4) specialty care (rheumatology, physiatry, or pain management); (5) chiropractic care; (6) physical therapy; or (7) other. Patients in the “other” category were unattributed or attributed to a provider that comprised <1% of the final sample (Suppl. Appendix C).
Demographics included age, gender, and insurance coverage (Medicare, Medicaid, or commercial). Covariates included mean (age-adjusted) Charlson Co-Morbidity index (CCI) score and indicators for individual CCI conditions, including congestive heart failure, peripheral vascular disease, chronic obstructive pulmonary disease, diabetes, hypertension, anxiety, and depression. [26] Additional covariates included self-reported body mass index >30 (yes/no), serious persistent mental illness (SPMI) (yes/no), and high health care use (yes/no). SPMI is defined as individuals diagnosed with schizophrenic disorders, episodic mood disorders, or borderline personality disorders based on ICD-9/ICD-10 codes (Suppl. Appendix D) over the previous 12-month period. High resource users were identified by using insurance company internal predictive models that identify members at risk for increased health care utilization. These models flag members with spending above a threshold and/or with escalating utilization. The model uses claims, pharmacy, and demographic data from the previous 12 months to predict whether use will continue to escalate or remain above the spending threshold over the following 12 months. Members with end-stage renal disease, transplant, and cancer are excluded from the models as they are expected to have high spending and use.
We created several dependent variables representing the amount and type of health care use occurring in the 12 months following the index visit. Using point of service codes, diagnostic-related group codes, and CPT-4 codes, we identified a specific service (one of our variables), whether it was associated with a LBP code, and when it occurred. “Episode length” was operationalized as the time from the date of the index visit to the date of the last claim with a LBP diagnosis code. An episode was considered “resolved” when a patient had 90 days without a claim. We used dichotomous outcomes (yes, no) to indicate the presence of an opioid prescription, specialist referrals (visit to orthopedics, neurosurgery, physical medicine, and rehabilitation, and/or pain management, spinal injections, and surgical intervention). High-tech imaging included magnetic resonance imaging (MRI) or computed tomography (CT) use. Low-tech imaging included radiographs. Unplanned care use was defined as subsequent use of the ED. An opioid prescription related to LBP was operationalized using pharmacy claims. When a prescription is filled, the fill date and the date the prescription was written are loaded into the claim. When the date the prescription was written coincided with a visit claim date that had an LBP-related diagnosis code, that prescription was associated with the current LBP episode. Time-to-event variables were created and operationalized as “time in days” from the index visit to the first claim with an LBP diagnosis and the variable.
We considered both total medical use and low back–related medical use in the subsequent year. Costs were calculated using United States dollars and included the index visit. Total cost of care (TCOC) was the benefit allowed amount, including copays, for medical and pharmacy claims for 365 days following the index visit, while LBP-related costs were the TCOC for medical and pharmacy claims with associated LBP diagnosis codes.
Other outcomes included opioid prescription, specialist referral (visit to orthopedics, neurosurgery, physical medicine and rehabilitation, and/or pain management), high-tech imaging (including MRI or CT), low-tech imaging (radiograph), spinal injection, additional ED use, and progression to surgical intervention. Additional description of study variables can be found in Supplemental Appendix E.
Data Analysis
Descriptive analyses were completed and stratified by first choice of provider (ED, primary care, surgery, specialty care, chiropractic care, physical therapy, and other). We calculated adjusted cumulative incidence and time to event curves for each outcome. Finally, we calculated hazard ratios for each of these outcomes using Cox proportional hazards models. Proportional hazard assumptions were met, and Kaplan Meier curves are available for review in Supplemental Appendix F. Because the selection of first provider can be influenced by observed and unobserved baseline characteristics, we attempted to account for the systematic differences in the populations that choose each provider. Traditionally, researchers have used regression adjustments or structural approaches to address selection bias. [27] Recently, more contemporary methods have evolved incorporating time to event outcomes and hazard ratios. Because our secondary outcomes were overwhelmingly time to event outcomes, we chose inverse probability of treatment weighting. Austin et al found that survival curves can be used to estimate each group (or in our case, first provider) separately with the simple weighting and “distribution” of baseline covariates: “the use of the ‘crude’ Kaplan–Meier estimator can allow for an unbiased comparison of survival between treatment (or exposure) groups.” [28] In our study, propensity scores were generated using a multinomial logistic regression to determine the probability of an individual choosing 1 provider over another. Initial diagnosis, baseline demographics, and all covariates were included in the multinomial model. Primary care was the reference group because more than 50% of patients chose this as their primary portal of entry, and many payment models use primary care as the preferred entry point into the health care system. Use of this technique results in “an artificial treatment population,” where the first choice of provider remains independent from the baseline measures. [29]
Mean and median costs were calculated independently for each portal of entry and for both total medical costs (TCOC) and those costs that were linked to the episode via a low back code in the first billing position. The 95% CIs were calculated using means, whereas interquartile range was calculated for median costs.
Results
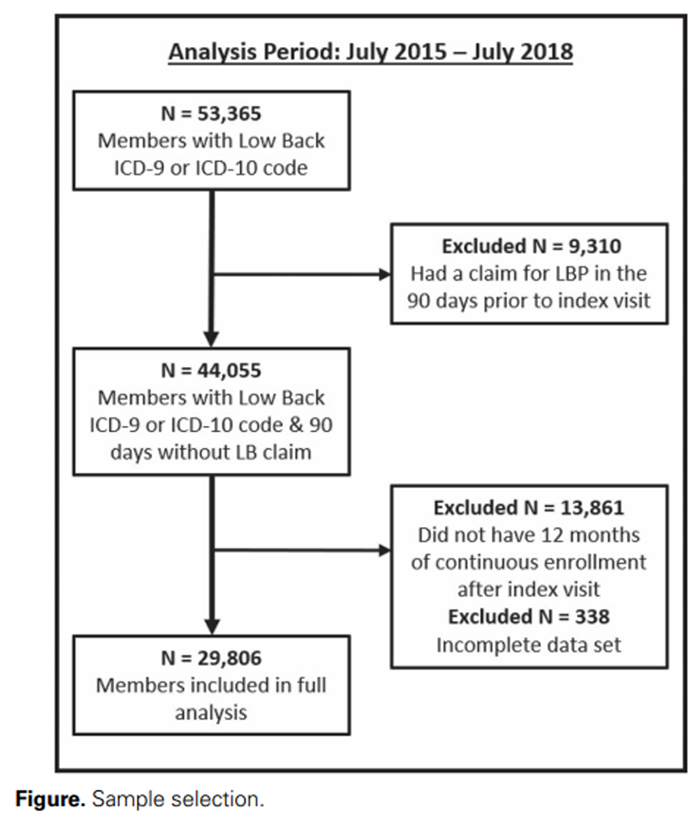
Figure

Table 1
page 4

Table 2
page 5The final sample consisted of 29,806 participants with a health care visit for acute LBP from July 1, 2015, to June 30, 2018 (Figure). The top 3 portals of entry, primary care (n = 15,199; 51%), chiropractic care (n = 4971; 17%), and the ED (n = 2895; 10%), accounted for over 75% of the patients (Table 1). Younger patients tended to choose chiropractic care, whereas females chose specialty care and physical therapy. Comorbid health burden, estimated using age-adjusted CCI, was highest in those who chose surgery or the ED. Comorbid health burden was lowest in the chiropractic care group. Members with mental health disorders (anxiety, depression, SPMI) were more likely to choose a surgeon or the ED. In terms of spending, those who chose specialty care had increased potential (14%) for increased utilization over the next year compared with chiropractic care (5.4%).
Episode Length
Patients who entered through the ED, chiropractic care, and physical therapy had the shortest median episode length at 35 days (ED interquartile range [IQR] = 10, 79; chiropractic care IQR = 10, 95) and 37 days (physical therapy IQR = 18, 7). Those who entered through specialty care had the longest median length of episode at 68 days (IQR = 30, 136) (Table 2).
Costs of Care
The average TCOC for all medical costs was lowest in those who first sought care with chiropractic care ($7,761; 95% CI = $7,306–$8,218) or physical therapy ($11,612; 95% CI = $10,586–$12,638). The highest average TCOC for all medical costs was seen in those patients who chose the ED ($20,028; 95% CI = $18,903–$21,154) and those who entered through surgery ($17,825; 95% CI = $16,794–$18,857). Similarly, when costs were limited to claims associated with LBP codes, the lowest average spending occurred in chiropractic care ($992; 95% CI = $913–$1,072) and physical therapy ($1,925; 95% CI = $1,689–$2,161), whereas the highest LBP-related spending was seen in surgery ($4,346; 95% CI = $3,870–$4,821) and the ED ($3,382; 95% CI = $3,102–$3,661) (Tab. 2).
Radiography (Low-Tech Imaging)
Radiography use was highest in those members who had first contact with a surgeon or a primary care provider (PCP). A total of 61% of those who saw a surgeon and 47% of those who saw their PCP would undergo a radiograph within 30 days following the index visit. In contrast, 6% of those who saw a physical therapist and 19% who saw a chiropractor received a radiograph in the first 30 days. During the next year, just over 24% of those who sought physical therapy or chiropractic care would receive a radiograph compared with over 70% for those who saw a surgeon and 60% for those who saw their PCP. In terms of risk, individuals seen in the surgical setting were 1.46 times (95% CI = 1.43–1.49) more likely to receive a radiograph than those seen by their PCP. Hazard ratios were lower than 0.5 for all other providers (Tab. 2).
CT/MRI (High-Tech Imaging)

Table3
page 6A total of 49% of those who chose primary care or surgery as their first provider received a CT or MRI in the 30 days following the index event. A total of 65% of those who chose primary care or surgery would receive a CT or MRI in the year following the index visit. In contrast, only 3% of those who entered through chiropractic care and 9% of those who entered through physical therapy received a CT or MRI in the first 30 days. MRI/CT use was greatest in the primary care group because hazard ratios for all providers relative to primary care were <1.00. Patients receiving chiropractic care and physical therapy had the lowest risk of receiving an MRI/CT, at any time in the subsequent year, with hazard ratios of 0.09 (95% CI = 0.08–0.1) and 0.26 (95% CI = 0.26–0.27), respectively (Table 3).
Injections
A total of 55% of individuals who entered through specialty care received an injection compared with <5% of those choosing chiropractic care and 15% of those choosing physical therapy. Relative to primary care, the risk of receiving an injection increased 2.2 times (95% CI = 2.16–2.26) when the first provider was specialty care. Entry through the ED increased the risk of injection by 1.2 times at any point during the next year (95% CI = 1.21–1.27) (Tab. 3).
Opioid Prescribing
Opioid prescription rates were highest for those who chose the ED (55%) and specialty care (39%). Rates were lowest for those who chose chiropractic care (5%) and physical therapy (11%). We found that, compared with first contact with primary care, those who chose the ED had a 2.82 (95% CI = 2.75–2.90) higher risk of filling an opioid prescription at any point during the year following the index visit. A total 21% of those prescriptions were filled on the day of the index visit (Day 1), with 33% filling a prescription in the first 30 days. Those who entered through specialty care were 1.58 (95% CI = 1.54–1.63) times more likely to receive an opioid prescription, with 18% filling that prescription on the day of the index visit. Those who chose surgery, physical therapy, and chiropractic care were less likely to receive an opioid prescription compared with primary care. Hazard ratios were <1.0 for physical therapy (0.39; 95% CI = 0.37–0.40), chiropractic care (0.13; 95% CI = 0.12–0.14), and surgery (0.90; 95% CI = 0.88–0.92) groups (Tab. 3).
Surgery
In our sample, fewer than 7% of those who initiated care at surgery, and 4% of those who chose the ED progressed to surgery over the next 12 months. In contrast, those who sought care from a chiropractor or physical therapist had significantly lower rates of surgical intervention. Those who chose chiropractic care progressed to surgery <1% of the time, and just over 1% of those who chose physical therapy required surgical intervention. Those who chose surgery first doubled their risk (2.0; 95% CI = 1.90–2.22) of undergoing a low back–related surgical procedure over the next year. Patients who used the ED had the second highest risk of surgical intervention (1.2; 95% CI = 1.10–1.31) (Tab. 3).
Specialty Referral
Specialty referral was defined as a referral to orthopedic surgery, neurosurgery, physical medicine and rehabilitation, rheumatology, or pain management. Referral to a specialist at any point during the next year was highest for the surgery group (1.66; 95% CI = 1.63–1.70) and the specialty care group (1.79; 95% CI = 1.76–1.83). This is likely because these portals of entry continued to manage members who chose them as their initial provider of choice. All other providers had hazard ratios <1.00, indicating rates of referral less than that of the reference group (Tab. 3).
Unplanned Care Use
Unplanned care use was highest in those members who chose the ED first. Over 30% of those who chose the ED would have an additional LBP-related visit to the ED. Members who chose the ED as their first contact provider were 5 times more likely to use the ED for a low back–related claim at any time during the year following their index visit (5.64; 95% CI = 5.35–5.93). All other portals of entry (except the “other” group) had hazard ratios <1.00, indicating rates of use less than that of the primary care reference group (Tab. 3).
Discussion
The purpose of this study was to investigate the impact that patient choice of first provider has on medical use in patients with an acute episode of LBP. As in previous studies, [17, 30] the most common entry points into the system were primary care, chiropractic care, and the ED. Those who chose chiropractic care and physical therapy first had lower risks of use for all outcomes. Additionally, chiropractic care and physical therapy had the lowest TCOC and low back–related medical spending. These 2 groups, however, have some unique characteristics that make them different from other portals of entry.
First, these providers are not medical doctors. Neither has prescribing rights and, during the timeframe under analysis, only chiropractors could provide or refer for imaging. This naturally forces physical therapists and chiropractors to choose nonsurgical interventions. Second, many medical providers seek a “pathoanatomic diagnosis.” The pathoanatomic diagnosis rarely drives interventions used by physical therapists. The timing of care also appears to be an issue. Patients can seek physical therapy and chiropractic care at any time during an episode, even while receiving care from other providers. Emerging evidence suggests that those patients who choose physical therapy and chiropractic care early in an episode have improved outcomes and lower costs compared with other providers. [16, 17, 31] Data continue to suggest that these 2 professions, when accessed early in the course of care, provide cost-effective, nonsurgical management strategies for LBP that align with CPG’s.
Of particular concern was the volume of patients filling a prescription for opioids. A total of 34% of our total sample would fill at least 1 prescription for opioids within the year following their index visit. A total of 38% of those who used the ED as their entry point would fill a prescription on Day 1, with 50% of patients filling a prescription within the next 30 days. Although these rates seem high, they are similar to previously studied cohorts. [30] These rates are not however, in line with past and current CPG’s. [32-34]
Utilization of MRI/CT was just as concerning. The American College of Physicians and the American Pain Society joint CPG recommends “clinicians should not routinely obtain imaging or other diagnostic tests in patients with nonspecific LBP.” [35] These guidelines also state “diagnostic imaging and testing for patients with LBP should only be used when severe or progressive neurologic deficits are present or when serious underlying conditions are suspected on the basis of history and physical examination.” [34] Since we excluded emergent LBP codes from our data set, emergent imaging should have been minimized. What we found however, was that 51% of the total population received an MRI/CT in the year following their index visit. Of those who received imaging, 29% of those images occurred on the day of the index visit. A total of 73% of MRI/CTs would occur within the first 30 days. That equates to 36% of our entire patient population being imaged within the 30 days following their index visit. When we break this down by provider type, 65% of those members who saw their PCP or a surgeon as the first provider would get an MRI over the next year. An argument might be made for the surgery cohort, as surgeons use MRI in their decision making about those patients who are appropriate for surgery. The rates in primary care, however, are confusing and warrant further investigation. In contrast, utilization rates of MRI in the physical therapy and chiropractic groups are significantly lower than other providers. Overall, there appears to be a lack of concordance between current CPGs and chosen interventions or referrals. This indicates that despite increased attention, there is still much work to be done with dissemination and implementation of best practice standards. [34-36]
Findings from this study appear to indicate that the first provider seen for an acute episode of LBP influences immediate health care utilization. What has been unclear to this point is the impact the initial choice of provider has on utilization over time. Our data show a relationship between the initial choice of provider and the interventions used, the initial costs incurred, and those medical costs related to the treatment of LBP for the subsequent 12 months after the index visit.
We identified several strengths and limitations in this study. Compared with previous studies, this study substantially increased heterogeneity and overall sample size. Though the increase in heterogeneity could be considered a limitation, the use of an expanded code set better represents the actual population of those with back pain coming into the system. After controlling for nefarious conditions such as cancer and fracture (Suppl. Appendix B), we’re left with the true representation of non-emergent back pain. This is clearly a source of selection bias based on symptom severity, but we attempted to control for this using treatment weighted propensity scoring. There was also concern surrounding with the inclusion of osteomyelitis and discitis rather than excluding them as emergent conditions. Though we do not consider them “emergent conditions,” their treatment pathways may deviate significantly than those with what would be considered “traditional” low back pain. A more homogenous cohort may give use the behavior of specific conditions, but it would also decrease the generalizability. Unfortunately, our conclusions were limited by the use of administrative claims data. Our data, though robust, contains no clinical information, which could clearly influence a patient’s choice of practitioner and a practitioner’s choice of intervention. This results in an inability to assess clinical outcomes and limits insights to utilization trends. Additionally, because of the administrative database queried, we cannot reliably attribute all events to any 1 specific provider. For example, if an individual is seen in the ED and has an MRI 7 days later, we cannot determine who ordered the MRI; only that the patient received the service.
Another potential limitation was our cost analysis. The focus of this study was to identify patterns of utilization, providers, and timing. The cost analysis we provided was unadjusted and may have therefore been influenced by the makeup of the individual groups. However, even with this potential confounder, we still found, in post hoc analysis, higher utilization and higher costs within certain first provider groups.
Finally, our data does not consider populations with no insurance, those with catastrophic coverage or those choosing to pay out of pocket. Because our data is claims based, and these patients would pay out of pocket, there would be no claim to identify this group. There is information available indicating that these populations are accessing the health system, but their provider of choice may not be represented in this study. [37] The behavior of this group may be vastly different than their partially of fully insured counterparts. Moreover, for those patients with insurance, benefit structure may influence patient choice. Many commercial plans have large co-pays that discourage patients from accessing certain providers or services. Medicaid, in contrast, has no co-pay. The low reimbursement rates however may create a financial disincentive for providers to accept patients with Medicaid. Finally, access and availability of services directly influences utilization. These influences can all be considered forms of selection bias. Despite the use of statistical methods to control for potential bias, we cannot fully eliminate the impact of selection bias on this study.
Notwithstanding these limitations, there are substantial strengths in this study. Previous analyses were limited by their use of primarily commercial data [30, 38, 39] or data derived from smaller health systems. [17] We analyzed claims from a health plan that has public and commercial lines of business. The size of the insurer and the number of active members allow for specific inclusion criteria while still providing a robust sample size. The inclusion of all payors allowed for a better representation of the those who may present to specific types of providers, reducing selection bias. Additionally, the use of an exhaustive code set allowed us to capture a more inclusive picture of the impact of LBP on our population and better represent coding practices that may vary from physician office to office.
This study offers compelling evidence that the first provider seen for an acute episode of LBP influences the trajectory of a specific patient episode and future health care utilization. Furthermore, it appears that per episode costs for low back care and total medical spending for year following the index visit are also influenced by the choice of first contact provider. As health care resources continue to dwindle, we need to consider more efficient and cost-effective strategies to manage patients with LBP. Implementation strategies should be multi-faceted, aimed at behavior change, and involve increased use of nonsurgical and non-opioid interventions. Given that chiropractic care and physical therapy provide nonpharmacologic and nonsurgical interventions that promote behavior change, significant consideration should be given to these practitioners as first-line providers of care for LBP. Their participation appears related to a decrease in both immediate and long-term utilization of health care resources.
Supplementary Material
Author Contributions
Concept/idea/research design: C.G. Bise, M. Schneider, J. Freburger, G.K. Fitzgerald, G. Switzer, P. Peele, A. Delitto
Writing: C.G. Bise, M. Schneider, J. Freburger, A. Delitto
Data collection: C.G. Bise, P. Peele
Data analysis: C.G. Bise, M. Schneider, G. Smyda, P. Peele
Project management: C.G. Bise
Providing facilities/equipment: A. Delitto
Providing institutional liaisons: A. Delitto
Consultation (including review of manuscript before submitting): M. Schneider, J. Freburger, G.K. Fitzgerald, G. Switzer, P. Peele, A. Delitto
References:
Martin, BI, Deyo, RA, Mirza, SK et al.
Expenditures and Health Status Among Adults With Back and Neck Problems
JAMA 2008 (Feb 13); 299 (6): 656–664Deyo RA, Mirza SK, Martin BI.
Back pain prevalence and visit rates:
estimates from U.S. national surveys, 2002.
Spine. 2006;31:2724–2727.
https://doi.org/10.1097/01.brs.0000244618.06877.cd.Yellin EH, Watkins-Castillo SI.
Direct medical costs. BMUS: The Burden of Musculoskeletal Diseases in the United States.
Accessed March 13, 2017.
https://www.boneandjointburden.org/
fourth-edition/iia0/low-back-and-neck-painIvanova JI, Birnbaum HG, Schiller M, Kantor E, Johnstone BM, Swindle RW.
Real-world practice patterns, health-care utilization, and costs in patients
with low back pain: the long road to guideline-concordant care.
Spine J. 2011;11:622–632.
https://doi.org/10.1016/j.spinee.2011.03.017.Williams CM, Maher CG, Hancock MJ et al.
Low Back Pain and Best Practice Care: A Survey of General Practice Physicians
Archives of Internal Medicine 2010 (Feb 8); 170 (3): 271–277Epstein-Sher S, Jaffe DH, Lahad A.
Are they complying? Physicians’ knowledge, attitudes, and readiness
to change regarding low back pain treatment guideline adherence.
Spine. 2017;42:247–252.
https://doi.org/10.1097/BRS.0000000000001714.Graves JM, Fulton-Kehoe D, Jarvik JG, Franklin GM.
Health Care Utilization and Costs Associated with Adherence to Clinical
Practice Guidelines for Early Magnetic Resonance Imaging among
Workers with Acute Occupational Low Back Pain
Health Serv Res. 2014 (Apr); 49 (2): 645–665Nunn ML, Hayden JA, Magee K.
Current management practices for patients presenting with
low back pain to a large emergency department in Canada.
BMC Musculoskelet Disord. 2017;18:92.
https://doi.org/10.1186/s12891-017-1452-1.Drazin D, Nuńo M, Patil CG, Yan K, Liu JC, Acosta FL.
Emergency room resource utilization by patients with low-back pain.
J Neurosurg Spine. 2016;24:686–693.
https://doi.org/10.3171/2015.7.SPINE14133.Mundkur ML, Rough K, Huybrechts KF et al.
Patterns of opioid initiation at first visits for pain
in United States primary care settings.
Pharmacoepidemiol Drug Saf. 2018;27:495–503.
https://doi.org/10.1002/pds.4322.Barnett ML, Olenski AR, Jena AB.
Opioid-prescribing patterns of emergency physicians and risk of long-term use.
N Engl J Med. 2017;376:663–673.
https://doi.org/10.1056/NEJMsa1610524.Stewart WF, Yan X, Boscarino JA et al.
Patterns of health care utilization for low back pain.
J Pain Res. 2015;8:523–535.
https://doi.org/10.2147/JPR.S83599.Webster BS, Verma SK, Gatchel RJ.
Relationship between early opioid prescribing for acute occupational
low back pain and disability duration, medical costs,
subsequent surgery and late opioid use.
Spine. 2007;32:2127–2132.
https://doi.org/10.1097/BRS.0b013e318145a731.Webster BS, Choi Y, Bauer AZ, Cifuentes M, Pransky G.
The cascade of medical services and associated longitudinal costs
due to nonadherent magnetic resonance imaging for low back pain.
Spine. 2014;39:1433–1440.
https://doi.org/10.1097/BRS.0000000000000408.Gore M, Sadosky A, Stacey BR, et al.
The Burden of Chronic Low Back Pain: Clinical Comorbidities,
Treatment Patterns, and Health Care Costs in Usual Care Settings
Spine (Phila Pa 1976). 2012 (May 15); 37 (11): E668–677Karvelas DA, Rundell SD, Friedly JL et al.
Subsequent health-care utilization associated with early physical
therapy for new episodes of low back pain in older adults.
Spine J. 2017;17:380–389.
https://doi.org/10.1016/j.spinee.2016.10.007.Fritz JM, Kim J, Dorius J.
Importance of the Type of Provider Seen to Begin Health Care
for a New Episode Low Back Pain: Associations
with Future Utilization and Costs
J Eval Clin Pract. 2016 (Apr); 22 (2): 247–252Garrity BM, McDonough CM, Ameli O et al.
Unrestricted direct access to physical therapist services is associated
with lower health care utilization and costs in patients
with new-onset low back pain.
Phys Ther. 2020;100:107–115.
https://doi.org/10.1093/ptj/pzz152.Frogner BK, Harwood K, Andrilla CHA, Schwartz M, Pines JM.
Physical therapy as the first point of care to treat low back pain:
an instrumental variables approach to estimate impact on
opioid prescription, health care utilization, and costs.
Health Serv Res. 2018;53:4629–4646.
https://doi.org/10.1111/1475-6773.12984.da Silva T, Macaskill P, Mills K et al.
Predicting recovery in patients with acute low back pain:
a clinical prediction model.
Eur J Pain. 2017;21:716–726.
https://doi.org/10.1002/ejp.976.Downie, AS, Hancock, MJ, Rzewuska, M, Williams, CM, Lin, CW, and Maher, CG.
Trajectories of Acute Low Back Pain: A Latent Class Growth Analysis
Pain. 2016 (Jan); 157 (1): 225–234Verhagen AP, Downie A, Popal N, Maher C, Koes BW.
Red flags presented in current low back pain guidelines: a review.
Eur Spine J. 2016;25:2788–2802.
https://doi.org/10.1007/s00586-016-4684-0.Henschke N, Maher CG, Refshauge KM et al.
Prevalence of and screening for serious spinal pathology in patients
presenting to primary care settings with acute low back pain.
Arthritis Rheum. 2009;60:3072–3080.
https://doi.org/10.1002/art.24853.Strudwick K, Nelson M, Martin-Khan M, Bourke M, Bell A, Russell T.
Quality indicators for musculoskeletal injury management
in the emergency department: a systematic review.
Acad Emerg Med. 2015;22:127–141.
https://doi.org/10.1111/acem.12591.Strudwick K, McPhee M, Bell A, Martin-Khan M, Russell T.
Review article: best practice management of low back pain in the emergency department
(part 1 of the musculoskeletal injuries rapid review series).
Emerg Med Australas. 2018;30:18–35.
https://doi.org/10.1111/1742-6723.12907.Charlson M, Wells MT, Ullman R, King F, Shmukler C.
The Charlson Comorbidity Index can be used prospectively
to identify patients who will incur high future costs.
PLoS One. 2014;9:e112479.
https://doi.org/10.1371/journal.pone.0112479.Austin PC.
An introduction to propensity score methods for reducing
the effects of confounding in observational studies.
Multivar Behav Res. 2011;46:399–424.
https://doi.org/10.1080/00273171.2011.568786.Austin PC.
The use of propensity score methods with survival or time-to-event outcomes:
reporting measures of effect similar to those used in randomized experiments.
Stat Med. 2014;33:1242–1258.
https://doi.org/10.1002/sim.5984.Austin PC, Stuart EA.
Moving towards best practice when using inverse probability of treatment
weighting (IPTW) using the propensity score to estimate causal
treatment effects in observational studies.
Stat Med. 2015;34:3661–3679.
https://doi.org/10.1002/sim.6607.Azad TD, Vail D, Bentley J et al.
Initial provider specialty is associated with long-term opiate use
in patients with newly diagnosed low back and lower extremity pain
Spine (Phila Pa 1976) 2019 (Feb 1); 44 (3): 211-218Fritz JM, Childs JD, Wainner RS, Flynn TW.
Primary care referral of patients with low back pain to physical therapy:
impact on future health care utilization and costs.
Spine. 2012;37:2114–2121.
https://doi.org/10.1097/BRS.0b013e31825d32f5.Dowell D, Haegerich TM, Chou R.
CDC guideline for prescribing opioids for chronic pain - United States, 2016.
MMWR Recomm Rep. 2016;65:1–49.
https://doi.org/10.15585/mmwr.rr6501e1.Chou R, Deyo R, Friedly J, Skelly A, Hashimoto R, Weimer M, et al.
Nonpharmacologic Therapies for Low Back Pain: A Systematic Review
for an American College of Physicians Clinical Practice Guideline
Annals of Internal Medicine 2017 (Apr 4); 166 (7): 493–505Chou R, Qaseem A, Snow V, Casey D, Cross JT Jr., Shekelle P, Owens DK:
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline
from the American College of Physicians and the American Pain Society
Annals of Internal Medicine 2007 (Oct 2); 147 (7): 478–491Qaseem A, Wilt TJ, McLean RM, Forciea MA;
Noninvasive Treatments for Acute, Subacute, and Chronic Low Back Pain:
A Clinical Practice Guideline From the American College of Physicians
Annals of Internal Medicine 2017 (Apr 4); 166 (7): 514–530Chou R, Deyo RA, Jarvik JG.
Appropriate use of lumbar imaging for evaluation of low back pain.
Radiol Clin N Am. 2012;50:569–585.
https://doi.org/10.1016/j.rcl.2012.04.005.Barnett JC, Vornovitsky MS.
Health Insurance Coverage in the United States: 2015
Current Population Reports, P60-257(RV)
U.S. Government Printing Office, Washington, DC, 2016.Kim LH, Vail D, Azad TD, et al.
Expenditures and Health Care Utilization Among Adults
with Newly Diagnosed Low Back and Lower Extremity Pain
JAMA Network Open 2019 (May 3); 2 (5): e193676Garber AM, Azad TD, Dixit A et al.
Medicare savings from conservative management of low back pain
Am J Manag Care. 2018 (Oct 1); 24 (10): e332–e337
Return to INITIAL PROVIDER/FIRST CONTACT
Since 6-28-2023


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |